The antisynthetase syndrome, defined in 1990,1 is characterized by the presence of antisynthetase antibodies, inflammatory myopathy, interstitial lung disease, mechanic's hands, arthritis, fever and Raynaud's phenomenon.
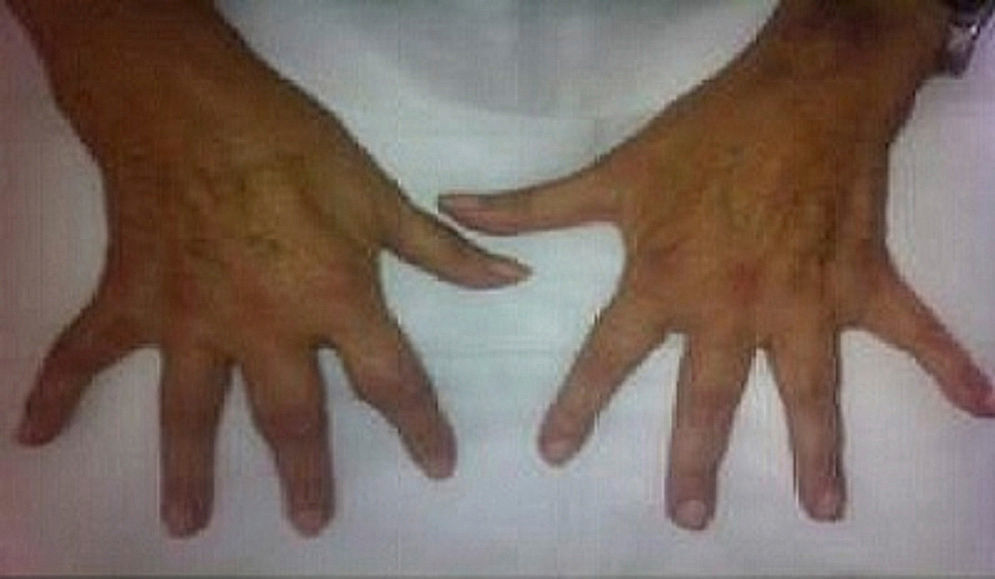
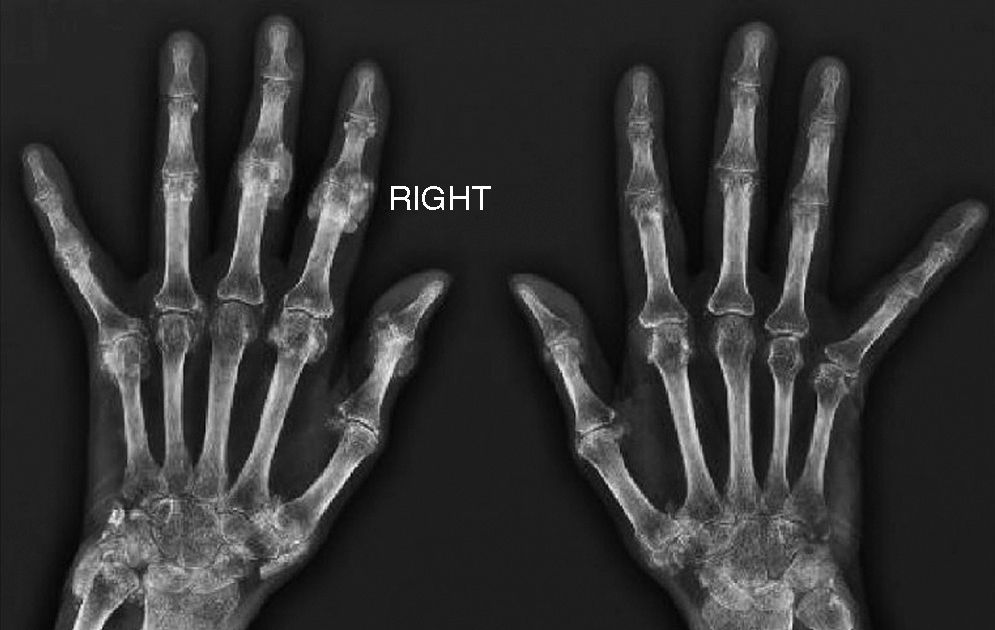
We present the case of a 63-year-old housewife who had a history of type 2 diabetes, hypertension and dyslipidemia, with good control, for which she was taking metformin, enalapril and atorvastatin. There was nothing notable in her family history, she did not consume harmful substances and was not contact with animals. She was referred to us with a 2-year history of polyarthralgia at irregular intervals, with predominantly mechanical symptoms, in small joints of the hands and feet. There was no swelling, but she reported having morning stiffness in the hands that lasted approximately 2h. In the review of organ systems for her medical history, she mentioned the development of a dry cough and dyspnea on moderate exertion since the onset of the arthralgias, as well as the appearance of Raynaud's phenomenon in her hands, without vasculitic lesions, one year earlier. Her appetite and weight had not been affected and she had no fever. Physical examination showed that her general health was good, with resting eupnea and no evidence of adenopathy or skin lesions; auscultation of heart and lungs revealed Velcro crackles down to middle lung fields, but there were no other findings; on rheumatological examination, she was found to experience pain on flexion and extension of both wrists, without synovitis, and small, cold, painless, semi-indurated lesions at some metacarpophalangeal and interphalangeal joints of the hands (Fig. 1); in the rest of the joint areas, there was no pain, limitations of the range of movement or swelling. The results of the neurovascular examination were normal, with no pain in response to pressure on the limb musculature or functional disability. The laboratory findings were as follows: complete blood count, blood biochemistry, acute phase reactants, aldolase, creatine kinase, thyroid hormones and parathyroid hormone were within normal range; the autoimmunity study only revealed positivity for anti-hystidyl-tRNA synthetase antibodies (anti-Jo-1) at a high titer (rheumatoid factor and anti-cyclic citrullinated peptide, antinuclear, anti-U1-RNP, anti-Ro anti-cytoplasmic and anti-endomysium antibodies were all normal). The electromyographic study of upper and lower limbs detected no evidence of inflammatory myopathy. The imaging studies performed included: radiographies of elbows, hands (Fig. 2), pelvis, knees and feet. The only abnormal findings were calcium deposits in periarticular areas of the hands, together with osteopenia, with no evidence of erosion of any joint. High-resolution radiography and chest tomography revealed a reticular pattern compatible with interstitial pneumonia. Lung biopsy was performed, and the final diagnosis was usual fibrosing interstitial lung disease. On the basis of the clinical data and results of the supplemental tests performed, we established a diagnosis of antisynthetase syndrome.
Antisynthetase syndrome is characterized by the presence of some of the described antisynthetase antibodies in serum, and at least one of the following clinical signs: interstitial lung disease, inflammatory myopathy or polyarthritis. Other features that support the diagnosis can include Raynaud's phenomenon, “mechanic's hands” and fever.2
Eight antisynthetase antibodies have been described, all of them directed against enzymes that acetylate transfer RNA (tRNA). The one most frequently detected is anti-Jo-1, partly because it is the only one that is routinely measured, given that the other antisynthetase antibodies require reference laboratories. The majority of the studies have demonstrated that patients with any of the antisynthetase antibodies described have interstitial lung disease. Although a large proportion of patients with antisynthetase syndrome have an inflammatory myopathy, some of the antisynthetase antibodies—particularly the anti-PL-12 antibodies (directed against alanyl-tRNA synthetase)—seem to be associated with interstitial lung disease without inflammatory myopathy,3 as was the case in our patient, despite the fact that she tested positive for anti-Jo-1.
With respect to the rheumatic manifestations of the antisynthetase syndrome, non-erosive symmetric polyarticular involvement is that most frequently found, and can be associated with distal calcinosis. Our patient reported no episodes of joint inflammation and we did not observe synovitis in our examination. Given that calcinosis usually develops in areas in which there has been an earlier inflammatory process, in our patient, the calcinosis may be the result of a previous subclinical inflammatory process (the patient was referred to us 2 years after the onset of her symptoms).
A recent publication from the Mayo Clinic4 dealt with the relationship between calcinosis and different connective tissue diseases. The rheumatic disease most frequently associated with calcinosis was dermatomyositis, followed by systemic sclerosis, mixed connective tissue disease and systemic lupus erythematosus. Approximately between 3% and 5% of the cases of antisynthetase syndrome can be classified as syndromes that overlap with other connective tissue diseases such as rheumatoid arthritis, systemic lupus erythematosus, systemic sclerosis or Sjögren's syndrome.5 The clinical and analytical data, data on autoimmunity, imaging studies and neurophysiological study ruled out all of these connective tissue diseases, as well as an overlap syndrome involving rheumatoid arthritis, as the cause of the calcinosis observed in our patient. Another interesting aspect of our case is the finding of periarticular calcinosis only in the hands, despite the fact that when calcinosis is associated with connective tissue diseases, it usually affects the areas of joint extension of the extremities in the form of a multifocal condition. Other processes that can cause calcinosis, although they were ruled out in our patient, are metabolic diseases (chronic nephropathy, hyperparathyroidism and hypervitaminosis D), parasitic infections like cysticercosis, and processes involved in muscle injuries or even periarticular injections.
The interest in our case lies in the presentation of calcinosis localized exclusively in the hands, with no evidence of previous inflammatory activity in or around the joints, in an anti-Jo-1-positive patient with antisynthetase syndrome, with no muscle involvement.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: García Rodríguez C, Salvatierra Ossorio J, Morales Garrido P, Raya Álvarez EG. Calcinosis en manos y síndrome antisintetasa sin afectación muscular. Reumatol Clin. 2016;12:60–61.