Intra-articular corticosteroid injections (IACI) are a fundamental part in the treatment of juvenile idiopathic arthritis. The current situation of IACI is reviewed in a population of children.
MethodsWe conducted a narrative review of the literature related to IACI in children, with respect to the injection technique, use of local and general anaesthesia, ultrasound guidance of the procedure, indications, special joints and type of optimal corticosteroid.
ResultsIACI are indicated in any subcategory of juvenile idiopathic arthritis, especially in oligoarticular juvenile idiopathic arthritis. The use of local anaesthetic is highly recommended, and in patients younger than 6 years or requiring multiple joint injections, conscious sedation can also be an option. Ultrasound guidance of injections is recommended in expert hands, but not in a generalised way. Triamcinolone hexacetonide is the corticosteroid of choice in large joints, whereas a more soluble corticosteroid is a better alternative in small or superficial joints (betamethasone or methylprednisolone) to avoid subcutaneous atrophy or hypopigmentation, the most frequent adverse effect of IACI.
ConclusionsIACI are performed heterogeneously and scientific evidence is limited in many cases.
Las infiltraciones intraarticulares con corticoides (IAC) son parte fundamental en el tratamiento de la artritis idiopática juvenil. Se realiza una revisión sobre la situación actual de las IAC en población infantil.
MétodosRevisión narrativa de la literatura de las IAC en población infantil, relacionada con la técnica de infiltración, el uso de anestesia local y general, la guía ecográfica, las indicaciones, las articulaciones especiales y el tipo de corticoide.
ResultadosLas IAC están indicadas en cualquier subcategoría de artritis idiopática juvenil y especialmente en la forma oligoarticular. El uso de anestésico local es recomendable, y en pacientes menores de 6 años o que requieran infiltración múltiple, también la sedación consciente. La infiltración guiada por ecografía es recomendable en manos expertas, pero no de forma generalizada. El hexacetónido de triamcinolona es el corticoide de elección en articulaciones grandes, mientras corticoides más solubles (betametasona o metilprednisolona) serían la alternativa ideal en articulaciones pequeñas o superficiales para evitar la atrofia subcutánea o la hipopigmentación, los efectos adversos más frecuentes.
ConclusionesLas IAC se realizan de forma heterogénea y la evidencia científica es limitada.
Juvenile idiopathic arthritis (JIA) encompasses all arthritis of unknown origin in individuals under the age of 16 years old which lasts for longer than 6 weeks.1 In all of the sub-categories of JIA local treatment with the intra-articular infiltration of corticoids (IAC) is a part of normal therapeutic management.2 Oligoarticular JIA is the type that affects 4 or fewer joints during the first 6 months of evolution of the disease, and it may sometimes be treated exclusively with IAC.2 Although IAC is performed very frequently in the treatment of JIA, opinions vary widely regarding the use of general or local anaesthetics, the infiltration technique, ultrasound guiding of the procedure or the corticoid that should be used.3,4 The differing ages of the patients and the different locations mean that it would be complicated to standardise the IAC procedure in children. This narrative review of the literature summarises the different aspects of IAC procedures in the treatment of JIA.
Infiltration TechniqueAlthough the infiltration technique has not been completely established, it is governed by the same recommendations that apply in adults, and these are summarised in Table 1. The literature contains a great many single-centre studies which describe their experience in performing IAC,5–9 although there are no guides or recommendations about how to do so. IAC is a situation in which children feel stress and nervousness, so that it is positive to create a relaxed atmosphere before performing the procedure.3 IAC should be performed with exquisite asepsis and in as short a time as possible. It is important to use sterile gloves and clean the puncture area with a topical antiseptic. It is recommended that as much liquid as is possible be extracted from the joint before infiltrating the corticoid. The needle should be cleaned in physiological serum to prevent subcutaneous atrophy.10 As is the case in adults, it is also recommendable to rest the unsupported joint for from 24 to 48h to prevent arthritis secondary to the introduced corticoid, even though this is very rare.10
General Recommendations for the Administration of Intra-articular Infiltrations in the Paediatric Population.
| Recommendation |
|---|
| Infiltrate one or two joints per procedure |
| Reinfiltrate after at least 2–4 weeks, if necessary |
| Do not infiltrate the same joint more than 3–4 times per year |
| Painstaking asepsis during the procedure |
| Use a local topical or subcutaneous anaesthetic |
| Use general anaesthesia or conscious sedation when necessary |
| Rest the joint for 24–48h after the procedure |
It is recommendable to use a local anaesthetic in all IAC11 procedures, with lidocaine that is either in an ointment (Emla®) or subcutaneous, chlorethyl in a spray or iontophoresis with lidocaine, depending on what is available. There is more evidence for the use of local anaesthetics or conscious sedation than is the case for other aspects of IAC.11–16 Uziel et al. compared the efficacy of a previous application of Emla® in reducing the pain reported by children with JIA during knee IAC.12 This double-blind randomised clinical trial showed no significant differences between the patients who used Emla® and those who did not, although Emla® is in very widespread use as a local anaesthetic.11 It is recommended that it be applied 60min prior to the procedure using an occlusive dressing, giving rise to anaesthesia in the top 3–5mm of the skin.11 Nevertheless, in clinical practice it is sometimes hard to comply with the minimum time during which Emla® ointment should be applied. Lidocaine iontophoresis produces anaesthesia in somewhat more than the top 8mm of the skin following a 20min10 application. However, this technique is not available in the majority of hospitals. It is probable that restriction of the effect of Emla® to the superficial level of the skin is the reason for the lack of differences in pain during IAC found by Uziel et al. in their clinical trial.12
The use of local anaesthetics is widely accepted in paediatric rheumatology,13 and a combination of a topical local anaesthetic with subcutaneous lidocaine may be beneficial in certain patients.14 Weiss et al. undertook an observational study comparing the use of a local anaesthetic (Emla® or lidocaine iontophoresis) with subcutaneous lidocoaine.14 They compared pain at 3 moments in the procedure: prior to the application of the local anaesthetic, after its application and just before the infiltration, and lastly after the IAC. They found no differences in reported pain between patients who had received subcutaneous lidocaine as well as a local anaesthetic and those who had only receive a local anaesthetic. The exception to this was post-IAC pain in girls, which was less when the methods of local anaesthesia were combined.14
Respecting general anaesthesia or conscious sedation, although some authors propose that this should be obligatory in all procedures,15 it is accepted more widely in specific situations.13 The situations in which it is recommended that some type of conscious sedation (nitrous oxide, propofol, midazolam or fentanil11) be used are: patients under the age of 6 years old, when there is a need to infiltrate 3 or more joints, or in complicated or small locations (the coxofemoral joint or subastragalus, for example).13 On the other hand, when parents and children were asked about their preference in the use of sedation, their opinions differed significantly.16 While the younger children preferred sedation, the parents preferred to avoid the risks this involves. Nevertheless, when the children are older or have had the disease for longer, a higher proportion of them prefer to avoid sedation.16
Ultrasound Scan GuidanceUltrasound scan is an ideal imaging technique for evaluating the paediatric population, and it makes it possible to guide the needle during IAC.7–9 Ultrasound scan guidance in IAC has been proven to be more precise and effective in adults.17 However, in the paediatric population there is no enough scientific evidence to recommend the use of ultrasound scan guidance in all IAC procedures.7–9,18–22 There are many description of its use in different hospitals, but they do not compare the efficacy of procedures carried out with or without ultrasound scan guidance.20–22 In small or complicated joints such as the hip, due to its depth and the proximity to the vascular-nerve bundle, it is recommended that ultrasound scan guidance be used by an expert.18 The exception to this recommendation is at the level of the temporomandibular joint (TMJ).19 Resnick et al. compared the improvement in pain management and mouth opening between patients who had received IAC of the TMJ with and without ultrasound scan guidance. They found that the only difference between both groups was the time taken by the procedure, which lasted for 49min longer in the group with ultrasound scan guidance.19
IndicationsAll patients with JIA are treatable using IAC or peritendinous AC as a single or complementary procedure.2 The oligo-articular form may enter remission after one or several infiltrations. A recent systematic review found that IAC have a beneficial effect.20
The use of systemic treatment with methotrexate in oligo-articular JIA is controversial, and it is not commenced in a routine way, especially in patients with monoarthritis.23 Recently the open, longitudinal and multicentre study by Ravelli et al. has shown that adding methotrexate to the treatment of patients with oligo-articular JIA after IAC of 2 or more joints may slightly increase the effect of infiltrations.24 Nevertheless, the question of whether or not children with oligo-articular JIA benefit from starting treatment with methotrexate has yet to be answered.24
Dysmetria is one of the most common complications that we may find in patients with JIA, especially those with the oligo-articular form and asymmetric synovitis. The hyperaemia that produces the inflammation leads to greater growth of the affected limb and this in turn causes a biomechanical problem that may give rise to complications in adult age. IAC prevent or reduces the severity of joint discrepancy.25 A classic study of 1999 which compared patients with JIA monitored in a hospital where IAC was performed as part of knee synovitis treatment with patients in another hospital where IAC was not used, showed that joint discrepancy was significantly greater in the second group of patients.25
Infiltration of Multiple JointsAlthough there is no limit to the number of joints that may require infiltration, a systemic effect is inevitable when many joints are infiltrated.10 The efficacy of multiple infiltrations (3 or more joints per procedure) has been evaluated in descriptive single-centre studies.26,27 In 2013, Papadopoulou et al. published a retrospective observational study in which joint remission following multiple IAC was observed in one third of the patients included, with an average follow-up of 11 months, as opposed to the two thirds of patients who had a new joint relapse following the IAC in an average time of 6 months.27 These results are not very favourable regarding the routine performance of multiple IAC.27 On the other hand, the efficacy of multiple infiltrations has not been compared with the use of short cycles of systemic corticoids, and it could be asked whether both strategies have a similar level of efficacy, thereby preventing an invasive procedure such as multiple infiltrations.
These multiple procedures require general anaesthesia or at least conscious sedation, and they require a longer session duration, so they are not recommended as routine practice. In the authors’ opinion the maximum recommendable number of IAC per session is 3 joints.
Temporomandibular JointsTMJ are often affected by JIA and they must be examined in all patients, regardless of subcategory. IAC of the TMJ is a relative frequent procedure that improve pain and mouth opening.19,28–30 The improvement is greater in those patients with a shorter time of evolution of their arthritis.29 In patients with morphological alterations and a longer time of evolution, hardly any functional improvement occurs and pain relief is temporary.30 The most common adverse effect of IAC in this location is subcutaneous atrophy, as this is a superficial joint. It is recommended as a complementary treatment, and, as was pointed out above, although ultrasound guidance does not increase its efficacy, it does mean that a longer time is necessary for the procedure.19
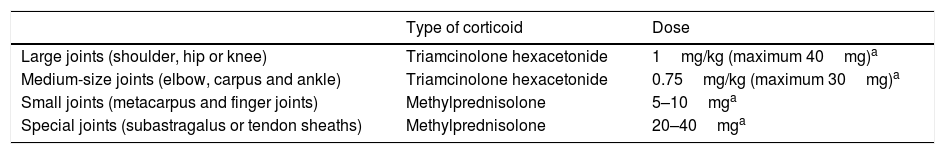
Type of CorticoidThe type of corticoid to be administered depends on the size of the joint: Table 2 shows the recommended dose and corticoid for each joint. It is here that the scientific evidence is the most solid, and where recommendations are the most widely accepted. IAC has longer-lasting efficacy when triamcinolone hexacetonide is used rather than more soluble corticoids such as betametasone.31 The former also undergoes less systemic diffusion and it causes less alteration of cortisol and glucose levels.32 Respecting triamcinolone, hexacetonide has been shown to be more powerful than acetonide in longitudinal studies as well as in retrospective ones.32–35 On the other hand, in spite of the fact that hexacetonide has been proven to have twice the anti-inflammatory effect than acetonide, the use of a double dose of triamcinolone acetonide does not give a greater benefit than the usual dose of triamcinolone hexacetonide.33 The study by Zulian et al. included patients with JIA and symmetrical synovitis (the majority in the knees); one joint was infiltrated with the standard dose of hexacetonide and the other one received an infiltration of the double dose of acetonide. A higher proportion of the joints infiltrated with hexacetonide went into remission, and they did so for a longer time.33 Adverse effects, chiefly subcutaneous atrophy and hypopigmentation, are more frequent with depot corticoids, so that these are not recommended for small or superficial joints, where it is more suitable to use soluble corticoids (betamethasone or methylprednisolone).
Type of Corticoid and Recommended Dose for Each Joint.
| Type of corticoid | Dose | |
|---|---|---|
| Large joints (shoulder, hip or knee) | Triamcinolone hexacetonide | 1mg/kg (maximum 40mg)a |
| Medium-size joints (elbow, carpus and ankle) | Triamcinolone hexacetonide | 0.75mg/kg (maximum 30mg)a |
| Small joints (metacarpus and finger joints) | Methylprednisolone | 5–10mga |
| Special joints (subastragalus or tendon sheaths) | Methylprednisolone | 20–40mga |
IAC are very common procedures in the treatment of JIA, especially in the oligo-articular subcategory, together with systemic treatment or alone. It is highly recommendable to use local anaesthesia before or during the procedure, and to evaluate using conscious sedation in specific situations. Although ultrasound guidance is not recommended as a routine, it may be useful in expert hands to prevent complications in the procedure. In general, large joints benefit more from the administration of triamcinolone hexacetonide, while more soluble corticoids (betamethasone or methylprednisolone)are preferable for small or superficial joints.
Conflict of InterestsThe authors have no conflict of interests to declare.
Please cite this article as: Nieto-González JC, Monteagudo I. Estado actual del tratamiento con infiltraciones intraarticulares en la artritis idiopática juvenil. Reumatol Clin. 2019;15:69–72.