To analyse the clinical/epidemiological data, the management and the treatments established in patients with Ocular Cicatricial Pemphigoid (OCP) in a Rheumatology Service.
Material and methodsReview of clinical histories of patients with OCP referred by ophthalmology between 2008 and 2019.
ResultsIn our series of 27 patients, 67% were diagnosed and referred in the last 2 years. Most in Foster stage 1. Of the patients, 18.5% presented associated Sjogren's syndrome, with poor progression: 88.8% received Methotrexate, 74% used it as monotherapy and 66% continued with said treatment up to the end. Eighteen point five percent had to combine or rotate therapies, the drugs used were mycophenolate, azathioprine, cyclophosphamide, sirolimus, etanercept, rituximab: 29% used steroids. Only in 2 eyes was stage progression observed. There were no serious adverse events, and 37% had mild adverse events.
ConclusionStarting immunosuppressive therapy early is essential, methotrexate being a good initial alternative in our experience, and treatment must be escalated in line with disease progression.
Analizar los datos clínicos/epidemiológicos, el manejo y los tratamientos instaurados a pacientes con Penfigoide Ocular Cicatricial (POC) en un Servicio de Reumatología.
Material y métodosRevisión de historias clínicas de pacientes con POC derivados por oftalmología entre 2008 y 2019.
ResultadosEn nuestra serie de 27 pacientes, 67% fue diagnosticado y derivado en los últimos 2 años. La mayoría en estadío 1 de Foster. El 18,5% presentó Síndrome de Sjogren asociado, conllevando a una evolución desfavorable. El 88,8% recibieron Metotrexato, 74% lo utilizaron en monoterapia y 66% continuaron el tratamiento hasta el final. El 18,5% debió combinar/rotar terapias, las drogas utilizadas fueron micofenolato, azatioprina, ciclofosfamida, sirolimus, rituximab. El 29% utilizó esteroides. Solo en 2 ojos progresó el estadío. No se registraron eventos adversos serios y 37% presentó eventos adversos leves.
ConclusiónEl inicio temprano de la terapia inmunosupresora es fundamental, siendo el metotrexato una buena alternativa como tratamiento de inicio según nuestra experiencia, debiendo escalar el tratamiento de acuerdo a la evolución.
Mucus membrane pemphigoid is a systemic, chronic, cicatricial inflammatory disease of autoimmune aetiology and low incidence, characterised by the appearance of subepithelial ampullary and cicatricial lesions which affect the mucous membranes of the whole body. Isolated ocular involvement has traditionally been called ocular cicatricial pemphigoid (OCP) and may, on some occasions, lead to irreversible sight loss if no early treated is prescribed.1–3 For this reason, it is essential to start immunosuppressant treatment immediately after diagnosis, to suppress the inflammation and prevent sequelae.4
Diagnosis requires a high level of suspicion by the ophthalmologist, mainly in cases of chronic or recurrent conjunctivitis which do not respond to treatment. However, its confirmation requires a conjunctival biopsy.2,3,5
The disease is classified according to Foster in 4 stages depending on the severity of the ocular compromise, which allows progression to be assessed and its treatment to be monitored.6,7
The selection of the agent to be used depends on the severity of the disease and the systemic compromise. The success of treatment is defined as the inducement of a white eye, with no activity and without progression of cicatricial pemphigoid.7
ObjectiveTo analyse the clinical/epidemiological data, management and treatments established according to Foster stages in patients with OCP in a rheumatology department.
Materials and methodsWe reviewed the medical rheumatological histories of patients diagnosed with OCP, followed up by our services, between November 2008 and July 2019. All of them were diagnosed and referred to our consultation by ophthalmologists, with a OCP diagnosis through biopsy. Variables were recorded referring to sex, age, age at diagnosis, time from first symptoms to diagnosis, a history of cancer and the presence of extraocular compromise obtained using questioning and physical examination.
The following lab data were collected: erythrocyte sedimentation rate (over 20 mm in 1st hour), reactive C protein levels (above .5 mg/dl), gamma globulin (above 1.4 g/dl), antinuclear antibodies, rheumatoid factor, anti-Ro and anti-La antibodies.
Patients were referred with a report of the Foster stage and the presence/absence of conjunctival inflammation. Symptoms of activity were also assessed such as the presence of photophobia, ocular pain, conjunctival hyperaemia and chemosis. Foster staging was used to assess progression.
All patients were subjected to periodical controls in our practice and with their ophthalmologist, whose opinion about the disease activity was essential for treatment decisions.
The number of eyes affected was recorded with Foster staging.
Patients initiated treatment with 10 mg methotrexate weekly, always combined with a 5 mg folic acid weekly and treatment was changed if after 3 months evidence of activity /inflammation persisted. The dose was progressively increased up to 20 mg and then rotated with another drug or in combination with the same, in agreement with the ophthalmology service. It should be noted that some patients had already been referred with previous treatments, and continued with these when evolution was favourable. The second line drugs used were mycophenolate, cyclophosphamide and rituximab. Systemic oral steroids were used for short periods in medium/low doses for rapid symptom control and only in some patients. All patients received topical treatment with cyclosporin.
The adverse events of the drugs were also recorded.
The study design was approved by the ethics committee of our hospital and no informed consent was required due to the anonymous nature of the study.
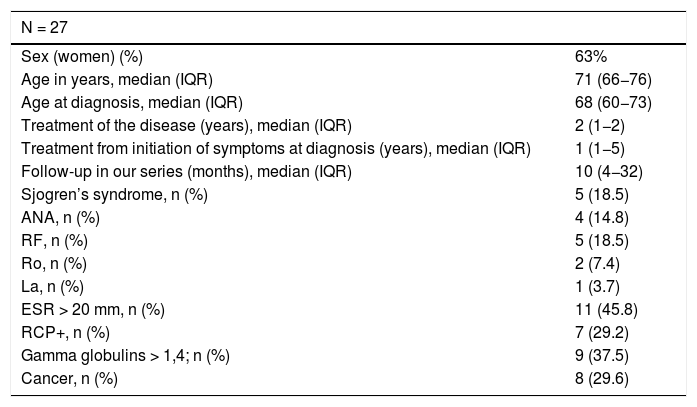
Descriptive statistics were performed on the variables studied to summarise demographic and clinical patient characteristics. Continuous variables were expressed as median and interquartile ranges and categorical variables as frequencies and percentages (Table 1).
Demographic, clinical and laboratory data of patients with cicatricial ocular pemphigoid.
| N = 27 | |
|---|---|
| Sex (women) (%) | 63% |
| Age in years, median (IQR) | 71 (66−76) |
| Age at diagnosis, median (IQR) | 68 (60−73) |
| Treatment of the disease (years), median (IQR) | 2 (1−2) |
| Treatment from initiation of symptoms at diagnosis (years), median (IQR) | 1 (1−5) |
| Follow-up in our series (months), median (IQR) | 10 (4−32) |
| Sjogren’s syndrome, n (%) | 5 (18.5) |
| ANA, n (%) | 4 (14.8) |
| RF, n (%) | 5 (18.5) |
| Ro, n (%) | 2 (7.4) |
| La, n (%) | 1 (3.7) |
| ESR > 20 mm, n (%) | 11 (45.8) |
| RCP+, n (%) | 7 (29.2) |
| Gamma globulins > 1,4; n (%) | 9 (37.5) |
| Cancer, n (%) | 8 (29.6) |
ANA: antinuclear antibodies; ESR: erythrocyte sedimentation rate; IQR: interquartile range; La: anti-La; RCP: reactive C protein; RF: rheumatoid factor; Ro: anti-Ro.
The clinical records of 27 patients were reviewed; 18 (67%) had been diagnosed and referred during the last 2 years.
Demographic, clinical and laboratory data are summarised in Table 1. Women predominate, with the average age at diagnosis being 65 years of age, and delay to diagnosis of one year.1–5 No extra ocular manifestations were determined. A history of cancer was recorded in 8 patients (29.6%) (3 cancer of the skin, 2 prostate, 2 haematological and one rectal cancer).
Foster stages for referral were Foster 0 = 15 eyes; 1 = 21 eyes; 2 = 5 eyes; 3 = 0 eyes; 4 = 5 eyes. Four patients did not present with stage reports. Only in 2 eyes of different patients was a progression from stage 1 to 2 and from 2 to 3 determined.
In 5 patients (18.5%) associated-Sjogren’s syndrome was diagnosed and it is notable that 4 of these had to combine or rotate treatments.
In laboratory tests less than half of the patients presented with accelerated erythrocyte sedimentation rates, positive reactive C protein and polyclonal hypergammaglobulinaemia (Table 1).
Table 2 contains the treatment the patients received.
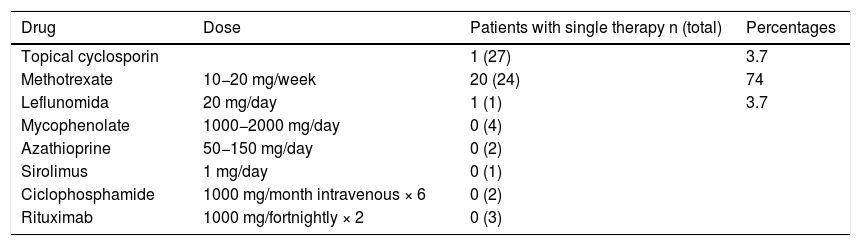
Treatments offered.
| Drug | Dose | Patients with single therapy n (total) | Percentages |
|---|---|---|---|
| Topical cyclosporin | 1 (27) | 3.7 | |
| Methotrexate | 10−20 mg/week | 20 (24) | 74 |
| Leflunomida | 20 mg/day | 1 (1) | 3.7 |
| Mycophenolate | 1000−2000 mg/day | 0 (4) | |
| Azathioprine | 50−150 mg/day | 0 (2) | |
| Sirolimus | 1 mg/day | 0 (1) | |
| Ciclophosphamide | 1000 mg/month intravenous × 6 | 0 (2) | |
| Rituximab | 1000 mg/fortnightly × 2 | 0 (3) |
Twenty four patients (88%) received methotrexate, of whom, 20 (74%) were in monotherapy and 18 of these (66%) continued with this treatment until the end of observation due to favourable evolution. One patient was in treatment with leflunomide and continued with it and another patient only had topical therapy with cyclosporine with no systemic treatment.
In 5 patients (18.5%) therapies had to be combined or rotated. The drugs used were azathioprine, micophenolate, cyclophosphamide, sirolimus and rituximab, with the latter being used when at least 2 previous lines of treatment had failed. The disease symptoms were controlled and progression had good outcomes in 3 of the patients treated. One patient also received etanercept combined with methotrexate for rheumatoid arthritis, with no progression of Foster staging.
Systemic steroids were used in 8 patients (29%) at some time, in low doses and for short periods. In the evolution of 4 patients it was recorded that they could withdraw the systemic treatment due to absence of sustained inflammation.
No severe adverse events were recorded, 10 patients (37%) presented with mild adverse events with the most frequent being gastrointestinal and none of them had to suspend treatment.
DiscussionEpidemiological data coincided with previous publications. One outstanding event was the presence of 5 patients with associated Sjogren’s syndrome, which led to a poorer prognosis in evolution since they had to rotate or combine treatments to achieve disease control.
Most of our patients were referred during the last 2 years and unlike other publications, in Foster stages 0 and 1, what stood out was the higher awareness of this pathology, early suspicion of it and rapid diagnostic confirmation by ophthalmology, leading to fast treatment initiation, conditioning evolution in a positive manner, since progression of staging was only found in 2 patients.8 This also highlights the importance of interdisciplinary coordination in this pathology.
Methotrexate was the most used treatment with good tolerance and control of inflammation, particularly in early stages. Based on our experience we were able to consider it a good initial option which, combined with mycophenolate, appeared to have a better response and tolerance than other drugs in initial stages.7,9,10 Treatments had to be combined or rotated according to disease evolution and in our experience rituximab managed to control the disease symptoms and progression after many previous treatments in the 3 patients treated.7,11
The existing bibliography to date is scarce and divergent, and controlled studies are therefore required with larger numbers of patients to be able to offer treatment recommendations in this pathology.
ConclusionDue to the inflammatory, autoimmune, progressive and cicatricial nature of OCP it is essential to offer early immunosuppressant therapy, aimed at eliminating inflammation and avoiding sequelae. Methotrexate is a good alternative as initial treatment in our experience, and there should be a stepping-up of treatment according to evolution. Interdisciplinary management of the disease is vitally important.
Conflict of interestsThe authors have no conflict of interests to declare.
Please cite this article as: Smichowski AM, Caputo VD, Romeo C, Rivero E, Morales NS, Casado G. Penfigoide ocular cicatricial: ¿metotrexato como tratamiento de inicio? Reumatol Clin. 2022;18:30–32.