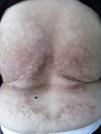
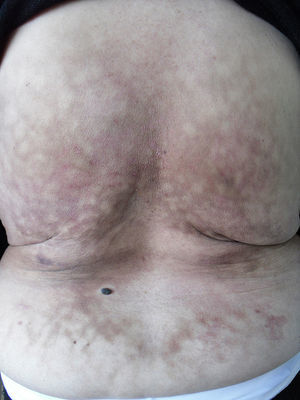
The patient was an 87-year-old woman with vertebral fractures and severe dorsolumbar osteoarthrosis. She was being treated with calcium, vitamin D and alendronate, in addition to nonsteroidal anti-inflammatory drugs (NSAID), tramadol and local heat. She came to our department with asymptomatic dorsal skin lesions that had appeared at some undetermined moment. The physical examination revealed an erythematous, violaceous, reticulated, macular region with areas of atrophic appearance and patches of brownish pigmentation, except in those portions on which her body did not rest heavily (Fig. 1). As the clinical diagnosis was consistent with erythema ab igne, she was asked about her daily routine with this in mind. The patient admitted that she had been using an electric blanket at high temperatures continuously for years, thus confirming the diagnosis. It was recommended that she limit her direct exposure to heat and that she lower the temperature. However, given the advanced stage of the skin damage, only a slight improvement was achieved.
Erythema ab igne is produced by repeated exposure of the skin to temperatures below the burn threshold (43–47°C). This exposure induces, by mechanisms that are still undefined, superficial damage to the dermal vascular plexus, with vasodilation and hemosiderin deposition, which result in its characteristic aspect.
This condition, which has been referred to as “hot water bottle rash”, traditionally appeared on the pretibial skin of elderly individuals due to exposure to space heaters. Today, practices like resting a laptop computer on one's thighs and, above all, the use of heat to relieve pain are the main triggers. Thus, we consider that those professionals who routinely recommend measures of this type must be made aware of this entity, since in the initial stages, the clinical signs may remit; however, if exposure is prolonged, the damage becomes irreversible, and cases of malignant transformation to epidermoid carcinoma have been reported.
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of InterestThe authors declare they have no conflicts of interest.
Please cite this article as: Cabrera Hernández A, Beà Ardebol S, Medina Montalvo S, Trasobares Marugán L. Eritema ab igne. Reumatol Clin. 2016;12:233–234.