We are writing to present the atypical case of a rare first manifestation of granulomatosis with polyangiitis.
The patient is a 74-year-old woman who came to our centers’ Emergency department due to 4 days with persistent headache associated to a red right eye and ptosis of the same side. The process had an abrupt onset and was not associated to fever or trauma, persisting over time and not improving with rest. Upon examination the patient had no cardiopulmonary, abdominal, locomotor, central or peripheral nervous system alterations; just the right red eye and ptosis were found. In the urgent laboratory tests requested we only found a CRP of 78mg/l and ESR of 109mm/h, with the rest of the serology within normal limits.
Eye examination showed unilateral proptosis of the right eye, red eye with a negative Tyndall effect, absence of cells in the anterior or posterior chamber, without retinal lesions. The patient had a 0.6 visual acuity of the right eye and of 1 on the left eye.
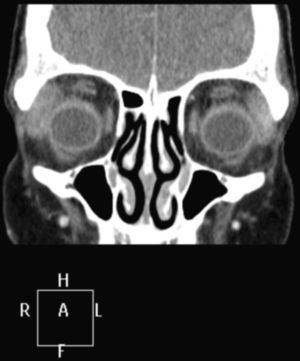
A cerebral magnetic resonance was performed showing an increase in the size of the right lacrimal grand with supracilliar and lateral and superior orbital affection of the right eye, compatible with dacryocystitis/infiltrative process (Fig. 1, coronal plane), leading us to the diagnosis of orbital pseudotumor with muscle affection and dacryocystitis, beginning treatment with high dose steroids and intravenous antibiotics, due to the severity of the process. A biopsy of the swollen area was performed but the result was non significant and response to medication was tapered, due to the severity of the eye manifestations.
We only found positivity to PR3 45U/ml (normal<3), with infectious serology (HIV, Syphillis, Brucella, hepatitis B and C, Toxoplasma), autoimmunity (RF, ANA, anti-DNA negative; ANCA: MPO negative), thyroid hormones and tumor markers negative. The chest X-ray did show a nodular pattern in the lower right lobe.
Two weeks later the patient presented non specific muscle and joint pain of the upper limbs, a single ulcer on the base of the tongue and fever. We performed a thoracic computed tomography which revealed several symmetric and random nodules, mainly on the right lung base, measuring 5 and 15mm, some of them cavitated, possibly related to granulomatosis. The lateral segment of the middle right lobe showed a condensation possibly related to the same process.
A transbronchial lung biopsy was performed showing a granulomatous vasculitic process, with segmental vascular necrosis and neutrophil and monocyte infiltration, making us reach a conclusion of granulomatosis with polyangiitis.
With respect to later treatment, once the diagnosed was reached we began treatment with: (a) pulse steroid 1.000mg for three doses, continuing with oral prednisone 1mg/kg for 2–4weeks and reducing to 20mg/day at the end of the second month, with a progressive downward adjustment for 6 months, (b) associated with cyclophosphamide boluses for 4 weeks intravenously, and (c) trimetoprim-sulphamethoxazole, orally, 3/week for Pneumocystis carinii prophylaxis.
Granulomatosis with polyangiitis is a systemic vasculitis of unknown cause that affects small and medium caliber vessels. It is characterized by respiratory system and kidney affection but may affect other organs. ANCA are frequently positive and the most important histologic characteristic is the presence of necrotizing granulomas.1,2 Their incidence in Spain reaches 2.95 cases/million inhabitants for granulomatosis with polyangiitis, 7.91 cases/million for microscopic polyarteritis and 1.31 cases/million for Churg-Strauss’ disease.3
Throughout the disease process, the incidence of ophthalmic manifestations described in this type of vasculitis4,5 goes from 20 to 50% of cases. Per region, the incidence is: conjunctivitis, keratitis (12%–20%); episcleritis and scleritis (12%–27%); uveitis (2%–7%); optic neuritis (12%–16%), and proptosis (15%–57%), but being very atypical as a presenting symptom.
Eye affection is a primordial manifestation of granulomatosis with polyangiitis and it distinguishes it from other systemic or ANCA positive vasculitidies.6,7 The most common initial manifestation is proptosis, but as in this patients case, the presence of diplopia and loss of visual acuity have also been previously described.
The differential diagnosis of orbital affection in a patient with granulomatosis with polyangiitis must include infections, fungal or bacterial, orbital lymphoma, sarcoidosis, Graves disease and orbital pseudotumor.
Treatment, based on adequate immunosuppression with steroids associated to cyclophosphamide, has led to the control of the disease in a high percentage of patients, although it is true that the loss of visual acuity is in many cases irreversible and requires a strict control by Ophthalmology as well as Rheumatology and primary care.
Please cite this article as: López-González R, Martínez-González O, Martín-Luquero Ibáñez M, Valdazo de Diego JP. Ojo rojo como manifestación primaria de vasculitis sistémica. Reumatol Clin. 2014;10:193–194.