A 48-year-old female was diagnosed in 2008 with rheumatoid arthritis with a presence of the rheumatoid factor (RF) and an absence of antibodies against cyclic citrullinated peptides (anti-CCPs). She met with the 1987 ACR classification criteria (morning stiffness for over 1h, symmetric arthritis of both carpal joints and of the 2nd to 4th bilateral proximal interphalangeal joints, a positive RF result and radiography showing erosions in carpal joints). She also met with four out of six criteria of the 2002 American/European Consensus Classification (AECC) for Sjögren's syndrome (xerostomia, xerophthalmia, Schirmer 4mm test and positive results for anti-Ro/SSA 52 and 60 and anti-La/SSB antibodies), together with hypergammaglobulinaemia and infiltration of parotid glands viewed in the CT scan. In her clinical history, renal colic is notable, repeated over 10 years ago. It was assessed by the urology department which determined a wait-and-see approach. She is currently undergoing treatment with prednisone, sulfasalazine, methotrexate and ophthalmic cyclosporine, having already completed two cycles of 1g rituximab due to persistent polyarthritis.
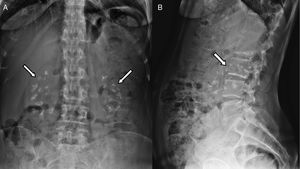
We observed an incidental finding of bilateral renal calcifications on an X-ray of the abdomen (Fig. 1). Analytically, the levels of creatinine and urea were normal (CKD-EPI 100.7ml/min), there were no basic–acid and hydroelectrolitical equilibrium alterations, she did not present with proteinuria and calcium levels were normal in urine at 24h (90mg/24h), as was phosphaturia. The pH balance was slightly alkaline (6.5) and there was insufficient vitamin D (36.8nmol/l) although parathyroid hormone levels were normal.
Diagnosis and EvolutionAs a result of the radiologic findings, the patient was diagnosed with nephrocalcinosis within the context of SS, despite not presenting with clinical or analytical alterations of nephropathy or alterations in the phosphocalcic metabolism. Close monitoring of renal function with periodical analytical controls was determined as treatment.
DiscussionNephrocalcinosis is characterised by calcification of the renal parenchyma. There are many causes including hyperparathyroidism, hypercalcemic nephropathy from excess vitamin D, Cacchi–Ricci disease (medullary sponge kidney) or distal renal tubular acidosis (dRTA) or type I acidosis.1
In SS, specifically, kidney function may be compromised in around 5% of cases. One of the possible causes of kidney compromise is dRTA. This leads to urinary alkalosis (pH>5.5), hyposthenuria, hypercalciuria, hyperphosphatemia and hypocitraturia, with or without metabolic acidosis and in several cases to hypokalaemia.2,3 Those patients with suspected dRTA who do not meet with analytical criteria may be given the ammonium chloride acid loading test to demonstrate the kidney's inability to acidify urine (pH<5.5).4
When there is development of basic–acid and hydroelectrolytic equilibrium alterations, treatment consists of administering bicarbonate and potassium citrate supplements to alkalinise the medium and recover losses, as well as a baseline treatment with glucocorticoids and immunosuppressants.1,5,6 It should be highlighted that the course of nephrolithiasis is distinct from that of nephrocalcinosis and that an incorrect treatment of metabolic acidosis may lead to the progression of nephrocalcinosis.7
We would therefore recommend an initial screening in patients with SS to detect possible nephropathy. An analysis of ions in the blood and of the phosphocalcic metabolism should be requested, as should a urine test at 24h, to evaluate the pH level, the proteinuria and excretion of ions, an immunological and serological test and also imaging tests.7
Ethical LiabilitiesProtection of people and animalsThe authors declare that no experiments using human beings or animals have been carried out for this research study.
Data confidentialityThe authors declare they have followed the protocols of their centre of work on patient data publication.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of InterestThe authors have no conflicts of interest to declare.
Please cite this article as: Jiménez Liñán LM, Rodríguez Montero SA, Marenco de la Fuente JL. Nefrocalcinosis en una paciente con artritis reumatoide y síndrome de Sjögren secundario. Reumatol Clin. 2019;15:58–59.