Gout is a disease that involves the deposit of monosodium urate (MSU) crystals, which mostly affects men, and constitutes the most common cause of arthritis in that gender. On occasion, it can lead to accumulations of crystals of variable size and location referred to as tophi. Considered to be a “mimicking” disease, gout can simulate, among others, infectious or neoplastic processes. We report the case of a patient with gout who developed an osteosarcoma arising at the site of a preexisting tophus.
The patient was a 65-year-old man with tophaceous gout who had been followed at another center and was referred to us by way of the medical oncology department for the management an acute attack of polyarthralgia and olecranon bursitis after a transfusion while undergoing chemotherapy. He had been diagnosed a year earlier with osteosarcoma on the dorsum of his foot arising at the location of a tophus that had been removed 7 months before, after pathological confirmation (Fig. 1) and negative findings in the study of the extension. It required infracondylar amputation and preoperative and postoperative chemotherapy with cisplatin and adriamycin. He had been taking allopurinol for 3 years (up to 300mg/day), and employed colchicine and/or nonsteroidal anti-inflammatory drugs during attacks. He had levels of uric acid in blood of up to 8mg/dL, and began to have symptoms at the age of 40 years with podagra, and later developed tophi in the olecranon bursa and the dorsum of his foot. The inflammatory attack was resolved with low-dose prednisone and aspiration of the olecranon bursa. Gram staining and culture of the fluid obtained were negative, and a study with polarized light microscopy revealed the presence of MSU crystals. He was discharged and began colchicine at 1mg/day after gradual interruption of prednisone therapy. During follow-up, he changed from allopurinol to febuxostat (at a dose of 80mg/day), which achieved optimization of his uric acid level in blood and progressive dissolution of the olecranon tophi. Several months later, colchicine was discontinued and he continued to take febuxostat at the same dose. He has not had any further attacks and maintains his level of uric acid at 5mg/dL. In May of 2016, he developed an “in-transit” recurrence of the neoplastic disease, with a superficial mass in ipsilateral thigh that required local resection and chemotherapy (ifosfamide).
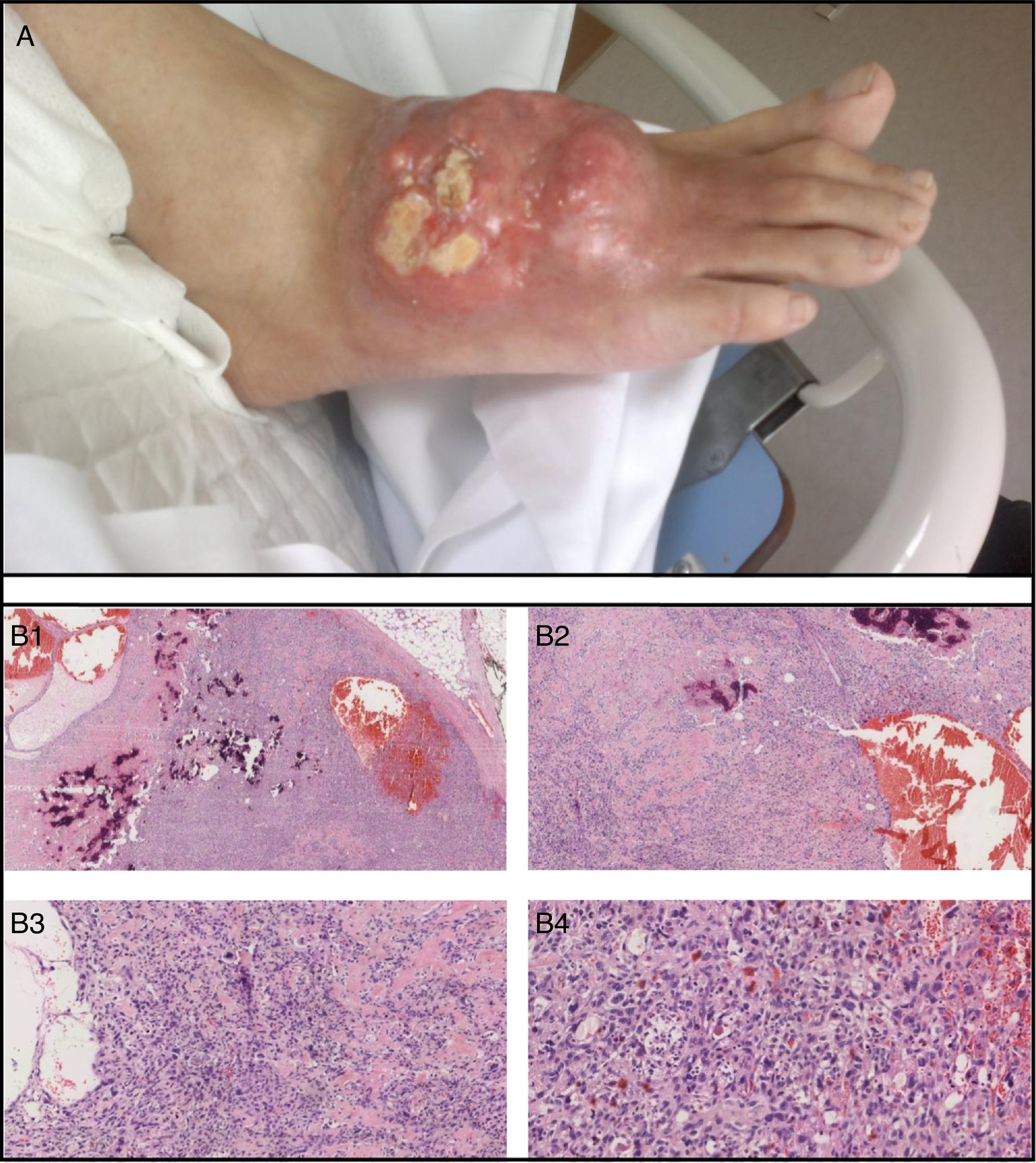
High-grade osteosarcoma on the dorsum of right foot in a patient with tophaceous gout. (A) Macroscopic description: tumor-like infiltrated erythematous violaceous plaque measuring 6cm in maximum diameter, composed of hard tumor nodules, with the consistency of bone and petrified. The surface consisted of excrescent tumor lesions that were slightly pedicled measuring about 3cm in diameter. (B) Microscopic description (hematoxylin and eosin [H&E]; from upper left to right and lower left to right: B1: H&E 2×; B2: H&E 4×; B3: H&E 10×; B4: H&E 20×). Telangiectatic osteosarcoma, with abundant osteoid formation and blood-filled spaces and no epithelial lining. At high magnification, it is possible to observe large cells with irregular and pleomorphic nuclei, and numerous mitoses, many atypical.
Gout is the most common cause of arthritis in men, and is originated by deposits of MSU crystals in tissues. Some patients develop tophi (subcutaneous, periarticular or intraarticular crystal accumulations) which can have a marked inflammatory activity and present calcifications or ossifications as they increase in size.1–3 Moreover, tophi can mimic infectious or neoplastic processes and become superinfected or undergo malignant transformation, having an adverse effect on the prognosis of the patient.
A number of publications have reported tumors that arise at the sites of tophi.4–9 All occurred in extremities of middle-aged or elderly men and involved recurrences or metastasis. There are descriptions of benign neoplasms such as giant cell tumors or malignant diseases such as different sarcomas (undifferentiated pleomorphic sarcoma, cutaneous angiosarcoma or fibrosarcoma).
The authors of these articles provide interesting hypotheses such as the role of prolonged hyperuricemia and the severity of the MSU deposit as factors leading to secondary cell transformation toward inflammation,8 or the theory of sarcoma associated with a foreign body, similar to those originated by other materials.7,10
Sarcomas are mesenchymal tumors originating from connective tissue (fibrosarcoma), cartilage (chondrosarcoma), bone (osteosarcoma), endothelium (angiosarcoma), etc. Although there may be a certain underestimation of the incidence of these neoplasms in gout, sarcomas seem to be uncommon, but occasionally are aggressive. Thus, they should be included in the differential diagnosis in the case of a subcutaneous or periarticular mass in a patient with gout or with the atypical complication of a preexisting tophus.
To the Pathology and Medical Oncology Departments of Grupo HM Hospitales, Madrid, Spain.
Please cite this article as: Calvo Aranda E, Rodríguez Pérez I, Rodríguez-Pascual J, García de la Peña Lefebvre P. Osteosarcoma en gota tofácea: descripción de un caso clínico y revisión de la literatura. Reumatol Clin. 2017;13:307–309.



![High-grade osteosarcoma on the dorsum of right foot in a patient with tophaceous gout. (A) Macroscopic description: tumor-like infiltrated erythematous violaceous plaque measuring 6cm in maximum diameter, composed of hard tumor nodules, with the consistency of bone and petrified. The surface consisted of excrescent tumor lesions that were slightly pedicled measuring about 3cm in diameter. (B) Microscopic description (hematoxylin and eosin [H&E]; from upper left to right and lower left to right: B1: H&E 2×; B2: H&E 4×; B3: H&E 10×; B4: H&E 20×). Telangiectatic osteosarcoma, with abundant osteoid formation and blood-filled spaces and no epithelial lining. At high magnification, it is possible to observe large cells with irregular and pleomorphic nuclei, and numerous mitoses, many atypical. High-grade osteosarcoma on the dorsum of right foot in a patient with tophaceous gout. (A) Macroscopic description: tumor-like infiltrated erythematous violaceous plaque measuring 6cm in maximum diameter, composed of hard tumor nodules, with the consistency of bone and petrified. The surface consisted of excrescent tumor lesions that were slightly pedicled measuring about 3cm in diameter. (B) Microscopic description (hematoxylin and eosin [H&E]; from upper left to right and lower left to right: B1: H&E 2×; B2: H&E 4×; B3: H&E 10×; B4: H&E 20×). Telangiectatic osteosarcoma, with abundant osteoid formation and blood-filled spaces and no epithelial lining. At high magnification, it is possible to observe large cells with irregular and pleomorphic nuclei, and numerous mitoses, many atypical.](https://static.elsevier.es/multimedia/21735743/0000001300000005/v1_201708230012/S2173574317300965/v1_201708230012/en/main.assets/thumbnail/gr1.jpeg?xkr=ue/ImdikoIMrsJoerZ+w937trqSwLGgTrQM2QjUSRyU=)


