To determine the clinical profile, degree of involvement and management in patients with knee, hip or hand osteoarthritis.
MethodsObservational study (health centres from 14 autonomous regions, n=363 primary care physicians), involving patients with clinical and/or radiological criteria from the American College of Rheumatology, consecutively selected (n=1258). Sociodemographic variables, clinical and radiological findings, comorbidity and therapeutic management were analysed.
ResultsMean age was 68.0±9.5 years old; 77.8% were women and 47.6% obese. Distribution by location was 84.3% knee, 23.4% hip, and 14.7% hands.
All patients reported pain. The most frequent radiographic Kellgren-Lawrence grade was stage III for knee and hip (42.9% and 51.9%, respectively), and III (37.2%) and II (34.5%) for hip.
Time since onset of osteoarthritis symptoms was 9.4±7.5 years, with a mean age at onset of around 60 years and a family history of osteoarthritis in 66.0%.
The most frequent comorbidities were hypertension (55.1%), depression/anxiety (24.7%) and gastroduodenal diseases (22.9%).
A total of 97.6% of the patients received pharmacological treatment, with oral analgesics (paracetamol) (70.5%) and oral NSAIDs (67.9%) being the most frequent drugs.
Bilateral osteoarthritis was present in 76.9% of the patients with knee osteoarthritis, 59.3% in hip and 94.7% in hands. Female gender and time since onset were associated with bilateral knee and hip osteoarthritis.
ConclusionsThe profile of the osteoarthritis patient is female, >65 years old, overweight/obese, with a comorbidity, frequent symptoms and moderate radiologic involvement. Most of the patients had bilateral osteoarthritis, associated with female gender and time since onset of disease. Paracetamol was the most common pharmacological treatment.
Determinar el perfil clínico, afectación y tratamiento en pacientes con artrosis de rodilla, cadera y manos.
Material y métodoEstudio observacional (Centros de Salud de 14 Comunidades Autónomas, n=363 médicos). Se incluyen pacientes con criterios clínicos/radiológicos de artrosis del American College of Rheumatology, seleccionados consecutivamente (n=1258). Se analizan variables sociodemográficas, hallazgos clínico-radiológicos, comorbilidad y tratamiento.
ResultadosLa media de edad fue 68,0±9,5 años, 77,8% eran mujeres y 47,6% tenían obesidad. Un 84,3% tenían artrosis de rodilla, 23,4% de cadera y 14,7% de manos.
Todos los pacientes referían dolor. El grado radiológico de Kellgren-Lawrence más frecuente en rodilla y mano fue el III (42.9% y 51.9%, respectivamente), y en cadera grado III (37,2%) y II (34,5%).
El tiempo de evolución de los síntomas de artrosis fue 9,4±7,5 años, con edad de inicio alrededor de 60 años. El 66% de los pacientes tenían antecedentes de artrosis.
Las comorbilidades más frecuentes son: hipertensión (55,1%), depresión/ansiedad (24,7%) y patología gastroduodenal (22,9%).
Un 97,6% recibían tratamiento farmacológico, los más utilizados son: analgésicos orales (paracetamol) (70,5%) y AINES orales (67,9%).
Presentaban afectación bilateral el 76,9% de pacientes con artrosis de rodilla, 59,3% en cadera y 94,7% en manos. El sexo femenino y mayor tiempo de evolución se asocian a afectación bilateral en rodilla y cadera.
ConclusionesEl perfil del paciente artrósico es de mujer >65 años, con sobrepeso-obesidad, comorbilidad, clínica frecuente y afectación radiológica moderada. La mayoría presentan afectación bilateral, asociada al sexo femenino y tiempo de evolución. El paracetamol es el fármaco más utilizado.
Osteoarthritis is the most common disease of the joints in humans, which affects more than 70% of people older than 50 years and its prevalence clearly increases with age until 70 years old. The significance of the problem is determined by its prevalence, among other reasons, which increases due to ageing of the population and obesity epidemic. It is the principal cause of morbidity, activity limitation, functional incapacity and use of health care services.1
Its prevalence is not known with certainty, since data may vary depending on whether clinical or radiological studies have been conducted and on the criteria used to define the disease, age and sex of the participants, as well as the joint or joints included in the study. At the same time, we must distinguish between radiological and clinical osteoarthritis, since less than 50% of the population with radiological changes present symptoms of osteoarthritis and more than 70% of people older than 50 years have radiological signs of this disease somewhere.2,3
There is no unique treatment for osteoarthritis. In this sense, recommendations from the European League Against Rheumatism4–6 for osteoarthritis of the knee, hip and hand, as well as the osteoarthritis guidelines from the National Institute for Health and Care Excellence,7 consider that the treatment of osteoarthritis must be multimodal and combine non-pharmacological measures with pharmacological treatment. However, management variability leads to this disease being addressed in different ways as to the diagnosis and treatment.
In this context, this descriptive study was conducted on patients with osteoarthritis with the objective of determining the clinical profile and level of affection of patients with osteoarthritis of the hip, knee and/or hand, as well as to understand the therapeutic management of the disease in these patients on a national scale, within the multicentre project called: Clinical assessment of patients with osteoarthritis: project “EVALÚA”.
Material and MethodsStudy Design and AreaA multicentre, observational, cross-sectional and descriptive study has been conducted in 14 autonomous communities (comunidades autónomas, CC.AA.) of Spain: Andalusia, Aragon, Asturias, Balearic Islands, Canary Islands, Cantabria, Castilla-La Mancha, Valencian Community, Extremadura, Galicia, La Rioja, Madrid, Murcia and Navarre.
Study PopulationIn every participating CC. AA., primary care physicians interested in participating in the study were selected. Each participating physician had to include four patients throughout the four consecutive days, selecting the first patient of each day that met the inclusion criteria and agreed to participate in the study. Patients were asked to give their informed consent, and the confidentiality of the collected data was ensured, pursuant to the personal data protection law. The study obtained the approval of the Clinical Investigation Ethics Committee (Comité Ético de Investigación Clínica, CEIC) of the Autonomous Community of Galicia (CEIC Code –Galicia 2004/048) and has been supported by the Spanish Society of Family and Community Medicine.
The sampling scheme was prepared based on the entire Spanish population from every CC. AA., as per the 2001 census, prepared by the National Institute of Statistics, and it was stratified to obtain the total number of patients to be studied, keeping the proportions observed in the reference population. As a result, an expected sample size of 667 physicians and 2665 patients was obtained. Finally, 363 physicians of 14 CC. AA., who included 1434 patients, participated. Of these, 176 were excluded because they did not meet the established inclusion criteria. Therefore, the study includes information of 1258 patients with osteoarthritis of the knee, hip and/or hands, provided by 363 physicians. This sample size makes it possible to estimate the parameters of interest with a safety of 95% and an accuracy of ±3%, together with an estimated loss percentage of 15%.
The study included patients with osteoarthritis of the knee, hip and/or hands, as per the clinical and/or radiological criteria of osteoarthritis proposed by the American College of Rheumatology8 (ACR), who visited the participating health care centres during the study period and agreed to participate in it. Patients with osteoarthritis of the spine as the only location were excluded, as well as patients with osteoarthritis and other diagnoses regarding the knee, hip and/or hands, patients with chronic renal failure on dialysis, with a transplant or neurological sequelae secondary to a stroke. Furthermore, patients with a prosthesis due to osteoarthritis are also excluded, since we consider that this subgroup of patients would not permit the assessment of ACR radiological criteria in the first place, and they should be an independent study object for the assessment of their functional situation before and after the intervention.
Measurements and Measurement InstrumentsThe following variables were studied: (1) sociodemographic data; (2) diseases and concomitant medication; (3) clinical and/or radiological findings, pursuant to the ACR classification criteria for osteoarthritis of the hip, knee and hand; (4) radiological findings pursuant to the Kellgren-Lawrence classification,9 and (5) treatment: type of treatment, prescription origin (family physician, specialised doctor, private physician or self-medication) and daily dose.
Statistical AnalysisA descriptive analysis of all the collected variables was conducted. Numerical variables are presented with their average±standard deviation, median and range. Qualitative variables are expressed as a percentage and a 95% confidence interval (CI). For the comparison of quantitative variables, the following tests were used: Kolmogorov–Smirnov test, Student test, Mann–Whitney test or variance analysis. For qualitative variables, the square chi test or Fisher's exact test was used. To determine the variables associated with events of interest (bilateral affection), a multivariate logistic regression analysis was performed. The statistical analysis was conducted with SPSS 15.0 and Epidat 3.1 software for Windows.
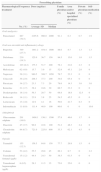
ResultsThe general characteristics of included patients are shown in Table 1. The average age of participants is 68.0±9.5 years, and 77.8% are women. 38.9% are overweight and 47.6% are obese.
General Characteristics of Patients With Osteoarthritis Included in the Study.
| No. | Average±SD | Median | |
|---|---|---|---|
| Age (years) | 1251 | 68.0±9.5 | 69 |
| BMI | 1227 | 30.4±5.1 | 29.7 |
| n | % | 95% CI | |
|---|---|---|---|
| Sex | |||
| Male | 279 | 22.2 | 19.8–24.5 |
| Female | 979 | 77.8 | 75.5–80.1 |
| BMI | |||
| Normal weight (BMI<25) | 165 | 13.5 | 11.5–15.4 |
| Overweight (BMI 25–29.9) | 477 | 38.9 | 36.1–41.6 |
| Obesity (BMI≥30) | 585 | 47.6 | 44.8–50.5 |
| Current smoker | 88 | 7.4 | 5.9–8.9 |
| Level of education | |||
| No education | 383 | 30.9 | 28.2–33.5 |
| Primary education | 697 | 56.2 | 53.4–59.0 |
| Secondary education | 127 | 10.2 | 8.5–12.0 |
| Tertiary education | 34 | 2.7 | 1.8–3.7 |
| Employment situation | |||
| Active | 168 | 13.5 | 11.6–15.4 |
| Unemployed | 10 | 0.8 | 0.3–1.3 |
| Retired | 375 | 30.1 | 27.5–32.7 |
| Housewife | 691 | 55.5 | 52.7–58.3 |
| Location | |||
| Knee | 812 | 64.5 | 61.9–67.2 |
| Hip | 118 | 9.4 | 7.7–11.0 |
| Hands | 75 | 6.0 | 4.6–7.3 |
| Knee+hip | 143 | 11.4 | 9.6–13.2 |
| Knee+hand | 76 | 6.0 | 4.7–7.4 |
| Hip+hand | 5 | 0.4 | 0.1–0.9 |
| Knee+hip+hand | 29 | 2.3 | 1.4–3.2 |
| Comorbidities | |||
| High blood pressure | 693 | 55.1 | 52.3–57.9 |
| Depression/Anxiety | 311 | 24.7 | 22.3–27.1 |
| Gastroduodenal pathology | 288 | 22.9 | 20.5–25.2 |
| Diabetes | 243 | 19.3 | 17.1–21.5 |
| Dyspepsia | 129 | 10.3 | 8.5–12.0 |
| GERD/hiatal hernia | 130 | 10.3 | 8.6–12.0 |
| Ischaemic cardiopathy | 88 | 7.0 | 5.5–8.4 |
| Heart failure | 71 | 5.6 | 4.3–6.9 |
| COPD | 65 | 5.2 | 3.9–6.4 |
| Chronic headache | 60 | 4.8 | 3.5–6.0 |
| Asthma | 57 | 4.5 | 3.3–5.7 |
| Angina | 51 | 4.1 | 2.9–5.2 |
| Gastroduodenal ulcer | 31 | 2.5 | 1.6–3.4 |
| Infarction | 27 | 2.1 | 1.3–3.0 |
| Neoplasia | 22 | 1.7 | 1.0–2.5 |
| Upper gastrointestinal bleeding | 12 | 1.0 | 0.4–1.5 |
| Lower gastrointestinal bleeding | 7 | 0.6 | 0.1–1.0 |
| Concomitant medication | |||
| Anticoagulation | 43 | 3.4 | 2.4–4.5 |
| Glucocorticoids | 18 | 1.4 | 0.7–2.1 |
| Low dose aspirin | 170 | 13.5 | 11.6–15.4 |
| Gastroprotection | 696 | 55.3 | 52.5–58.1 |
SD, standard deviation; COPD, chronic obstructive pulmonary disease; GERD, gastroesophageal reflux disease; CI, confidence interval; BMI, body mass index.
The most commonly found comorbidities include: high blood pressure (55.1%), depression/anxiety (24.7%), gastroduodenal pathology (22.9%) and diabetes (19.3%). In relation to concomitant medication, the most common is gastroprotection (55.3%) and, in particular, proton pump inhibitors (45.0%) (Table 1). 84.3% of the participants had osteoarthritis of the knee, 23.4%, osteoarthritis of the hip and 14.7%, osteoarthritis of the hands. The most common location was the knee, followed by the knee plus hip and hip (Table 1).
Pursuant to the ACR clinical criteria for the classification of osteoarthritis, all the patients presented pain in the last month in any of the locations of osteoarthritis (Table 2).
American College of Rheumatology Clinical Classification Criteria for Osteoarthritis According to the Location.
| n | % | 95% CI | |
|---|---|---|---|
| Osteoarthritis of the knee (n=1060) | |||
| Knee pain on most days of the previous month | 1060/1060 | 100 | 99.6–100.0 |
| Age ≥38 years | 1055/1056 | 99.9 | 99.5–100.0 |
| Bone crepitus elicited by active movements | 875/1059 | 82.6 | 80.3–84.9 |
| Morning stiffness of the knee ≤30min | 873/1060 | 82.4 | 80.0–84.7 |
| Joint hypertrophy, hard in consistency | 559/1050 | 53.2 | 50.2–56.3 |
| Osteoarthritis of the hip (n=295) | |||
| Hip pain on most days of the previous month | 295/295 | 100 | 98.7–100.0 |
| Age >50 years | 287/293 | 98.0 | 96.2–99.7 |
| Pain triggered by the internal rotation of the hip | 241/295 | 81.7 | 77.1–86.3 |
| Morning stiffness ≤60min | 235/295 | 79.7 | 74.9–84.4 |
| ESR ≤45mm/h | 153/292 | 52.4 | 46.5–58.3 |
| Internal rotation of the hip ≥15° | 136/295 | 46.1 | 40.2–51.9 |
| Internal rotation of the hip <15° | 120/295 | 40.7 | 34.9–46.4 |
| Hip flexion ≤115° | 98/295 | 33.2 | 27.7–38.8 |
| Osteoarthritis of the hands (n=185) | |||
| Pain, aches or stiffness in the joints of the hands on most days of the previous month | 185/185 | 100 | 98.0–100.0 |
| Joint hypertrophy, hard in consistency, in, at least, 2 of the 10 selected joints | 185/185 | 100 | 98.0–100.0 |
| Swelling signs present in less than 3 metacarpophalangeal joints | 185/185 | 100 | 98.0–100.0 |
| Joint hypertrophy, hard in consistency, in, at least, 2 distal interphalangeal joints of any finger | 137/183 | 74.9 | 68.3–81.4 |
| Joint deformity in, at least, one of the 10 selected joints | 129/176 | 73.3 | 66.5–80.1 |
CI, confidence interval; ESR, erythrocyte sedimentation rate.
Pursuant to the ACR radiological criteria for the classification of osteoarthritis (Table 3), no radiological findings were noted in a very low percentage of patients: 3% (95% CI of 1.7%–4.2%) in osteoarthritis of the knee, 2% (95% CI of 0.7%–4.7%) in osteoarthritis of the hip and 1.1% (95% CI of 0.1%–6.1%) in osteoarthritis of the hand. Pursuant to the Kellgren-Lawrence radiological classification, most of the patients with osteoarthritis of the knee and hand were classified as degree 3 (42.9% and 51.9%, respectively). Most of the patients with osteoarthritis of the hip were classified as degree 2 (34.5%) and degree 3 (37.2%) (Table 3). 66.0% (95% CI of 63.3%–68.7%) of the participants have family history of osteoarthritis. These patients are significantly younger (67.2±9.4 vs 69.0±9.3, P=.001) and mostly women (69.6% vs 53.6%, P<.001). The average time for the evolution of the osteoarthritis symptoms was 9.4±7.5 years, with a median of 8 years. The average age of onset of disease symptoms stood, in all cases, at around 60 years old.
American College of Rheumatology Radiological Classification Criteria for Osteoarthritis According to the Location.
| N | % | 95% CI | |
|---|---|---|---|
| Osteoarthritis of the knee | |||
| No pathological findings | 24/806 | 3.0 | 1.7–4.2 |
| Osteophytes | 655/806 | 81.3 | 78.5–84.0 |
| Subchondral sclerosis | 485/806 | 60.2 | 56.7–63.6 |
| Geodes or subchondral cysts | 113/806 | 14.0 | 11.6–16.5 |
| Joint space narrowing | 636/806 | 78.9 | 76.0–81.8 |
| Joint dislocations and/or altered bone alignment | 85/806 | 10.5 | 8.4–12.7 |
| Kellgren-Lawrence scale | |||
| Grade 0 | 6/734 | 0.8 | 0.1–1.5 |
| Grade 1 | 97/734 | 13.2 | 10.7–15.7 |
| Grade 2 | 200/734 | 27.2 | 23.9–30.5 |
| Grade 3 | 315/734 | 42.9 | 39.3–46.6 |
| Grade 4 | 116/734 | 15.8 | 13.1–18.5 |
| Osteoarthritis of the hip | |||
| No pathological findings | 5/245 | 2.0 | 0.7–4.7 |
| Osteophytes | 197/245 | 80.4 | 75.2–85.6 |
| Subchondral sclerosis | 135/245 | 55.1 | 48.7–61.5 |
| Geodes or subchondral cysts | 31/245 | 12.7 | 8.3–17.0 |
| Joint space narrowing | 204/245 | 83.3 | 78.4–88.1 |
| Joint dislocations and/or altered bone alignment | 11/245 | 4.5 | 1.7–7.3 |
| Kellgren-Lawrence scale | |||
| Grade 0 | |||
| Grade 1 | 34/223 | 15.2 | 10.3–20.2 |
| Grade 2 | 77/223 | 34.5 | 28.1–41.0 |
| Grade 3 | 83/223 | 37.2 | 30.6–43.8 |
| Grade 4 | 29/223 | 13.0 | 8.4–17.6 |
| Osteoarthritis of the hands | |||
| No pathological findings | 1/89 | 1.1 | 0.1–6.1 |
| Osteophytes | 64/89 | 71.9 | 62.0–81.8 |
| Subchondral sclerosis | 59/89 | 66.3 | 55.9–76.7 |
| Geodes or subchondral cysts | 21/89 | 23.6 | 14.2–33.0 |
| Joint space narrowing | 72/89 | 80.9 | 72.2–89.6 |
| Joint dislocations and/or altered bone alignment | 28/89 | 31.5 | 21.2–41.7 |
| Kellgren-Lawrence scale | |||
| Grade 0 | 1/79 | 1.3 | 0.1–6.8 |
| Grade 1 | 7/79 | 8.9 | 2.0–15.8 |
| Grade 2 | 14/79 | 17.7 | 8.7–26.8 |
| Grade 3 | 41/79 | 51.9 | 40.3–63.5 |
| Grade 4 | 16/79 | 20.3 | 10.7–29.7 |
CI, confidence interval.
Kellgren-Lawrence scale: grade 0: normal; grade 1: possible osteophytes, doubtful joint space narrowing; grade 2: defined osteophytes and possible joint space narrowing; grade 3: moderate osteophytes, joint space narrowing, some subchondral sclerosis, possible joint deformity; grade 4: large osteophytes, severe joint space narrowing, severe subchondral sclerosis and defined joint deformity.
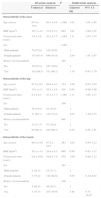
The disease progression took longer for women that met the classification criteria for osteoarthritis of the knee (8.0 vs 9.4 years, P=.010). The family history of osteoarthritis is associated with the disease developing earlier and for a longer period of time. This does not happen in patients with osteoarthritis of the hip or hand (Table 4).
Diagnosis Age and Progression Time of Osteoarthritis in Patients With Osteoarthritis of the Knee, Hip or Hand, According to Diverse Variables.
| Diagnosis age | Progression time (years) | |||||
|---|---|---|---|---|---|---|
| Average±SD | Median | P | Average±SD | Median | P | |
| Osteoarthritis of the knee | ||||||
| Total (n=1060) | 59.1±10.0 | 60 | 9.1±7.3 | 7.5 | ||
| Sex | .403 | .010 | ||||
| Male | 59.6±10.0 | 60 | 8.0±6.6 | 6 | ||
| Female | 59.0±10.0 | 59 | 9.4±7.4 | 8 | ||
| Smoker | .016 | .001 | ||||
| No | 59.3±9.9 | 60 | 9.2±7.3 | 8 | ||
| Yes | 56.2±10.5 | 57 | 6.7±5.9 | 5 | ||
| Family history of osteoarthritis | <.001 | .009 | ||||
| No | 60.8±10.2 | 61.5 | 8.4±7.1 | 6 | ||
| Yes | 58.0±9.7 | 58 | 9.5±7.5 | 8 | ||
| Osteoarthritis of the hip | ||||||
| Total (n=295) | 60.3±10.2 | 60.5 | 8.4±7.0 | 7 | ||
| Sex | .368 | .720 | ||||
| Male | 59.3±11.5 | 61 | 8.5±7.9 | 7 | ||
| Female | 60.6±9.6 | 60 | 8.4±6.6 | 7 | ||
| Smoker | .008 | .304 | ||||
| No | 61.2±9.8 | 62 | 8.2±6.4 | 7 | ||
| Yes | 53.5±9.8 | 50 | 6.9±5.2 | 5 | ||
| Family history of osteoarthritis | .475 | .729 | ||||
| No | 60.9±11.5 | 63 | 8.2±7.3 | 6.5 | ||
| Yes | 59.9±9.5 | 60 | 8.5±7.0 | 7 | ||
| Osteoarthritis of the hands | ||||||
| Total (n=185) | 57.4±9.7 | 57 | 10.4±7.8 | 9 | ||
| Sex | .938 | .456 | ||||
| Male | 57.5±11.4 | 57.5 | 9.2±7.2 | 7 | ||
| Female | 57.4±9.5 | 57 | 10.6±7.9 | 9.5 | ||
| Smoker | .001 | .001 | ||||
| No | 58.0±9.8 | 57 | 9.9±7.6 | 8 | ||
| Yes | 50.8±8.7 | 52 | 5.5±4.9 | 4 | ||
| Family history of osteoarthritis | .425 | .990 | ||||
| No | 58.1±9.9 | 58 | 11.0±8.9 | 10 | ||
| Yes | 56.8±9.6 | 56 | 10.4±7.7 | 8.5 | ||
SD, standard deviation.
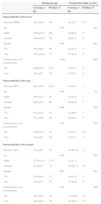
On most patients with osteoarthritis, the disease appears in a bilateral manner, either for osteoarthritis of the knee (76.9%), hip (59.3%) or hand (94.7%). Table 5 shows the differences among patients with osteoarthritis depending on whether the affection is unilateral or bilateral. After adjusting by age, sex, body mass index, progression time of osteoarthritis and history, the variables associated with a bilateral affection of osteoarthritis of the knee are older age (OR=1.03; 95% CI of 1.01–1.05), greater body mass index (OR=1.03; 95% CI of 1.00–1.07) and longer progression time of osteoarthritis (OR=1.11; 95% CI of 1.07–1.15), as well as female sex (OR=2.04; 95% CI of 1.41–2.97). For osteoarthritis of the hip, the variables identified with an independent effect for predicting a bilateral affection are a longer progression time of the disease (OR=1.11; 95% CI of 1.05–1.17) and female sex (OR=2.03; 95% CI of 1.10–3.75). No variables associated with bilateral affection on osteoarthritis of the hands were found (Table 5).
Differences in Patients With Osteoarthritis Regarding Unilateral or Bilateral Affection and Logistic Regression Analysis to Predict Bilateral Affection, According to Location.
| Bivariate analysis | P | Multivariate analysis | |||
|---|---|---|---|---|---|
| Unilateral | Bilateral | Adjusted OR | 95% CI | ||
| Osteoarthritis of the knee | |||||
| Age (years) | 65.9±10.4 | 69.1±8.8 | <.001 | 1.03 | 1.01–1.05 |
| BMI (kg/m2) | 29.7±4.5 | 31.0±5.3 | .003 | 1.03 | 1.00–1.07 |
| Progression time (years) | 5.9±5.6 | 10.1±7.5 | <.001 | 1.11 | 1.07–1.15 |
| Sex | <.001 | – | |||
| Male patients | 76 (32.6) | 129 (16.6) | 1 | ||
| Female patients | 157 (67.4) | 646 (83.4) | 2.04 | 1.41–2.97 | |
| History of osteoarthritis | .189 | – | |||
| No | 78 (35.5) | 227 (30.8) | 1 | ||
| Yes | 142 (64.5) | 511 (69.2) | 1.19 | 0.83–1.70 | |
| Osteoarthritis of the hip | |||||
| Age (years) | 67.8±9.2 | 69.6±9.3 | .114 | 1.00 | 0.97–1.03 |
| BMI (kg/m2) | 30.1±5.1 | 29.5±4.8 | .416 | 0.95 | 0.90–1.00 |
| Progression time (years) | 6.3±6.1 | 10.1±7.3 | <.001 | 1.11 | 1.05–1.17 |
| Sex | .109 | – | |||
| Male patients | 38 (34.9) | 41 (25.8) | 1 | ||
| Female patients | 71 (65.1) | 118 (74.2) | 2.03 | 1.10–3.75 | |
| History of osteoarthritis | .898 | – | |||
| No | 32 (31.7) | 47 (30.9) | 1 | ||
| Yes | 69 (68.3) | 105 (69.1) | 0.54 | 0.45–1.51 | |
| Osteoarthritis of the hands | |||||
| Age (years) | 64.4±9.8 | 67.5±10.0 | .383 | 1.02 | 0.94–1.12 |
| BMI (kg/m2) | 28.3±4.3 | 28.9±4.5 | .680 | 0.98 | 0.82–1.17 |
| Progression time (years) | 9.8±10.0 | 10.6±7.9 | .479 | 1.00 | 0.90–1.12 |
| Sex | .284 | – | |||
| Male patients | 2 (22.2) | 18 (11.1) | 1 | ||
| Female patients | 7 (77.8) | 144 (88.9) | 0.95 | 0.10–8.93 | |
| History of osteoarthritis | .108 | – | |||
| No | 5 (62.5) | 44 (29.1) | 1 | ||
| Yes | 3 (37.5) | 107 (70.9) | 3.48 | 0.71–16.97 | |
CI, confidence interval; BMI, body mass index; OR, odds ratio.
The data shows average±SD or n (%) depending on the case.
As for therapeutic management, we have observed that 58.1% (95% CI of 55.3%–60.8%) of the patients received pharmacological treatment combined with some kind of non-pharmacological treatment. The most common non-pharmacological treatment has been hypocaloric diet (36.6%), together with exercise and kinesitherapy (36.5%). 39.5% (95% CI of 36.8%–42.3%) had only pharmacological treatment and 2.4% (95% CI of 1.6%–3.4%) of the patients did not receive any drug.
The most common pharmacological treatments are paracetamol (70.5%) (95% CI of 67.9%–73.1%) and oral non-steroidal anti-inflammatory drugs (NSAIDs) (67.9%) (95% CI of 65.3%–70.5%) (Table 6). The most common treatment is the combined intake of oral analgesics and oral NSAIDs (18.4%) (95% CI of 16.2%–20.5%), followed by treatment using only oral analgesics (13.2%) (95% CI of 11.3%–15.1%) and treatment using only oral NSAIDs (10.6%) (95% CI of 8.8%–12.3%).
Most Frequently Used Oral and Transdermal Pharmacological Treatments for Patients With Osteoarthritis, Doses Used and Physician Who Prescribed It.
| Prescribing physician | ||||||||
|---|---|---|---|---|---|---|---|---|
| Pharmacological treatment | Frequency | Dose (mg/day) | Family physician (%) | Area and/or hospital specialised physician (%) | Private physician (%) | Self-medication (%) | ||
| No. (%) | Average | SD | Median | |||||
| Oral analgesics | ||||||||
| Paracetamol | 887 (70.5) | 2195.6 | 980.0 | 2000 | 91.1 | 6.3 | 0.7 | 1.9 |
| Oral non-steroidal anti-inflammatory drugs | ||||||||
| Ibuprofen | 349 (27.7) | 1441.2 | 454.4 | 1600 | 88.6 | 8.7 | 1.3 | 1.3 |
| Diclofenac | 230 (18.3) | 125.0 | 36.7 | 150 | 84.5 | 13.0 | 1.0 | 1.5 |
| Aceclofenac | 103 (8.2) | 175.3 | 51.7 | 200 | 76.1 | 21.6 | 2.3 | 0 |
| Meloxicam | 62 (4.9) | 15.7 | 3.0 | 15 | 52.9 | 45.1 | 2.0 | 0 |
| Naproxen | 39 (3.1) | 980.5 | 308.7 | 1050 | 76.7 | 23.3 | 0 | 0 |
| Celecoxib | 36 (2.9) | 208.3 | 37.3 | 200 | 34.6 | 65.4 | 0 | 0 |
| Piroxicam | 34 (2.7) | 23.3 | 7.3 | 20 | 78.6 | 14.3 | 3.6 | 3.6 |
| Ketorolac | 21 (1.7) | 39.4 | 24.6 | 30 | 66.7 | 33.3 | 0 | 0 |
| Dexketoprofen | 18 (1.4) | 50.3 | 20.7 | 50 | 68.8 | 18.8 | 12.5 | 0 |
| Rofecoxib | 14 (1.1) | 23.9 | 3.8 | 25 | 54.5 | 45.5 | 0 | 0 |
| Lornoxicam | 13 (1.0) | 12.9 | 4.1 | 16 | 50.0 | 41.7 | 8.3 | 0 |
| Indomethacin | 11 (0.9) | 111.4 | 40.9 | 100 | 90.0 | 0 | 0 | 10.0 |
| SYSADOAS | ||||||||
| Glucosamine sulphate | 201 (16.0) | 1498.1 | 156.1 | 1500 | 57.8 | 40.6 | 1.7 | 0 |
| Diacerein | 47 (3.7) | 90.8 | 22.8 | 100 | 51.2 | 46.3 | 2.4 | 0 |
| Chondroitin sulphate | 84 (6.7) | 721.0 | 225.8 | 800 | 33.3 | 62.1 | 4.5 | 0 |
| Opioids | ||||||||
| Tramadol | 155 (12.3) | 158.5 | 84.8 | 150 | 77.7 | 20.8 | 1.5 | 0 |
| Codeine | 53 (4.2) | 55.5 | 29.8 | 45 | 89.1 | 8.7 | 0 | 2.2 |
| Transdermal fentanyl (μg/h) | 15 (1.2) | 44.4 | 24.3 | 50 | 38.5 | 61.5 | 0 | 0 |
| Transdermal buprenorphine (μg/h) | 6 (0.5) | 29.3 | 11.5 | 35 | 75.0 | 25.0 | 0 | 0 |
SD, standard deviation.
The average drug dose used is 2195.6±980.0mg/day for paracetamol, 1441.2±454.4mg/day for ibuprofen, 125.0±36.7mg/day for diclofenac and 175.3±51.7mg/day for aceclofenac (Table 6).
Globally, 25% of the patients were treated with SYSADOAS (16.0% glucosamine sulphate, 6.7% chondroitin sulphate and 3.7% diacerein) (Table 6).
The most commonly used drugs are mostly prescribed by the family physician. Among the drugs most frequently prescribed by an area and/or hospital specialised physician, there are celecoxib (65.4%), chondroitin sulphate (62.1%) and transdermal fentanyl (61.5%) (Table 6).
DiscussionWith this study, we intend to describe the characteristics of patients with osteoarthritis and to verify the consistency with results highlighted in other published studies. In this sense, we have found that the most common location of osteoarthritis is distinctly the knee (64.5% of included patients), followed by the knee plus the hip (11.4%) and hip (9.4%). This result is consistent with published studies.10–14
The characteristics of study patients mostly include the risk factors described for the development of osteoarthritis. In this way, we found that it mostly occurs in women (77.8%) regardless of the location of the osteoarthritis, the average age of participants is 68 years and, at the same time, people being overweight and with obesity are usually the target (38.9% and 47.6%, respectively) in study participants. All of these results are consistent with other epidemiologic studies and published revisions.10,12,13,15–18
As with other studies,12,14,17,19–21 we have found that the most common comorbidity is high blood pressure (55.1%). Upon observing the concomitant medication of study participants, we have noted that gastroprotectors (55.3%) and, among them, proton pump inhibitors (45%) are the most commonly prescribed drugs. This may be related to the wide use of NSAIDs in these patients and the need to avoid adverse gastrointestinal effects.
The most commonly used pharmacological treatments in patients of this study are paracetamol (70.5%) and oral NSAIDs (67.9%). Several epidemiologic studies also show that the most commonly used drugs for osteoarthritis are analgesics followed by NSAIDs, which is consistent with the guidelines for the management of osteoarthritis regarding the use of a pharmacological treatment.11,13,14,22 However, there are also other studies that show a greater use of drugs (mostly NSAIDs) which is not in compliance with the guidelines.12,23–26 Hunter et al.27 in the article on the quality of the management of osteoarthritis, outlines that, despite the consistency among recommendations for the management of osteoarthritis, the clinical practice is not in compliance with them, but instead responds to several factors (preferences of the physician and patient, support from the health care service, etc.).
This study clearly shows the underuse of non-pharmacological treatments in an isolated manner (0.3%). The inadequate indication of non-pharmacological measures has been found in other studies.20,25,28 Hypocaloric diet (36.6%) and physical exercise (36.5%) are the most frequent recommendations, and these findings are consistent with other studies.12,14
The used average dose of paracetamol and opioid analgesics is lower than the one established in the recommendations from the World Health Organisation regarding the defined daily dose of drugs,29 while the most commonly prescribed NSAIDs (ibuprofen and diclofenac) are administered at a higher dose, though recommendations on the use of NSAIDs indicate that they ought to be taken at the lowest possible dose during the shortest possible time.
We cannot obtain from the results of this study the therapeutic compliance only be investigating the prescription. In this sense, the Mediterranean Osteoporosis (MEDOS) study,30 conducted in Australia, determined that the therapeutic adherence was related to the side effects of drugs, their cost, mode of action and treatment schedule.
Study LimitationsThis study was conducted with volunteer physicians interested in participating in it and with patients that, during the study period, were identified by those physicians. It is clear that this results in a selection bias that we consider is inevitable to ensure the feasibility of the study, since we cannot conduct these studies if they are without volunteer professionals and patients willing to participate. Patients have been selected in a consecutive manner, as they visited the physicians’ offices during the study period. The consistency of the results of this study in relation to other publications, some of which have been randomly selected, shows that their external validity has not been affected as to result generalisation.
To minimise the bias of information, physicians who participated in the study have been trained on the protocol and information collection. Besides, all the measurement instruments and the questionnaires used are validated (Kellgren–Lawrence radiological scale, ACR clinical and radiological criteria).
A multivariate logistic regression analysis was conducted to control the confusion regarding the bilateral affection of joints.
This study shows that the profile of the patient with osteoarthritis is that of a female patient >65 years, overweight-obese, frequent clinical, comorbidity and moderate radiological affection. Most patients have bilateral affection. In the case of osteoarthritis of the knee, bilateral affection is associated with older female patients, with a greater body mass index and a longer progression time of osteoarthritis. In the case of osteoarthritis of the hip, variables associated with bilateral affection are female sex and progression time. No determinants of bilateral affection were found in osteoarthritis of the hands, given that in most of these patients both hands are affected. Most patients are under pharmacological treatment prescribed by a family physician, and the most commonly used drug is paracetamol. The used dosage of analgesia is lower than the dosage recommended in clinical guidelines.
Ethical ResponsibilitiesProtection of people and animalsAuthors state that no experiments were performed on human beings or animals as part of this investigation.
Confidentiality of dataAuthors declare that they have complied with the site protocols about the publication of patient data.
Right to privacy and informed consentThe authors have obtained the informed consent from the patients and/or subjects referred to in the article. This document is in possession of the corresponding author.
Conflict of InterestsThe authors declare that there were no conflicts of interest when conducting this study.
This study was conducted with the support of the Spanish Society of Family and Community Medicine (Sociedad Española de Medicina de Familia y Comunitaria, SEMFYC) and obtained financing from the pharmaceutical laboratory MSD.
Juana Redondo Sánchez (Andalusia), Rosa Magallón Botaya (Aragon), Salvador Tranche Iparraguirre (Asturias), Anabel Cremades Maestre (Balearic Islands), M. Dolores Marrero Díaz (Canary Islands), Álvaro Pérez Martín (Cantabria), Enrique González Hidalgo (Castilla-La Mancha), José Espinosa Día (Extremadura), José Luis Torres Baile (La Rioja), Alejandro Tejedor Varillas (Madrid), Juan de Dios González Caballero (Murcia), Adolfo Hervás Angulo (Navarre) and José Sanfélix Genovés (Valencian Community).
Please cite this article as: Castaño Carou A, Pita Fernández S, Pértega Díaz S, Grupo de estudio EVALÚA. Perfil clínico, grado de afectación y manejo terapéutico de pacientes con artrosis en atención primaria: estudio multicéntrico nacional EVALÚA. Reumatol Clin. 2015;11:353–360.