Myositis ossificans is a heterotopic calcification consisting of the transformation of primitive mesenchymal cells, present in the muscle connective tissue, into osteogenic cells. This disorder can be hereditary, and can affect up to 2 children per million or, to a larger extent, be acquired secondarily to orthopedic and traumatic injuries,1,2 with greater incidence during the second and third decades of life. It is associated with skeletal anomalies, erythema, reduction of joint mobility and can mimic the clinical presentation of cellulitis, osteomyelitis or thrombophlebitis.
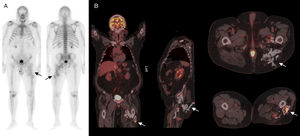
We report the case of a 66-year-old man, with a history of hematoma involving fibrous tissue. He underwent an intervention in left thigh, while in orthopedic follow-up. We performed bone scintigraphy after the administration of 815 MBq of 99mTc-hydroxymethylene-diphosphonate. We observed an abnormal increase in the osteoblastic activity in soft tissues of the middle and proximal third of left thigh up to left hip, with uptake of the tracer in the region of adjacent soft tissues and changes in normal bone morphology (Fig. 1A) compatible with myositis ossificans After a course of several years, and in the clinical context of a lesion suggestive of a lung neoplasm, we performed positron emission tomography-computed tomography (PET/CT) after administration of 370 mBq of 18-fluorodeoxyglucose (18F-FDG). We observed several accumulations of the radiotracer that were distributed by the posteroinferior planes of the left buttock up to the middle third of the ipsilateral thigh (Fig. 1B), with a maximum standardized uptake value (SUVmax) of 9.1 in relation to a lesion with a highly heterogeneous morphology, with areas that were calcified, hypodense and formed by soft tissues. These findings would correspond to myositis ossificans located exactly beneath the tip of the greater trochanter.3 Unlike metastatic calcifications, that are associated with a change in the calcium phosphate metabolism, myositis ossificans can appear as a complication of muscle injury with hematoma secondary to inflammation of the fascia following a neurological lesion, surgery, traumatic injury or a burn.4
(A) Whole body bone scan with 99mTc-hydroxymethylene-diphosphonate in anterior and posterior projections that show a pathological and irregular increase in osteoblastic activity in the middle and proximal thirds of left thigh, with tracer uptake in adjacent soft tissues and a change in the normal bone morphology (arrows). (B) Coronal, sagittal and axial images of the 18F-fluorodeoxyglucose positron emission tomography/computed tomography study showing multiple abnormal accumulations of the radiotracer that are distributed from posteroinferior planes of the left buttock up to the middle third of the ipsilateral thigh (arrows).
Although it is not a frequent finding in PET/CT studies, some investigations provide evidence of its use as a suitable tool in the evaluation of biological activity in soft tissues.5,6
Treatment depends on the degree of functional involvement, based on approaches involving radiotherapy, nonsteroidal anti-inflammatory drugs or diphosphonates7 with preventive intention, or surgical resection and rehabilitation in established cases.2,8
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of InterestThe authors declare they have no conflicts of interest.
Please cite this article as: Sánchez Aguilar M, García Jiménez R, Borrego Dorado I. Miositis osificante: gammagrafía ósea y tomografía por emisión de positrones/tomografía computarizada con 18F-desoxiglucosa. Reumatol Clin. 2018;14:309–310.