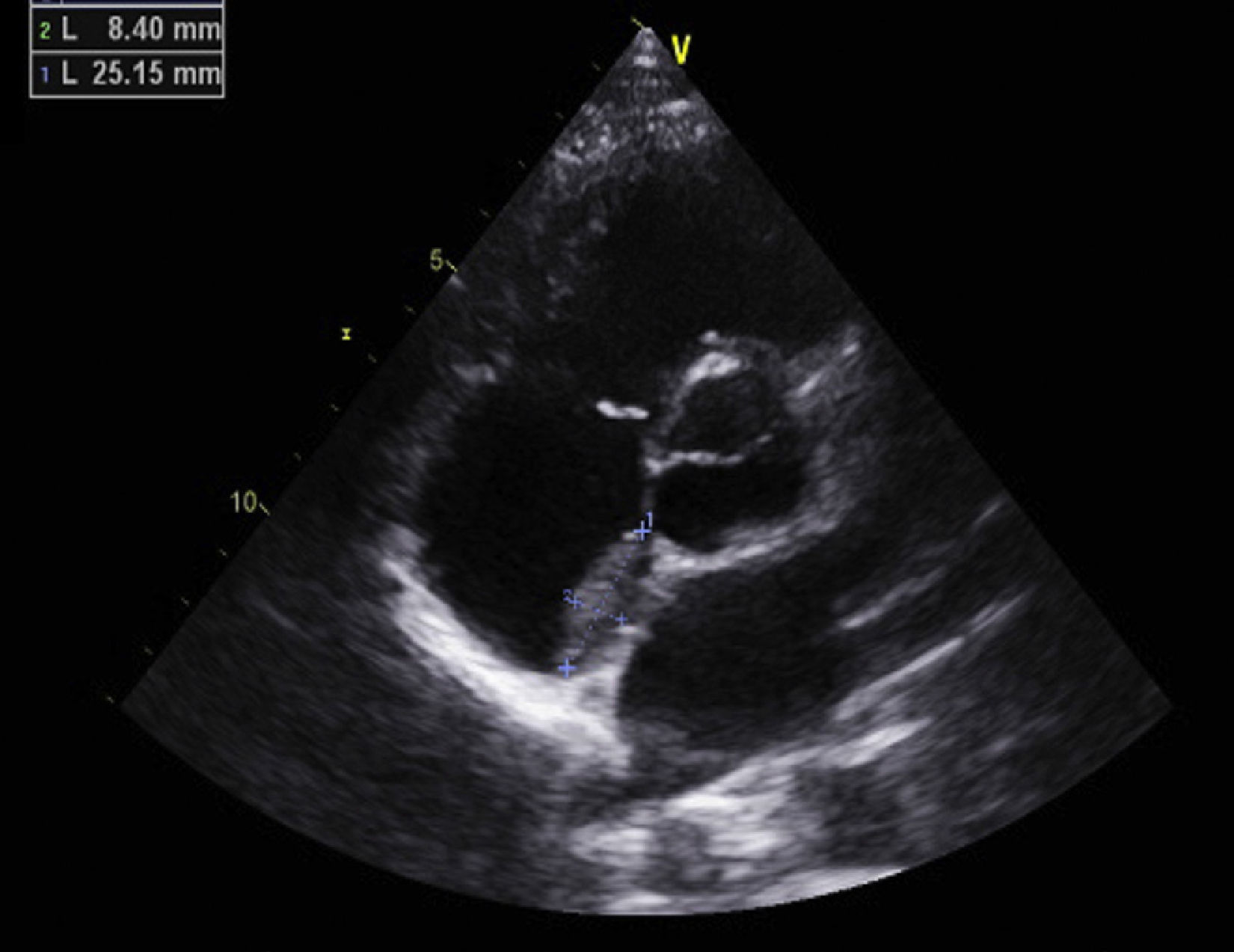
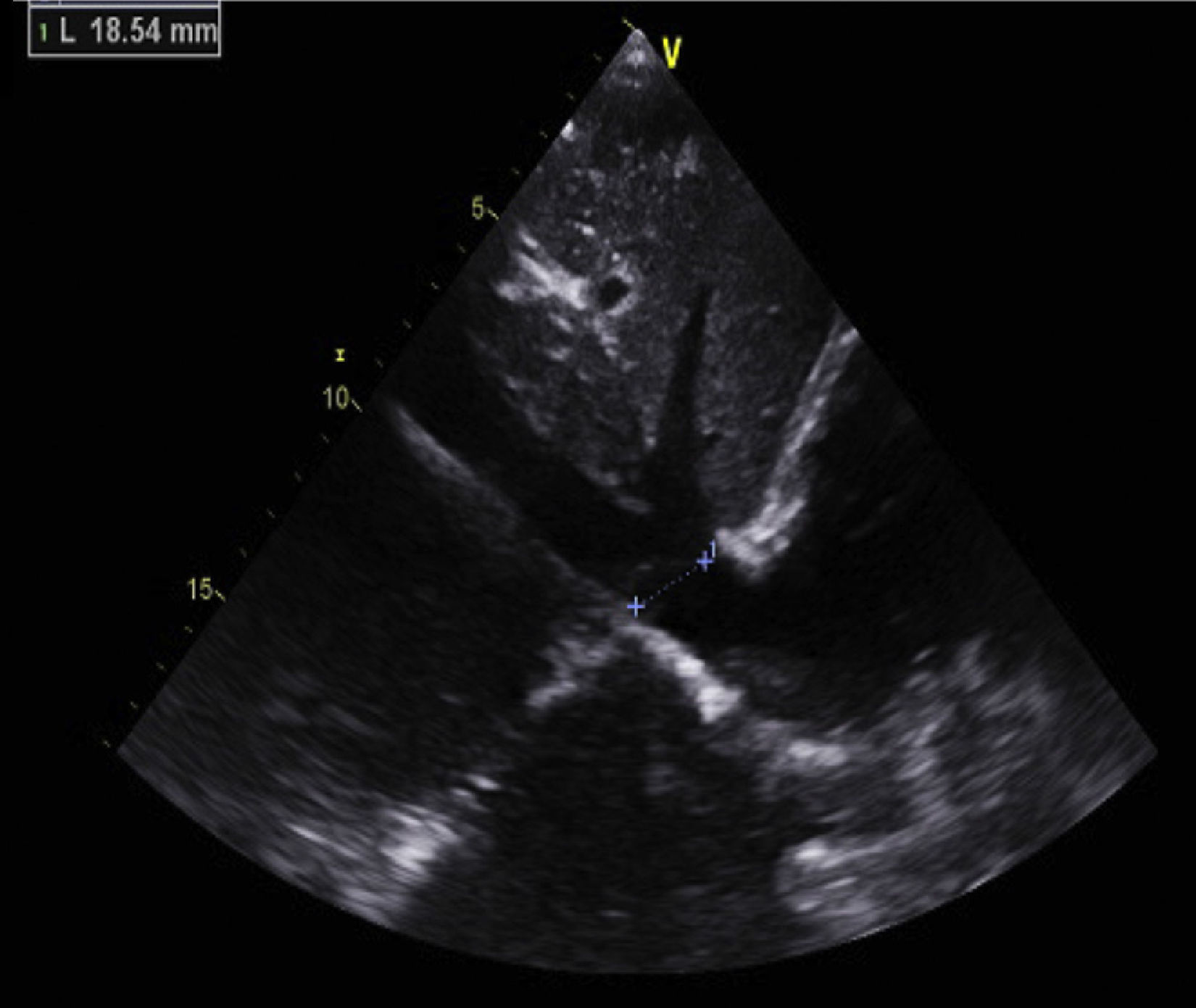
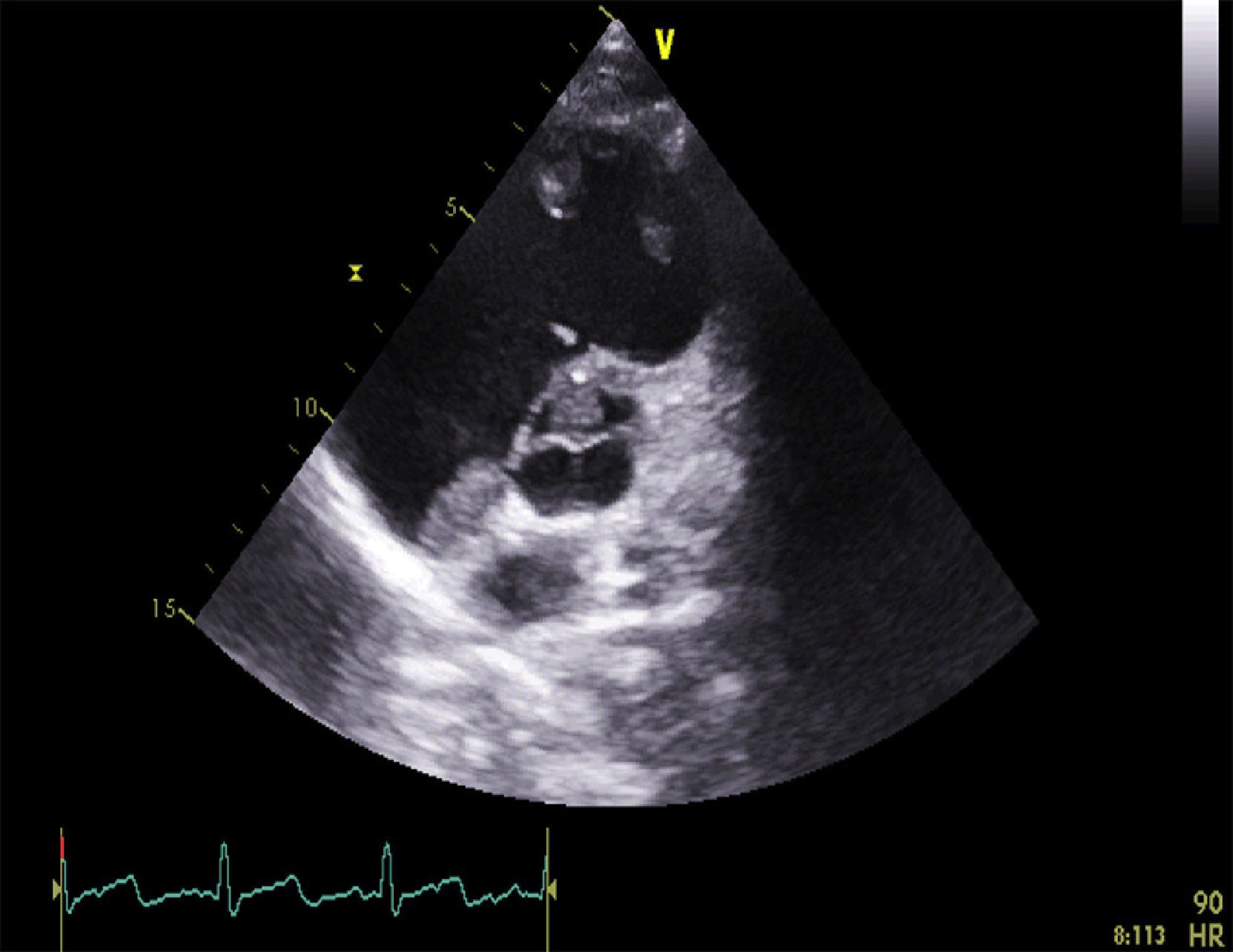
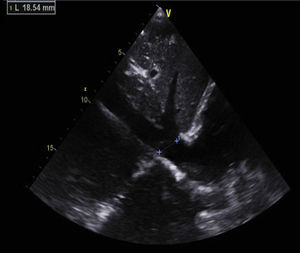
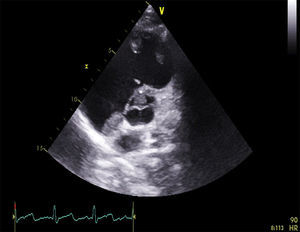
Antiphospholipid syndrome (APS) is an autoimmune disease, with antiphospholipid antibodies associated with hypercoagulability, vascular thrombosis, and fetal loss.1,2 Cardiac involvement occurs frequently, and is deeply related to hypercoagulability in spite of recommended anticoagulant therapy.3 In this report, we describe the images of a Caucasian 19-year-old male, with a previous history, 4 years earlier, of an acute in situ right chamber thromboembolic episode submitted to a surgical intracardiac thrombectomy. At this time APS was diagnosed with increased levels of lupus anticoagulant and IgM anti-beta(2)-glycoprotein I. All other autoantibodies were negative. He was readmitted in April 2012 with an initial suspicion of endocarditis. Intracardiac and inferior vena cava thrombi as well as acute and chronic pulmonary thromboembolism were detected in spite of adequate anticoagulation. After full dose anticoagulation he improved well and was discharged. In September 2012 he was readmitted after 2 weeks of fever, dyspnea and left thoracic pain again with pulmonary thromboembolism. Transthoracic echocardiogram (TTE) revealed an image suggestive of a thrombus at the upper part of the atrial septum in the right atrium (25×8mm), Image 1, and in the inferior vena cava (18mm) near the roof of the right atrium, Image 2. Also in the infundibulum of the right ventricle and in the right ventricular outflow tract several freely moving masses were visualized, indicative of thrombus near the lateral wall, Image 3. A long course of antibiotic was done and all microbiological tests proved negative. Hydroxychloroquine and colchicine were added to an intensive antithrombotic regimen of acenocumarol, enoxaparin and acetylsalicylic acid with a significant reduction of the right atrium and inferior vena cava thrombi and a complete disappearance of the right ventricular masses. The patient improved clinically and no further relapses were observed during follow-up.
Ethical responsibilitiesProtection of people and animalsThe authors declare that no experiments were performed on humans or animals for this study.
Data confidentialityThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors declare no conflict of interest.