Hematogenous spread of Neisseria gonorrhoeae, a sexually transmitted pathogen, results in disseminated gonococcal disease (DGD), also known as arthritis-dermatitis syndrome, due to the development of skin lesions, tenosynovitis, and arthritis. The most frequently affected population is young adults. We describe the case of an adolescent female who acutely developed skin lesions, arthritis, tenosynovitis, and constitutional symptoms. The causal agent was identified by a culture of vaginal secretion and treated with ceftriaxone for 7 days with complete recovery. It is important to differentiate this clinical picture from other types of arthritis developed in adolescence.
La propagación vía hematógena de Neisseria gonorrhoeae, patógeno de transmisión sexual, resulta en una enfermedad gonocócica diseminada (EGD), también conocida como síndrome artritis-dermatitis por el desarrollo de lesiones cutáneas, tenosinovitis y artritis. La población que más frecuentemente se ve afetada es la de adultos jóvenes. Describimos el caso de una adolescente femenino que de forma aguda desarrolló lesiones cutáneas, artritis, tenosinovitis y síntomas constitucionales por EGD. La identificación del agente causal fue por cultivo de secreción vaginal y fue tratada con ceftriaxona intravenosa durante 7 días, con recuperación clínica completa. Es importante diferenciar este cuadro clínico de otros tipos de artritis desarrollados en la adolescencia.
Neisseria gonorrhoeae, gram-negative diplococcus infects mucosal surfaces such as the urethra, pharynx, conjunctiva, rectum and cervix, the latter having an asymptomatic course, causing a delay in diagnosis in women.1 It is mainly, but not exclusively, seen in sexually active young adults.2 The increase in antimicrobial resistance of N. gonorrhoeae observed in the last decade has led to the resurgence of some of its complications, making it important to identify its clinical manifestations early.3
Asymptomatic local infection favours spread through the bloodstream, causing disseminated gonococcal disease (DGD) in between .5% and 3% of patients, manifesting 2 to 3 weeks after the primary infection.1,4 DGD presents skin alterations, asymmetric polyarticular arthritis and tenosynovitis.5
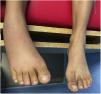
Clinical observationA 14-year-old female patient, previously healthy, presented with fever and arthritis. The beginning of her sexual life had started 9 months previously, without protection, and she had had 2 sexual partners. For 5 days she had been complaining of pain in the right 3rd metacarpophalangeal joint, to which were added the right wrist and ankle, in addition to fever. On admission she showed inability to stand and walk, bilateral arthritis in the wrists and the 2nd to 5th metacarpophalangeal joints. The right ankle and foot were observed with increased volume, hyperaemia and increased local heat, severe pain to touch and to move, which was considered cellulitis (Fig. 1). Gynecological examination: erythematous, oedematous vulva, abundant foamy green, non-fouling leucorrhoea, and mild periorificial cervicitis.
Laboratory studies showed leukocytosis and neutrophilia, C-reactive protein 10.8 mg/dl and erythrocyte sedimentation rate 20 mm/h. General urine examination with Trichomonas spp. Immunological pregnancy test, VDRL, anti-HIV1/HIV2 antibodies, hepatitis B and C negative; Vaginal exudate culture with Neisseria gonorrhoeae, blood culture negative. Soft tissue ultrasound of the right ankle with posterior tibial tenosynovitis and extensor hallucis longus due to soft tissue inflammatory process. It was treated with metronidazole and ceftriaxone for 7 days. During the first days after starting antibiotic therapy, she showed clinical improvement, allowing her to walk, the arthritis of her hands and wrists resolved, and her tenosynovitis improved.
DiscussionWe present a clinical case report representative of DGD, with severe arthritis and tenosynovitis, reporting in the literature its presence in 86% of patients.6 The main message of this case is without a doubt that it reflects the importance of asking questions about sexual activity, the number of sexual partners, and the use of barrier methods since these patients are adolescents with arthritis, tenosynovitis, and constitutional symptoms such as fever and general malaise.7
The clinical presentation of DGD includes arthralgias of one or more joints (knees, wrists, elbows and ankles), accompanied by fever, chills, cervicitis and skin changes.8 The skin condition includes papulo-pustular lesions, vesicles or hemorrhagic bullae, due to the formation of microabscesses with bacterial embolization in the skin.9 Petechiae, purpura, erythema nodosum, cellulitis and vasculitis have also been reported.1 In our patient we described the presence of cellulite as a skin condition.
Endocervical or vaginal culture in women and urethral culture in men are the gold standard for the isolation of N. gonorrhoeae and determination of antimicrobial susceptibility. In DGD we must perform blood cultures and other affected sites to expand the possibilities of isolation.1,10 In this case, the agent was only detected in vaginal secretion.
The 2021 Disease Control Centres recommended treatment includes 1 g. of intramuscular/intravenous ceftriaxone daily or cefotaxime 1 g intravenously every 8 h and switch to an oral regimen based on antimicrobial susceptibility, after 24–48 hours of clinical improvement, for a total of 7 days.3
ConclusionsDGD is an uncommon presentation of gonococcal infection, but it is important to differentiate it from other forms of arthritis in adolescents.
Conflict of interestsThe authors have no conflict of interests to declare.