There is no updated information on epidemiology and cost of management of non infectious uveitis (NIU) in Spain. This study assessed the frequency of various types of uveítis as well as associated costs of resources used in their management.
Material and methodNIU epidemiological data and direct costs were collected from a literature search. This was complemented with consensus information from 2 expert panel meetings and data from questionnaires to ophthalmologists and rheumatologists, experts on these conditions. Healthcare resources costs were obtained from the Oblikue database, from a medical society and from approved drug prices in Spain.
ResultsDuring 2011 the estimate number of NIU was 9398 (45% male, 70% aged 16–65 years). Incidence per type of uveitis was: acute anterior uveitis (AAU) 55%; posterior uveitis (PU) and pan-uveitis (PanU) 15% each; adult chronic anterior uveitis, pediatric chronic anterior uveitis and intermediate uveitis 5% each. Among total costs (77,834,282.10€), initial drug therapy was the highest (43,602,359.29€), followed by surgical treatment of complications (8,367,420.43€). With respect to types of uveitis, PanU (26,692,948.29€), PU (22,283,330.50€) and AAU (14,336,755.38€) showed the highest associated costs.
ConclusionsNon infectious uveitis is associated to high costs in Spain, both in its diagnosis and in its treatment. Early diagnosis and treatment should allow for substantial savings for the National Health System.
No existen datos actualizados sobre la epidemiología y los costes asociados de la uveítis no infecciosa (UNI) en España. Este estudio investiga la frecuencia de los tipos de uveítis y el coste de los recursos utilizados en su manejo en 2011.
Material y métodoSe recogió información mediante búsqueda bibliográfica de datos epidemiológicos y de costes directos de la UNI. La información se completó mediante consenso de 2 paneles de expertos y cuestionario a oftalmólogos y reumatólogos especialistas en esta enfermedad. Los costes de los recursos se obtuvieron de la base de datos Oblikue, de una sociedad médica y de los precios de los medicamentos aprobados en España.
ResultadosEn 2011 se diagnosticaron 9.398 nuevos pacientes de UNI (45% hombres, el 70% entre 16 y 65 años). La incidencia por tipos fue: uveítis anterior aguda (UAA) 55%, uveítis posterior (UP) y panuveítis (PU) 15% y uveítis anterior crónica en edad adulta, uveítis anterior crónica pediátrica y uveítis intermedia 5%. Del total de costes calculados (77.834.282,10€), el tratamiento farmacológico inicial fue el recurso más costoso (43.602.359,29€), seguido del tratamiento quirúrgico de las complicaciones (8.367.420,43€). Respecto a los tipos de uveítis, los costes asociados más elevados fueron los de la PU (26.692.948,29€), la UP (22.283.330,50€) y la UAA (14.336.755,38€).
ConclusionesLa UNI en España genera unos elevados costes tanto de diagnóstico como de tratamiento. Un diagnóstico y tratamiento precoz de la enfermedad permitirían un ahorro sustancial al Sistema Nacional de Salud.
The term uveitis comprises a range of inflammatory conditions affecting the uvea, the middle layer of the eye that supplies most of the blood flow to the retina.1 The most widely used classification, based on the primary anatomic location of the inflammation, was established by the International Uveitis Study Group (IUSG 1987) and distinguishes among anterior, intermediate and posterior uveitides and panuveitis.1,2 These conditions are also classified as chronic, acute or recurrent.3
The etiology of uveitis is variable, and the disorder can present as an exclusively ocular process or be associated with systemic infectious or immunological diseases. Developed countries report fewer cases of infectious uveitis. According to Spanish and international data, patients diagnosed with ankylosing spondylitis, reactive arthritis, psoriatic arthritis or inflammatory bowel disease have a possibility of developing uveitis of 20%–30%, 12%–37%, 7%–16%, and 2%–9%, respectively.4–7 On the other hand, uveitis is often the first clinical manifestation of spondyloarthritis,8–10 the diagnosis of which may be delayed by between 5 and 10 years,4 and 10%–23% of the patients with uveitis have some form of spondyloarthritis.
Uveitis is considered a severe disease, with serious sequelae, that causes between 5% and 20% of the cases of legal blindness and 10% of the cases of impaired vision,1,11 conditions that can be associated with different types of work disability. On the other hand, uveitis patients, a great majority of whom are of working age when diagnosed, must receive long-term drug therapy, with secondary effects and medical appointments that can result in lost productivity due to absenteeism. Even so, the economic impact generated by this disease and the social costs attributable to its morbidity are practically unknown.1
A retrospective study evaluated the annual use of resources in France for the follow-up of patients with uveitis12 and estimated mean direct costs of € 3403 per patient, € 2889 of which were due to hospital admissions. Another study performed in the United States analyzed the mean annual costs,13 which were US$ 8450 in patients with noninfectious uveitis (NIU). Outpatient admissions and drug therapy were the most costly items, representing 29% and 22% of the total cost, respectively.
The objective of this study was to estimate the cost to the Spanish Health System of NIU during the first year after diagnosis, using data on the resources utilized in its management during 2011. On the other hand, given the lack of published epidemiological data on this disease, the incidence we report is also an estimation.
Material and MethodsWe analyzed the information on the burden of NIU in Spain by means of a structured search of the literature and databases, including Cochrane Library Plus (the Spanish version of the Cochrane Library), PubMed/Medline, Center for Reviews and Dissemination, Índice Médico Español – Biomedicina, del Consejo Superior de Investigaciones Científicas (Spanish Medical Index for Biomedicine issued by the Spanish Scientific Research Council) and general searches using the terms “uveitis”, “economy” and “costs and cost analysis”. We evaluated the management, epidemiological data and direct costs of NIU, and found that there was little information on the epidemiological profile and cost of the disease. There was also very few references to its clinical management and on routine clinical practice due, among other factors, to the inexistence of Spanish clinical practice guidelines.
In view of this circumstance, we decided to conduct this study on the basis of information from primary and secondary references yielded by a literature review, using a technique involving expert panel consensus to evaluate data not found in the publications.
The consensus technique consisted of the formation of a panel of 5 experts, 2 ophthalmologists and 3 rheumatologists, members of units dedicated to uveitis in Spanish tertiary level hospitals.
The experts were invited to openly express their opinions, using paper-and-pencil exercises, on each item and on the data obtained from the literature search. Their opinions were used to formulate a structured questionnaire with queries on epidemiology (incidence and frequency of the different clinical forms of uveitis) and on the use of resources in the management of each of these forms (medical costs, diagnostic procedures, drug therapies, surgical procedures and complications, such as cataracts and glaucoma). The responses were analyzed and averaged, and the experts were invited to participate in a second panel in which they scored their degree of consensus and formulated preliminary considerations regarding the subjects of interest. A third round of consensus building involving those data for which the degree of consensus was lowest was carried out by electronic mail.
On the basis of the incidence rates in the United States,14 the panel agreed on the value most representative of the Spanish scenario in 2 consensus meetings. That value, adjusted for sex and age,15 was utilized to estimate the number of new cases in 2011.
This procedure enabled the calculation of the resources consumed in diagnostic procedures, hospital pharmacy supplies, outpatient treatment of the disease and of its complications for the first year from the time of diagnosis.
To calculate the direct costs of NIU, we first estimated the allocation of resources for each of the following line items: costs of referral (visits to primary care, to specialists or to the emergency department prior to diagnosis); of diagnosis (visits to specialists, tests required for the initial diagnosis); of treatment (drugs and their outpatient administration for initial treatment and treatment of flares); of follow-up (visits to specialists, diagnostic tests); and of complications (surgery, emergency department visits).
Using the data on resource use resulting from the expert consensus, we calculated the direct costs.
Per unit costs were assigned to the resources to be evaluated. As the Spanish Health System does not record information on prices or costs per disease process, we reviewed prices and rates in Spain and chose the most recent rates published by the Spanish autonomous communities, hospitals and medical societies, updated for 2011. We searched the official daily gazettes and bulletins of the autonomous communities in the Oblikue database,16 which provides economic information on the health care sector, and that of the Col-legi Oficial de Metges (Medical Association) of Barcelona, Spain.17
We calculated the cost of drugs according to the mode of administration: topical, oral, systemic injection or intraocular injection. Thirteen types of drugs were taken into account, including mydriatic and cycloplegic agents, topical and systemic corticosteroids, sulfasalazine, antimetabolites, and T-cell and anti-TNF inhibitors. The cost of patient self-administration was included in that of the medication only for topical and oral formulations. Systemic corticosteroids, which were infused in the outpatient setting, were included in the day hospital costs, whereas the intraocular drugs administered in the specialist's office were added to the costs of the visit.
The monetary value of drug therapy was calculated on the basis of the average costs of the regimens and the therapeutic agents agreed on by the experts, taking into account the average cost of acquisition from the manufacturer (plus value added tax) reflected in the Integra database of February 2012, issued by the Spanish Ministry of Health.18,19 None of the deductions or discounts applied to the price of medications in the hospitals were taken into account due to the lack of data.
For the calculation of the cost of treatment administered in a specialist's office or in an outpatient setting, we considered it to be fully funded by the Spanish Health System. For all other drug therapies, we considered that, in the case of patients of working age, identified according to the incidence data, the system financed 40% of the cost.
To the costs of outpatient treatment, as well as the surgical procedures required to treat complications, we added the costs of visits to the physician, visits to the day hospital and hospital admissions.
Finally, we quantified overall costs and mean costs per patient according to the type of resource, the frequency and percentage of patients, as well as the incidence, in accordance with the following forms of NIU: acute anterior uveitis (AAU), adult chronic anterior uveitis, pediatric chronic anterior uveitis, posterior uveitis (PU), intermediate uveitis (IU) and panuveitis.
ResultsTable 1 shows the estimated incidence of each type of NIU, together with the cost per patient and overall costs. When we extrapolated the data in the literature to the Spanish population in 2011, adjusted for age and sex, we estimated that there would be 9398 new cases of NIU in 2011, meaning a rate of 20 new cases per 100,000 population, 55% in women and 70% in individuals aged 16–65 years.
Incidence, Overall Costs and Cost per Patient According to the Type of Noninfectious Uveitis in Spain in 2011.
| Type of uveitis | Proportion of all noninfectious uveitides (%) | Overall annual cost (€) | Cost/patient/year (€) |
|---|---|---|---|
| Panuveitis | 15 | 26,692,948.29 | 18,922.35 |
| Posterior uveitis | 15 | 22,283,330.50 | 15,919.52 |
| Acute anterior uveitis | 55 | 14,336,755.38 | 2811.17 |
| Pediatric chronic anterior uveitis | 5 | 7,397,824.68 | 15,738.93 |
| Intermediate uveitis | 5 | 4,211,846.42 | 6889.17 |
| Adult chronic anterior uveitis | 5 | 2,911,576.83 | 6080.30 |
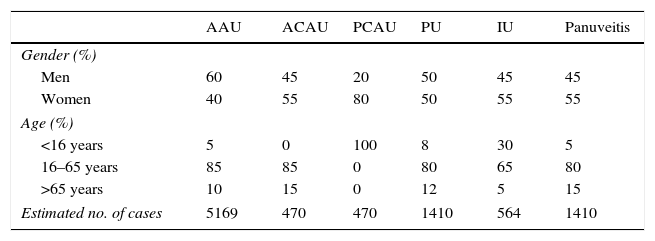
Acute anterior uveitis was the NIU most frequently diagnosed (55%). Table 2 shows the distribution of NIU by gender, age and type of uveitis.
Number of Cases and Distribution According to Gender, Age and Type of Noninfectious Uveitis in Spain in 2011.
| AAU | ACAU | PCAU | PU | IU | Panuveitis | |
|---|---|---|---|---|---|---|
| Gender (%) | ||||||
| Men | 60 | 45 | 20 | 50 | 45 | 45 |
| Women | 40 | 55 | 80 | 50 | 55 | 55 |
| Age (%) | ||||||
| <16 years | 5 | 0 | 100 | 8 | 30 | 5 |
| 16–65 years | 85 | 85 | 0 | 80 | 65 | 80 |
| >65 years | 10 | 15 | 0 | 12 | 5 | 15 |
| Estimated no. of cases | 5169 | 470 | 470 | 1410 | 564 | 1410 |
AAU, acute anterior uveitis; ACAU, adult chronic anterior uveitis; IU, intermediate uveitis; PCAU, pediatric chronic anterior uveitis; PU, posterior uveitis.
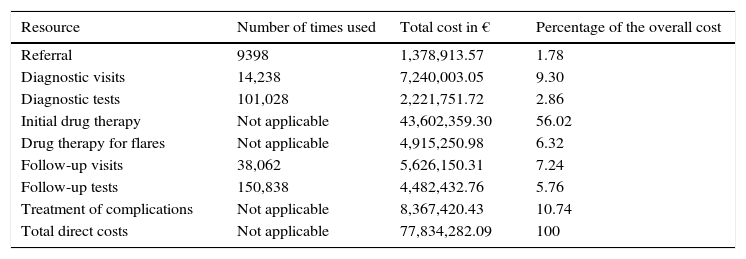
The overall cost during 2011 was € 77,834,282.10. The cost of initial drug therapy was the largest expenditure, amounting to € 43,602,359.29. Table 3 details the use of resources, the overall annual cost and the percentage.
Use of Resources and Total Costs of Noninfectious Uveitis in Spain in 2011.
| Resource | Number of times used | Total cost in € | Percentage of the overall cost |
|---|---|---|---|
| Referral | 9398 | 1,378,913.57 | 1.78 |
| Diagnostic visits | 14,238 | 7,240,003.05 | 9.30 |
| Diagnostic tests | 101,028 | 2,221,751.72 | 2.86 |
| Initial drug therapy | Not applicable | 43,602,359.30 | 56.02 |
| Drug therapy for flares | Not applicable | 4,915,250.98 | 6.32 |
| Follow-up visits | 38,062 | 5,626,150.31 | 7.24 |
| Follow-up tests | 150,838 | 4,482,432.76 | 5.76 |
| Treatment of complications | Not applicable | 8,367,420.43 | 10.74 |
| Total direct costs | Not applicable | 77,834,282.09 | 100 |
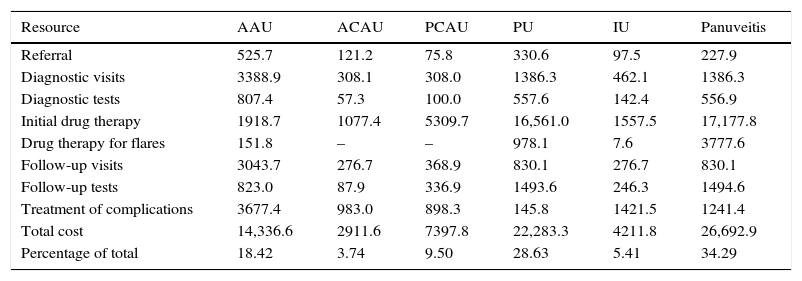
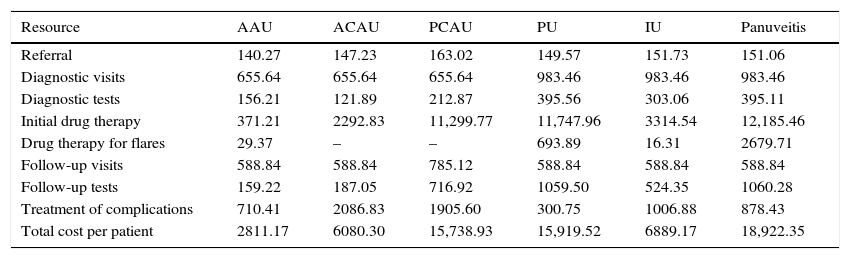
Panuveitis was the most costly form (€ 26,692,948.29) followed by PU (€ 22,283,330.50) and AAU (€ 14,336,755.38). The total cost per patient ranged from € 2811.17 for AAU to € 18,922.35 for PU. Tables 4 and 5 show, respectively, the overall costs and the cost per patient corresponding to each line item, according to the type of uveitis.
Total Costs (in Thousands of €) per Type of Noninfectious Uveitis in Spain in 2011.
| Resource | AAU | ACAU | PCAU | PU | IU | Panuveitis |
|---|---|---|---|---|---|---|
| Referral | 525.7 | 121.2 | 75.8 | 330.6 | 97.5 | 227.9 |
| Diagnostic visits | 3388.9 | 308.1 | 308.0 | 1386.3 | 462.1 | 1386.3 |
| Diagnostic tests | 807.4 | 57.3 | 100.0 | 557.6 | 142.4 | 556.9 |
| Initial drug therapy | 1918.7 | 1077.4 | 5309.7 | 16,561.0 | 1557.5 | 17,177.8 |
| Drug therapy for flares | 151.8 | – | – | 978.1 | 7.6 | 3777.6 |
| Follow-up visits | 3043.7 | 276.7 | 368.9 | 830.1 | 276.7 | 830.1 |
| Follow-up tests | 823.0 | 87.9 | 336.9 | 1493.6 | 246.3 | 1494.6 |
| Treatment of complications | 3677.4 | 983.0 | 898.3 | 145.8 | 1421.5 | 1241.4 |
| Total cost | 14,336.6 | 2911.6 | 7397.8 | 22,283.3 | 4211.8 | 26,692.9 |
| Percentage of total | 18.42 | 3.74 | 9.50 | 28.63 | 5.41 | 34.29 |
AAU, acute anterior uveitis; ACAU, adult chronic anterior uveitis; IU, intermediate uveitis; PCAU, pediatric chronic anterior uveitis; PU, posterior uveitis.
Costs (€) and Resources Used per Patient According to Type of Noninfectious Uveitis in Spain in 2011.
| Resource | AAU | ACAU | PCAU | PU | IU | Panuveitis |
|---|---|---|---|---|---|---|
| Referral | 140.27 | 147.23 | 163.02 | 149.57 | 151.73 | 151.06 |
| Diagnostic visits | 655.64 | 655.64 | 655.64 | 983.46 | 983.46 | 983.46 |
| Diagnostic tests | 156.21 | 121.89 | 212.87 | 395.56 | 303.06 | 395.11 |
| Initial drug therapy | 371.21 | 2292.83 | 11,299.77 | 11,747.96 | 3314.54 | 12,185.46 |
| Drug therapy for flares | 29.37 | – | – | 693.89 | 16.31 | 2679.71 |
| Follow-up visits | 588.84 | 588.84 | 785.12 | 588.84 | 588.84 | 588.84 |
| Follow-up tests | 159.22 | 187.05 | 716.92 | 1059.50 | 524.35 | 1060.28 |
| Treatment of complications | 710.41 | 2086.83 | 1905.60 | 300.75 | 1006.88 | 878.43 |
| Total cost per patient | 2811.17 | 6080.30 | 15,738.93 | 15,919.52 | 6889.17 | 18,922.35 |
AAU, acute anterior uveitis; ACAU, adult chronic anterior uveitis; IU, intermediate uveitis; PCAU, pediatric chronic anterior uveitis; PU, posterior uveitis.
The costs of referral to the tertiary care hospital where the diagnostic study was performed includes referrals from emergency departments, other hospitals, primary care ophthalmology departments and other consulted specialists. The mean cost of referral ranged between € 140.27 and € 163.02.
The diagnosis of AAU required 2 visits and PU, IU and panuveitis required 3. Both an ophthalmologist and a rheumatologist were present during each diagnostic visit. Thus, the costs of diagnostic visits ranged between € 655.64 and € 983.46, depending on the type of uveitis. The costs of diagnostic tests also varied according to the type of uveitis. The overall costs of referrals, visits and diagnostic tests amounted to € 10,840,668.34.
The total cost of drug therapy was € 43,602,359.29. However, certain drugs were administered more frequently to patients with more than 3 episodes a year (recurrent disease). The total annual cost of the management of recurrences was € 4,915,250.98. The overall cost of follow-up was estimated to be € 10,108,583.06.
A percentage of patients developed complications secondary to the disease that required surgery; moreover, they visited the emergency department with certain frequency. The cost per patient of visits to the emergency department ranged between € 2123.26 for IU and € 5400.49 for AAU. On the other hand, the per unit cost for each surgical procedure was € 127 for iridotomy, € 1036 for cataract surgery, € 1270 for vitrectomy and € 2935 for glaucoma surgery. Taking into account the mean number of procedures per type of uveitis, the costs ranged between € 49 for iridotomy in AAU and € 1415 for glaucoma surgery in adult chronic anterior uveitis. The annual cost of the treatment of complications and related visits to the emergency department was € 8,367,420.43.
DiscussionCurrent data for Spain11 indicate that the most common form of uveitis is AAU, although PU and panuveitis are also frequent findings, and the results of this study agree with this affirmation. The various forms of uveitis have different etiologies. Acute anterior uveitis associated with spondyloarthropathies and HLA-B27 positivity is the most common of the known etiologies. The etiology of this condition is a determinant of the resources required for the diagnosis, treatment and follow-up.
The largest expenditure in all the forms of uveitis was that corresponding to initial treatment (€ 43,602,359.29), constituting 56% of the overall costs (€ 77,834,282.10). The second most costly line item was that corresponding to the surgical treatment of complications (€ 8,367,420.43), 10.7% of the total. None of these surgical procedures required hospital stays, except in pediatric patients. In contrast, some of the drug therapies did generate hospital costs for their administration, generally ambulatory stays. This fact, and not only the cost of the drug, increases the expenditure corresponding to initial drug therapy, which is consumed by 100% of the patients.
The finding of a mean annual cost per patient (direct costs) for the management of NIU of between € 6000 and € 19,000, depending on the form of uveitis, is especially noteworthy. These figures are higher than those corresponding to more prevalent conditions, such as hypertension (€ 1200)20 and type 2 diabetes (€ 1305),21 but not as elevated as those reported for cancer (€ 24,800).22
Regarding the forms of uveitis, in 2011, the total cost of AAU (€ 14,336,755.38), the most prevalent form, was lower than the costs of PU (€ 22,283,330.50) and of panuveitis (€ 26,692,948.29). This was due to the cost of the drug therapy, which, in the latter 2 cases, was more intensive and was administered more frequently. The number of drugs needed to treat recurrences is generally greater in PU and panuveitis, and they are usually required in a larger number of cases. Drug therapy for adult and pediatric chronic anterior uveitides and intermediate uveitis was much less expensive and, since there were no recurrences, the overall costs were also much lower (€ 2,911,576.82, € 7,397,824 and € 4,211,846.42, respectively).
In future studies, researchers could investigate whether the prevention or adequate treatment of PU and panuveitis would reduce their economic burden and, thus, the overall burden of the management of NIU.
The cost of follow-up tests in PU and panuveitis was higher than that found in other forms of uveitis. Although the incidence of AAU was greater, the cost of the follow-up tests was also lower because the percentage of patients requiring these tests proved to be smaller. However, autofluorescence was performed only in PU and panuveitis (70% of the cases), a circumstance that explains the higher cost in these 2 forms.
The results of our study are in line with those of a recent report13 in which the costs of outpatient admissions and drug therapy were the major expenditures (29% and 22%, respectively) and in which IU, PU and panuveitis had higher annual costs than AAU. However, in contrast to our findings, a study conducted in France12 reported that the number of hospital stays represented the largest expenditure and was associated with indirect costs. However, due to the differences in clinical management, these results are not comparable as they do not involve the same hospital resources.
In the present study, the data on the use of resources were based on the clinical experience of ophthalmologists and rheumatologists from tertiary care hospitals with multidisciplinary uveitis clinics. This circumstance probably produces bias since the management of this disease in primary care centers and nonreferral hospitals was not taken into account. Likewise, these tertiary centers may have more efficient care management strategies, for example, arranging for patients to be seen by 2 specialists during each visit, which could reduce work absenteeism. Thus, the figures provided here may underestimate the total costs of the disease. Another limitation related to the data is the fact that the referral centers carry out a closer follow-up only of the most serious cases of uveitis, referring other patients to a lower level of care. This may mask the incidence of certain forms of uveitis, for example, AAU, among the general population.
The management of NIU depends on the type, its etiology, the complications, the course and associated systemic diseases. There is no treatment algorithm for this management in Spain. Thus, although the information on the clinical experience of the specialists involved in this study is based on referral data, it may not reflect clinical practice in some Spanish centers.
Another limitation of the study is the fact that the indirect costs due to absences from work to keep medical appointments and to the blindness that this disease can produce have not been estimated.
Noninfectious uveitis generates elevated diagnostic and therapeutic costs. Early diagnosis and treatment of the disease would result in a substantial savings for the Spanish Health System.
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
FundingThis study was financed by AbbVie Farmacéutica, S.L.U., Madrid, Spain.
Conflicts of InterestThe authors declare they have no conflicts of interest.
The authors thank IMS Health for their collaboration in the conduction of the study and their data analysis, as well as in the preparation of the draft of this article.
Please cite this article as: Adán-Civera AM, Benítez-del-Castillo JM, Blanco-Alonso R, Pato-Cour E, Sellas-Fernández A, Bañares-Cañizares A. Carga y costes directos de la uveítis no infecciosa en España. Reumatol Clin. 2016;12:196–200.