To assess the association between histologic findings in the minor salivary gland biopsy (MSGB) and anti La (La/SS-B) and antiRo antibodies (Ro/SS-A), antinuclear antibodies (ANA) and rheumatoid factor (RF), and compare the value of the latter as diagnostic tests with MSGB, considered as the gold standard.
Materials and methodsPatients with suspected primary Sjögren syndrome (PSS) referred for MSGB were included. Antibody measurements were performed. Grades III and IV biopsy results were considered positive.
ResultsTwo hundred and eighteen (218) patients were included, 95% females, with a median age of 54 years and 12 months median duration of sicca symptoms. Thirty-six of the biopsies were positive. 33% of patients had positive anti Ro/SS-A anti La/SS-B antibodies, 62% had positive ANA, and 31% positive RF. A statistically significant association was found between MSGB and anti Ro/SS-A anti La/SS-B, ANA and RF. ANA were the most sensitive antibodies (84%. 95% CI: 75– 92), and the most specific were: anti Ro/SS-A and/or anti La/SS-B (78%. 95% CI: 71–85) and RF (78%. 95% CI: 69–87).
ConclusionOn PSS clinical suspicion, anti Ro/SS-A and anti La/SS-B antibodies have a great value to achieve the diagnosis, with MSGB useful for diagnosis of seronegative patients. The results also suggest the importance of ANA and RF for PSS classification.
Evaluar la asociación entre los hallazgos histológicos de la biopsia de glándula salival menor (BGSM) y los anticuerpos anti La (La/SS-B), anti Ro (Ro/SS-A), anticuerpos antinucleares (FAN) y factor reumatoideo (FR), y comparar el valor de estos como test diagnóstico con la BGSM considerada como patrón oro.
Material y métodosSe incluyeron pacientes con sospecha de síndrome de Sjögren primario (SSp) derivados para realización de BGSM. Se realizó medición de anticuerpos y se consideró BGSM positiva a los grados III y IV de la clasificación de Chisholm.
ResultadosSe incluyeron 218 pacientes, 95% género femenino, con una mediana de edad de 54 años y de tiempo de evolución de los síntomas sicca de 12 meses. El 36% de las biopsias fueron positivas. El 33% de los pacientes presentaban anticuerpos anti Ro/SS-A anti La/SS-B positivos, 62% FAN positivo y el 31% FR positivo. Se encontró asociación estadísticamente significativa entre la BGSM y anti Ro/SS-A, anti La/SS-B, FAN y FR. El FAN resultó ser el anticuerpo más sensible (84% IC95%: 75-92), siendo los más específicos: anti Ro/SS-A y/o anti La/SS-B (78% IC95%: 71-85) y el FR (78% IC95%: 69-87).
ConclusiónAnte la sospecha clínica de SSp, los anticuerpos anti Ro/SS-A y anti La/SS-B son de gran valor para arribar al diagnóstico, siendo la BGSM especialmente útil en los pacientes seronegativos. Los resultados también sugieren la utilidad del FAN y el FR para la clasificación de SSp.
Sjögren's syndrome (SS) is a systemic autoimmune disease involving the exocrine glands, manifesting with symptoms arising from hyposecretion thereof. In addition to symptoms arising from the exocrine affection, the disease can produce various extraglandular manifestations. SS can occur alone, as primary SS (pSS) or associated with other autoimmune diseases, as secondary SS.1
To date different classification criteria have been proposed, which are based on a combination of clinical, serological and histological findings.2–8
Histology, as part of the diagnosis, was first proposed in 1970 by Waterhouse, Chisholm and Mason; the latter were those establishing the score using foci of inflammatory cells aggregates.9
In order to obtain the material for pathology, a minor salivary gland biopsy (MSGB) is performed. While this is an invasive procedure, it is easy to perform and several studies show a low frequency of complications, which are usually mild.8–14
However, despite the simplicity of the technique, MSGB is not incorporated into daily practice in all centers, which leads to inconvenience in defining the presence of SS according to the American–European 2002 classification criteria currently in force.8
According to these criteria, the presence of a compatible MSGB and/or the presence of anti-Ro/SS-A and/or anti La/SS-B are necessary to diagnose pSS.
Furthermore, the 1993 European criteria and7 the 2012 preliminary criteria10 include, in addition to anti Ro/SS-A and La/SS-B antibodies, anti-nuclear (ANA) and rheumatoid factor (RF) as part of the serological criteria.
Because there is still difficulty in obtaining a MSGB for the diagnosis of SS in daily practice, we set out to estimate the association between the presence of histological stages III and IV affection in the classification proposed by Chisholm and the presence of anti Ro/SS-A and/anti-La SS-B; and assess the value of these antibodies as a diagnostic test, compared with MSGB, which was taken as a reference test or gold standard.
The secondary objectives evaluated were the association between the presence of infiltrates stages III and IV in MSGB with ANA and RF positivity and analyze the value of such antibodies as a diagnostic test, compared with MSGB.
Materials and methodsThe study design was observational, analytical and cross-sectional.
We included consecutive patients with suspected pSS derived from different centers of Argentina to the Rheumatology Department, Hospital Rivadavia, for a MSGB, between October 2007 and December 2011.
Exclusion criteria were related to the procedure: use of aspirin or other NSAIDs within the week before the study, clinical signs of local infection at the site of the biopsy, patients with anticoagulation or a clotting disorder or other causes of sicca symptoms and treatment with anticholinergic drugs or radiotherapy of the head and neck. Biopsies in which the material obtained was insufficient or non-glandular, patients with other autoimmune associated rheumatic disease, cases where results of anti-Ro/SS-A or anti-La/SS-B were not available were also excluded as well as those who refused inclusion into the protocol.
Demographics (age, gender), duration of sicca symptoms when performing the biopsy, concomitant disease (hypothyroidism and diabetes), treatment at the time of the biopsy (corticosteroids, immunomodulatory/immunosuppressive drugs), antibody results (ANA in Hep 2, anti Ro/SS-A, anti-La/SS-B by ELISA, latex nephelometry and turbidimetry RF,) as well as MSGB results according to the classification proposed by Chisholm–Mason were recorded. The results of biopsies stages III and IV were considered as positive 9.
Xerophthalmia and xerostomia were defined as the presence of symptoms of ocular and oral dryness according to the classification criteria proposed in 2002.8
Since the 2002 classification criteria require positivity for anti Ro/SS-A and/or anti La/SS-B or a positive MSGB to classify a patient with pSS and the latter being an invasive biopsy procedure, we decided to choose the latter as the gold standard, with the objective of assessing the value of the antibodies and their usefulness as a replacement for MSGB.
The pathologic study was carried out by a single, independent and blinded pathologist, the Chair of Anatomic Pathology at the Faculty of Medicine of Buenos Aires, with over 15 years experience in the evaluation of histological material from MSGB. Antibodies were determined in different centers of reference of the country, mainly in the city of Buenos Aires, and the cutoff used to define the results as positive or negative was defined by the laboratory of each center.
The study was approved by the education, research and ethics committee of the hospital. Patients signed informed consent.
Statistical analysisThe data were fed into a Microsoft Excel database and analyzed using the STATA 11 statistical package.
The general characteristics of the population were described; continuous variables were reported as means and standard deviations (SD) or medians and interquartile ranges (IQR) according to their distribution. Frequency distribution analysis of categorical variables was performed.
For the bivariate analysis a t test or Mann–Whitney test for continuous variables, such as distribution and sample size, was used. Categorical variables were analyzed using chi-square or Fisher exact test according to a distribution table as expected frequency.
To assess the association and the presence of potential confounders in the relationship between the positivity of each of the antibodies and MSGB, three models of multiple logistic regression were performed: 1–MSGB and anti Ro/SS-A, anti-La/SS B antibodies, 2–MSGB and ANA and 3–MSGB and RF, considering the biopsy as the dependent variable. Odds ratios (OR) and corresponding 95% CI were calculated.
P<.05 was considered as significant.
Sensitivity (S), specificity (Sp), positive predictive value (PPV), negative predictive value (NPV) and positive likelihood ratio (PLR) were calculated with their respective 95% confidence intervals (95%CI) for each antibody and compared with MSGB, which was taken as the gold standard.
ResultsFrom October 2007 to December 2011, 400 patients referred by their GP with suspected pSS underwent a MSGB. One hundred and eighty-two patients were excluded: 130 for lacking anti Ro/SS-A or anti-La/SS-B antibody results, 31 had an associated autoimmune rheumatic disease, 21 had insufficient or no glandular material; 218 patients were included for analysis. The 130 patients excluded due to lack of anti Ro/SS-A or anti-La/SS-B antibody results were similar to those included in the study: 96% female (92 of 96 patients), median age 53 years (ric: 41–60.92 patients), 91% had xerophthalmia (88 of 91 patients), 85% xerostomia (78 of 92 patients), 80% mentioned both manifestations (74 of 92 patients) and 49% had a positive sialometry (21 of 43 patients).
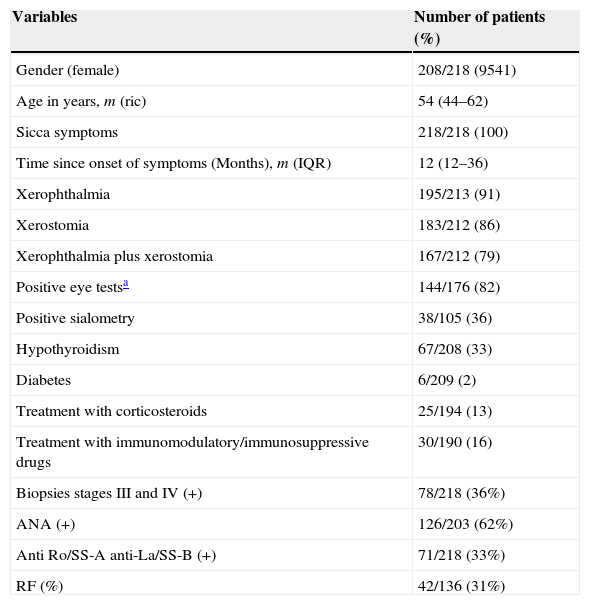
The reason of the referral for a biopsy of all patients included in the study was the presence of xerophthalmia and/or xerostomia in the context of suspected pSS. 95% (208/218) of patients were female, with a median age of 54 years (ric: 44–62) and median time of disease progression of 12 months with sicca symptoms (ric: 12–36). 92% had xerophthalmia, and 86% xerostomia; 79% had both manifestations (Table 1).
Demographic and Clinical Characteristics.
| Variables | Number of patients (%) |
|---|---|
| Gender (female) | 208/218 (9541) |
| Age in years, m (ric) | 54 (44–62) |
| Sicca symptoms | 218/218 (100) |
| Time since onset of symptoms (Months), m (IQR) | 12 (12–36) |
| Xerophthalmia | 195/213 (91) |
| Xerostomia | 183/212 (86) |
| Xerophthalmia plus xerostomia | 167/212 (79) |
| Positive eye testsa | 144/176 (82) |
| Positive sialometry | 38/105 (36) |
| Hypothyroidism | 67/208 (33) |
| Diabetes | 6/209 (2) |
| Treatment with corticosteroids | 25/194 (13) |
| Treatment with immunomodulatory/immunosuppressive drugs | 30/190 (16) |
| Biopsies stages III and IV (+) | 78/218 (36%) |
| ANA (+) | 126/203 (62%) |
| Anti Ro/SS-A anti-La/SS-B (+) | 71/218 (33%) |
| RF (%) | 42/136 (31%) |
m: median; IQR: interquartile range.
Of the 218 biopsies, 36% (78) were positive (stage III or IV) and 64% (140) negative (stage 0, I or II). 33% (71/218) of patients had anti-Ro/SS-A, La/SS-B positive antibodies, 62% (126/203) had positive ANA and 31% (42/136) positive RF (the result of RF and ANA was not counted in all of the cases) (Table 1).
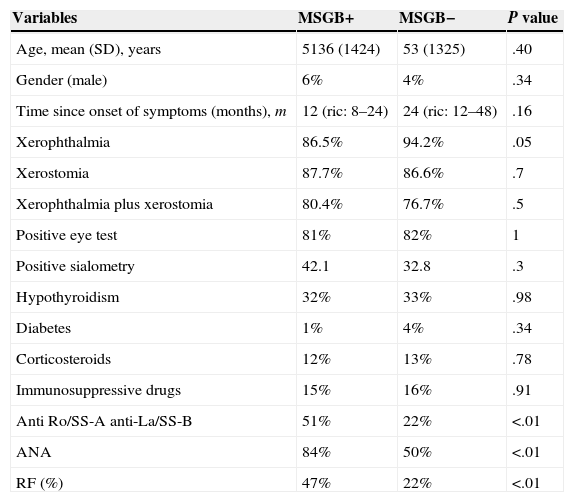
Comparing the demographic and clinical characteristics of patients with positive MSGB with patients with negative MSGB in the univariate analysis, no statistically significant differences in any of the analyzed variables (Table 2) were found.
Results of the univariate analysis: demographic and clinical characteristics between MSGB+ and MSGB−.
| Variables | MSGB+ | MSGB− | P value |
|---|---|---|---|
| Age, mean (SD), years | 5136 (1424) | 53 (1325) | .40 |
| Gender (male) | 6% | 4% | .34 |
| Time since onset of symptoms (months), m | 12 (ric: 8–24) | 24 (ric: 12–48) | .16 |
| Xerophthalmia | 86.5% | 94.2% | .05 |
| Xerostomia | 87.7% | 86.6% | .7 |
| Xerophthalmia plus xerostomia | 80.4% | 76.7% | .5 |
| Positive eye test | 81% | 82% | 1 |
| Positive sialometry | 42.1 | 32.8 | .3 |
| Hypothyroidism | 32% | 33% | .98 |
| Diabetes | 1% | 4% | .34 |
| Corticosteroids | 12% | 13% | .78 |
| Immunosuppressive drugs | 15% | 16% | .91 |
| Anti Ro/SS-A anti-La/SS-B | 51% | 22% | <.01 |
| ANA | 84% | 50% | <.01 |
| RF (%) | 47% | 22% | <.01 |
SD, standard deviation; m, median; IQR, interquartile range.
When analyzing the presence of the association between antibodies and MSGB in a univariate analysis, statistically significant associations with ANA (P<.01), anti Ro/SS-A and/or anti-La/SS-B antibodies (P<.01) and RF (P<.01) were found (Table 2).
Considering the MSGB as a dependent variable, and anti Ro/SS-A La/SS-B antibodies as a variable of interest, in a multivariate analysis adjusted for age, duration of symptoms, hypothyroidism, treatment with immunomodulatory/immunosuppressive drugs and the confounding effect of ANA antibodies, a confounding effect was found in the relationship between MSGB and anti-Ro/SS-A anti-La/SS-B (crude OR MSGB-anti Ro/SS-A anti-La/SS-B: 3.70, CI 95% CI 2.04–6.72, P<.01. ANA adjusted OR: 2.59, 95% CI 1.29–5.22, P<.01). By including in the analysis the RF, a confounding effect was also exerted, losing the anti La/SS-B anti Ro/SS-A antibodies association with a positive biopsy (OR: 1.98; 95% CI 0, 79–5.00, P: .15). The remaining variables did not exert a confounding effect or show significant associations in the multivariate model.
By analyzing the relationship between ANA and MSGB, a significant and independent association was observed between ANA and MSGB, with the anti Ro/SS-A La/SS-B antibodies being a confounder of the relationship (crude OR ANA MSGB-5.25, 95% CI 2.59–10.65; P<.01. OR adjusted for anti Ro/SS-A anti-La/SS-B: 3.36, 95% CI 1.53–7.36, P<.01). RF remained associated significantly and independently to the MSGB without exerting a confounding effect in the relationship between the ANA and MSGB.
By adjusting the relationship between RF and MSGB, neither the ANA nor the anti Ro/SS-A La/SS-B antibodies exerted confounding effects (OR crude MSGB-FR: 3.17, 95% CI 1.48–6, 75, P<.01. Adjusted OR: 2.99, 95% CI 1.30–6.87, P<.010). All other variables remained without association and did not behave as confounders.
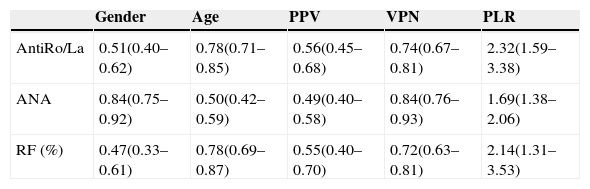
Finally, we calculated the S, Sp, PPV, NPV and PLR of each of the antibodies using the MSGB as a reference test. ANA proved to be the most sensitive (0.84, 95% CI 0.75–0.92) and had the best NPV (0.84, 95% CI 0.76–0.93), whereas anti-Ro/SS-A and/or anti-La/SS-B and RF yielded similar results, being the most specific (95% CI 0.71–0.85 0.78 and 0.78, 95% CI 0.69–0.87, respectively) and having the best PPV (0.56 95% CI 0.45–0, 58 and 0.55 95% CI 0.40–0.70, respectively). All showed good PLR (Table 3).
S, Sp, PPV, NPV, and PLR of the Different Antibodies in Relation to the MSGB (Gold Standard).
| Gender | Age | PPV | VPN | PLR | |
|---|---|---|---|---|---|
| AntiRo/La | 0.51(0.40–0.62) | 0.78(0.71–0.85) | 0.56(0.45–0.68) | 0.74(0.67–0.81) | 2.32(1.59–3.38) |
| ANA | 0.84(0.75–0.92) | 0.50(0.42–0.59) | 0.49(0.40–0.58) | 0.84(0.76–0.93) | 1.69(1.38–2.06) |
| RF (%) | 0.47(0.33–0.61) | 0.78(0.69–0.87) | 0.55(0.40–0.70) | 0.72(0.63–0.81) | 2.14(1.31–3.53) |
AUC, area under the curve; Sp, specificity; PLR, positive likelihood ratio; S, sensitivity; NPV, negative predictive value; PPV, positive predictive value.
To date, different classification criteria pSS have been proposed, which are based on a combination of clinical, serological and histological findings.2–8 There have been many classifications, from the publication of the San Francisco2 (which prioritize the histopathological appearance) and the San Diego criteria,3 in which the MSGB is essential for the diagnosis of defined pSS, as well as the Copenhagen4 Greeks,5 Japanese6 and the European Community criteria,7 which do not require a MSGB nor the presence of antibodies, to the American–European criteria 20028 and the 201210 US Preliminary Criteria which require the presence of histological or serological criteria.
Given the diversity of criteria used throughout the years and the lack of training for obtaining and reading the material from a biopsy, combined with the minor risks associated to the procedure,8–14 determining where it would be desirable to histologically define the diagnosis of pSS often poses problems in daily practice.
Our study aims to provide information to help define the usefulness of antibodies as an alternative to biopsies for the classification of pSS, using the MSGB as a gold standard. We found not only a significant association of anti Ro/SS-A La/SS-B antibodies with MSGB, but also with ANA and RF. In turn, given the PLR of all such antibodies, one can consider each as good study in relation to glandular inflammatory damage, although given the low specificity of ANA, its combination with another antibody such as RF, as proposed in the 2012 preliminary criteria, appears to be an option.
Other studies also analyzed the relationship between antibodies and MSGB. Manoussakis et al.,15 in a study conducted with 54 patients with a clinical diagnosis of pSS and 92 patients with rheumatoid arthritis, found that anti-Ro/SS-A, anti-La/SS-B antibodies and the titers of ANA and RF correlated with the histological stage of the biopsy.
Saito et al.,16 in a study of 107 patients with SS, found that both RF and the anti Ro/SS-A and anti-La/SS-B antibodies were significantly more frequent in patients with periductal lymphocytic infiltrate.
In turn, Wise et al.,17 in their analysis of 187 patients in whom MSGB was performed to study pSS, found that patients with foci score over 1 on biopsy had a significantly higher frequency of ANA, RF, anti Ro/SS-A and anti-La/SS-B.
Regarding anti Ro/SS-A and anti La/SS-B antibodies, it has been described that patients with anti La/SS-B show a greater inflammatory infiltrate in subjects only having positive anti Ro/SS-A and those who are seronegative.18,19 Halse et al. showed the presence of a good correlation between the foci score and the presence of Ro 52kD and 48kD in saliva, indicating a strong relationship between local inflammation and autoantibody production.18 Moreover, a strong correlation between the presence of autoantibodies in serum and 52-kD Ro, Ro 60kD and La/SSB in the salivary glands was found.20,21
A study conducted in 181 Chinese patients with an initial diagnosis of pSS compared different methods of detection of serum anti Ro/SS-A (double immunodiffusion, Western blot and ELISA) and found a significant association with MSGB with the three methods, although the degree of agreement between the foci histological score and the antibody detected by Western blot was not very good, concluding that the positive results of such antibodies in serum may indicate higher than 1 scores on biopsy, therefore in these cases could obviate the22 performance thereof.
On the other hand, Peen et al.23 revalidated the association between RF positivity and the presence of lymphocytic foci at histology, while Bamba et al.24 found a significant association between anti-Ro/SS-A and anti-La/SS-B antibodies and a positive biopsy, but not with the ANA.
Daniels et al. in a multicenter study with a large number of patients also observed this association between the four serological markers and MSGB25 and the same group even proposed new classification criteria of the disease which include RF and ANA, the latter with a titer greater or equal to 1/320.26 Thus arose the 2012 American preliminary criteria, in which the domain considered positive is the immunology laboratory, before the positivity of anti-Ro/SS-A and/or anti La/SS-B and/or ANA (a titer greater or equal to 1/320) plus RF.10
However, controversy exists on the inclusion of ANA and RF in the new set of proposed criteria, given that this decision stems from a consensus of experts of the sicca cohort in which there were patients with other autoimmune rheumatic diseases analyzed, leading many experts to suggest further studies regarding this point, before defining its true role within the 2012 criteria.27,28
With respect to our study, it has limitations due in large part because the data come from normal clinical practice. We believe there may be a bias in patient selection because many times in daily practice a MSGB is performed only in the presence of negative anti Ro/SS-A and anti-La/SS-B antibody results; there could also be a bias in the results of antibody testing, since they were conducted in different centers. On the other hand, a weakness of the study was the lack of additional information on other clinical manifestations of patients, in addition to ocular and oral dryness, due to the difficulty in collecting this information from patients who, in many cases, come from other health care centers.
On the other hand, although the sample size was not calculated for diagnostic tests, the number of observations available allowed for no empty cells or very few observations in the contingency table, impeding ample 95%CI, which also speaks of a small number of patients.
In any case, we believe that the results of this study reinforce the notion that while the clinician can do without the MSGB in patients with positive anti-Ro/SS-A, anti-La/SS-B antibodies, it is of fundamental importance in seronegative patients. On the other hand, the significant and independent relationship found between ANA and MSGB and between RF and MSGB and the results of their value as diagnostic tests, suggest that these antibodies, bu themselves in the case of RF (due to their higher specificity), or possibly in combination (ANA plus RF) could be useful in assessing the immunology laboratory domain in the pSS classification.
Ethical ResponsibilitiesProtection of people and animalsThe authors declare that this research did not perform experiments on humans or animals.
Data confidentialityThe authors declare that they have followed the protocols of their workplace regarding the publication of patient data.
Right to privacy and informed consentThe authors have obtained the informed consent of patients and/or subjects referred to in the article. This document is in the possession of the corresponding author.
Conflict of InterestThe authors have no conflict of interest to state.
Please cite this article as: Santiago ML, Seisdedos MR, Garcia Salinas RN, Catalán Pellet A, Villalón L, Secco A. Utilidad de los anticuerpos y de la biopsia de glándula salival menor en el estudio del complejo sicca en la práctica diaria. Reumatol Clin. 2015;11:156–160.