Cardiac complications in scleroderma (SD) are associated with a poor prognosis. Up to 15% of patients, generally with limited forms and anticentromere antibodies, develop pulmonary hypertension (PHT). Early diagnosis improves the prognosis, so that routine transthoracic echocardiograms (TTE) are recommended.1 Pericardial bleeding has also been described, as have valvulopathies, myocarditis and hypertrophy or myocardial fibrosis.2,3 We believe it is of interest to present the case of a patient with limited SD who developed mitral-aortic valvulopathy that was finally attributed to ergotamine toxicity.
A 59 year-old woman diagnosed SD based on Reynaud’s phenomenon, characteristic capillaroscopy and anticentromere antibodies. At the moment of diagnosis TTE showed insignificant aortic and mitral insufficiency, normal systolic function and the absence of PHT data. 11 years later the valvulopathy had evolved to become severe mitral and tricuspid insufficiency, moderate aortic insufficiency and severe PHT (PSAP: 75 mmHg). Two mechanical prostheses were therefore implanted at mitral and aortic levels.
Two years later she visited due to general syndrome and dyspnoea. She was treated with Furosemide, Ranolazine, Acenocumarol, Spironolactone, Omeprazol and Bromazepam.
Physical examination only found distal metacarpophalangeal sclerodactila, with no scarring, ulcers or telangiectasias, and mild cutaneous sclerosis on the legs.
Relevant analytical data are shown in Table 1.
Analytical results.
| Biochemistry | Haemogram | Immunology | |||
|---|---|---|---|---|---|
| Creatinine | 1.23 mg/dl | Haemoglobin | 12.5 g/dl | ANA | Positive 1/1,280, centromere |
| AST | 44 UI/l | Leukocytes | 7,620 | Anti-DNA, ENA, ANCA | Negative |
| AP | 716 UI/l | Platelets | 13,700 | Anticardiolipin antibodies, anti-2-glycoprotein antibodies | Negative |
| GGT | 290 UI/l | PCR | 46 m/h | IgG4 | Normal (0.05) |
| PCR | 2.54 mg/dl | – | – | Plasmablasts in peripheral blood | Negative |
ANA: antinuclear antibodies; ANCA: antineutrophile cytoplasm antibodies; Anti-DNA: anti-DNA antibodies; AST: aspartate aminotransferase; ENA: extractable nuclear antigens; AP: alkaline phosphatase; GGT: gamma glutamyl transpeptidase; PCR: polymerase chain reaction.
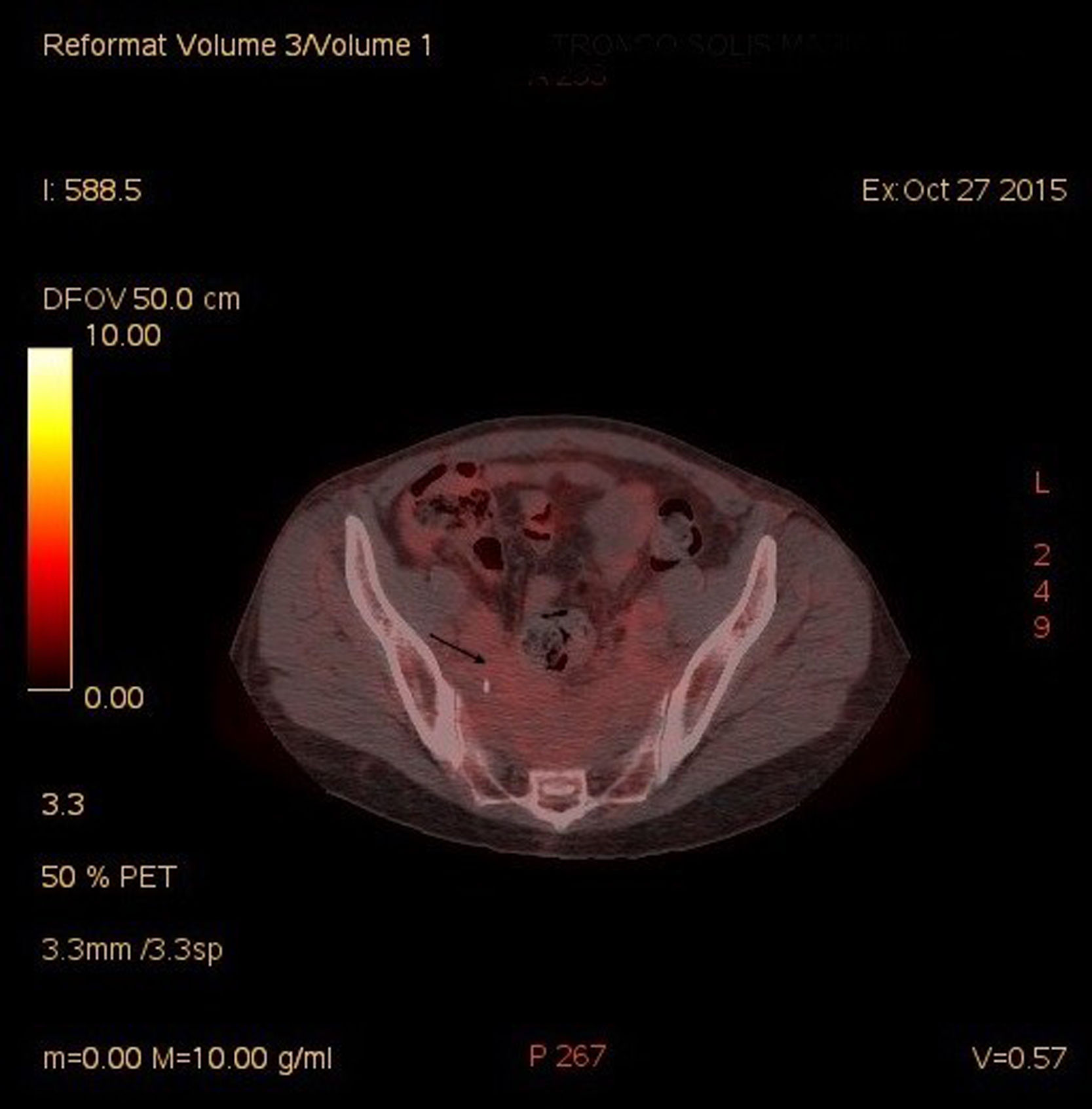
A thoracic-abdominal CT scan showed an extensive area of retroperitoneal (RPF) and pelvic fibrosis with bilateral ureterohydronephrosis. Subsequently a PET-CT scan with 18F-FDG (Fig. 1) confirmed the mass of soft tissues in front of the sacrococcygeal region, with low glucidic avidity (SUVmax: 2.16 g/ml).
Given these findings a double J catheter was implanted and the fibrotic retroperitoneal lesions were biopsied. In the valves resected 2 years previously and in the retroperitoneal lesions only areas of fibrosis with negative immunofluorescence for IgG4 were observed.
The patient then remembered taking Hemicraneal® (paracetamol, caffeine and 2 mg ergotamine tartrate) almost every day for several years in suppository format for headaches, without medical prescription.
It was finally assumed that the RPF as well as the valvulopathy were side effects of the ergotamines.
RPF is a fibroinflammatory disease that is now considered to be within the spectrum of diseases associated with IgG4, although it has also been associated with other systemic diseases.4 Differential diagnosis of this disease includes carcinoid tumours, actinomycosis, radiotherapy or abdominal surgery and Erdheim-Chester’s disease, although drugs also have to be considered. They include anti-migraine medication (metisergide and ergotamine), dopaminergic agonists used in Parkinson’s disease (pergolide and cabergoline), anorexigenic drugs (fenfluramine, dexfenfluramine and benfluorex) and anti-TNF5 drugs. However, the list includes recreational drugs as well, such as 3,4-methylenodioxymethamphetamine, known as ecstasy.6 These drugs have strong affinity for the 5HT28 serotonin receptor that is found in valvular tissue, and they cause lesions similar to those observed in carcinoid tumours, with thickening and accumulation of collagen and the proliferation of myofibroblasts and smooth muscle cells.
Ergotamine is used as migraine prophylaxis. It is sold over the counter and its use is contraindicated in Raynaud as it causes vasospasm. The first case of valvulopathy due to ergotamines was described in 19745 and, although its toxicity is well-known, it is rarely diagnosed. It is probably under-diagnosed as it is taken without supervision, and its toxicity appears after prolonged use.6,7
Our patient, with limited SD, developed valvulopathy and RPF due to ergotamines. Although both toxicities are well-known, they are exceptional in the same patient. On the other hand, the association of SD and RPF, profibrotic diseases that may have similar physiopathological mechanisms, is exceptional.8,9 In spite of sophisticated current diagnostic procedures, our diagnosis is still based on directed anamnesis, which is often overlooked. In SD, as is the case for other systemic diseases,10 other processes and drugs which may simulate their clinical manifestations must always be taken into account.
FinancingThis research received no specific grant from any agency in the public or private sector or those which are not-for-profit.
Please cite this article as: Suárez Pérez L, Caminal Montero L, Trapiella Martínez L, Rugeles Niño J. Valvulopatía en la esclerodermia, no siempre es autoinmunidad. Reumatol Clin. 2021;17:57–58.