Kaposi's sarcoma (KS) is a malignant vascular tumor widely known as a complication of acquired immunodeficiency syndrome (AIDS) but also related to immunosuppression in renal transplants, and less frequently, to other diseases. We describe a case of KS in a patient affected by antisynthetase syndrome treated with steroids.
El sarcoma de Kaposi (SK) es un tumor vascular maligno conocido fundamentalmente por ser una complicación del síndrome de inmunodeficiencia adquirida (sida), pero también asociado a inmunosupresión en trasplantados renales y, menos frecuentemente, en otras enfermedades. Se presenta un caso de SK en un paciente diagnosticado de síndrome antisintetasa en tratamiento con corticoides.
KS is a malignant vascular tumor not only known primarily for being a complication of acquired immunodeficiency syndrome (AIDS), but also associated with immunosuppression in renal transplant recipients. Less commonly, KS develops in patients with other diseases after long cycles of immunosuppressive therapy. Due to its uniqueness, we present a case of KS in a patient diagnosed with antisynthetase syndrome treated with chronic steroids and a review of the published literature to date.
Clinical PresentationThe patient, a 67-year-old male, had no history of allergies, was an ex-smoker (17 years, 30 cigarettes/day), moderate former alcohol drinker and had chronic obstructive pulmonary disease (emphysema) under bronchodilator therapy as well as presented palmar keratoderma without data of psoriatic arthropathy.
In January 2007, the patient presented pain in both shoulders and the cervical spine without pelvic girdle pain or loss of strength, accompanied by weight loss of 8kg and occasional fever unquantified. He denied anorexia, GI disturbances, worsening of respiratory symptoms or other associated symptoms. Physical examination was normal except for pain upon mobilizing both shoulders, with decreased range of motion, suggestive of bilateral supraspinatus tendinitis. The patient had no strength loss at any level and had a dubious swelling of the distal and proximal interphalangeal joints of the hands. He also had nail lesions suggestive of onychodystrophy.
His laboratory tests showed CBC and coagulation within normal limits. There was only minimal elevation of aspartate aminotransferase and alanine aminotransferase (50U/l and 61U/1, respectively), creatine kinase (CK) of 478U/L, lactate dehydrogenase of 736U/1. Protein, immunoglobulins, C-reactive protein, rheumatoid factor, complement, antinuclear antibodies, antimitochondrial antibodies, smooth muscle and antigastric parietal cell antibodies, alpha-1 antitrypsin deficiency, and thyroid stimulating hormone were negative or were within normal limits, except positivity for Jo-1 antibody. He had an elevated CA 15.3 93.1U/ml, with normal values for the remaining tumor markers performed (alpha-fetoprotein, carcinoembryonic antigen, CA125, CA 19.9, and PSA). Serology for hepatitis viruses B and C and syphilis, human immunodeficiency virus (HIV), Brucella and cytomegalovirus were negative. Chest X-ray showed aortic elongation and images compatible with bronchiectasis in the middle lobe and lingula and both lower lobes. A computed tomography (CT) of the abdomen showed no abnormalities. A CT scan of the chest, abdomen, and pelvis showed radiographic evidence of emphysema and retrocaval lymphadenopathy in the limit of radiological significance and of subcarinal location, without other significant findings. An electromyogram showed a moderate increase in deltoid and biceps poliphasia as a nonspecific finding, without fibrillation potentials and normal amplitude of motor unit potentials. A muscle biopsy showed variability in the size of muscle fibers, interstitial inflammatory infiltrates of T and B lymphocytes and expression of major histocompatibility complex class I antigens on the muscle fibers and type II fiber atrophy, all compatible with inflammatory myopathy.
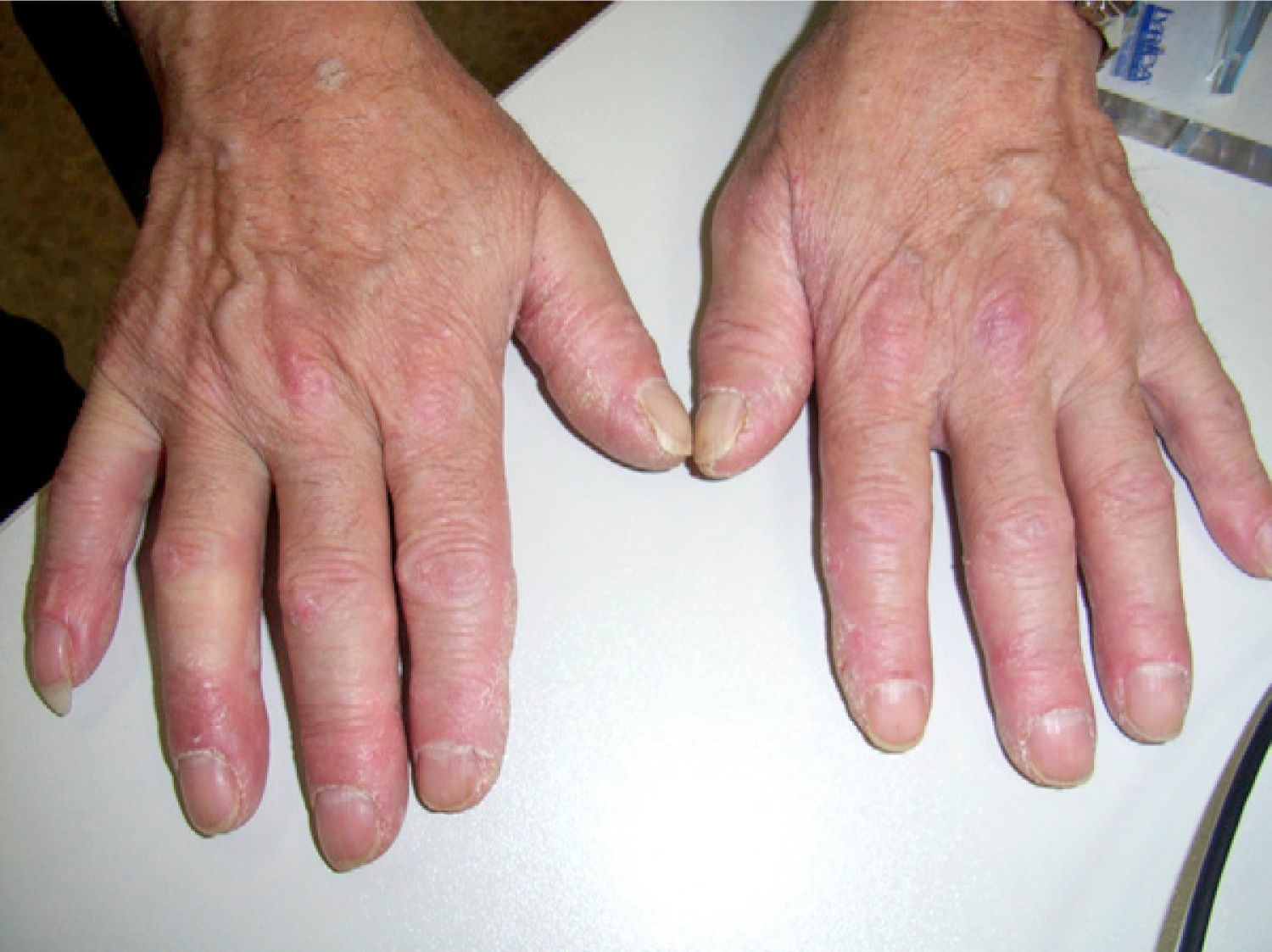
In the presence of a muscle biopsy compatible with polymyositis (PM), increased transaminases and CK and positivity of anti Jo1, the patient was diagnosed with antisynthetase syndrome, treated with prednisone at an initial dose of 30mg/day, which was decreased gradually to a maintenance dose of 7.5mg/day. Two months after the initiation of steroid therapy, the patient presented hyperkeratotic lesions and fissures in the lateral and volar sides of the fingers, compatible with “mechanic's hands” a feature of antisynthetase syndrome (Fig. 1).
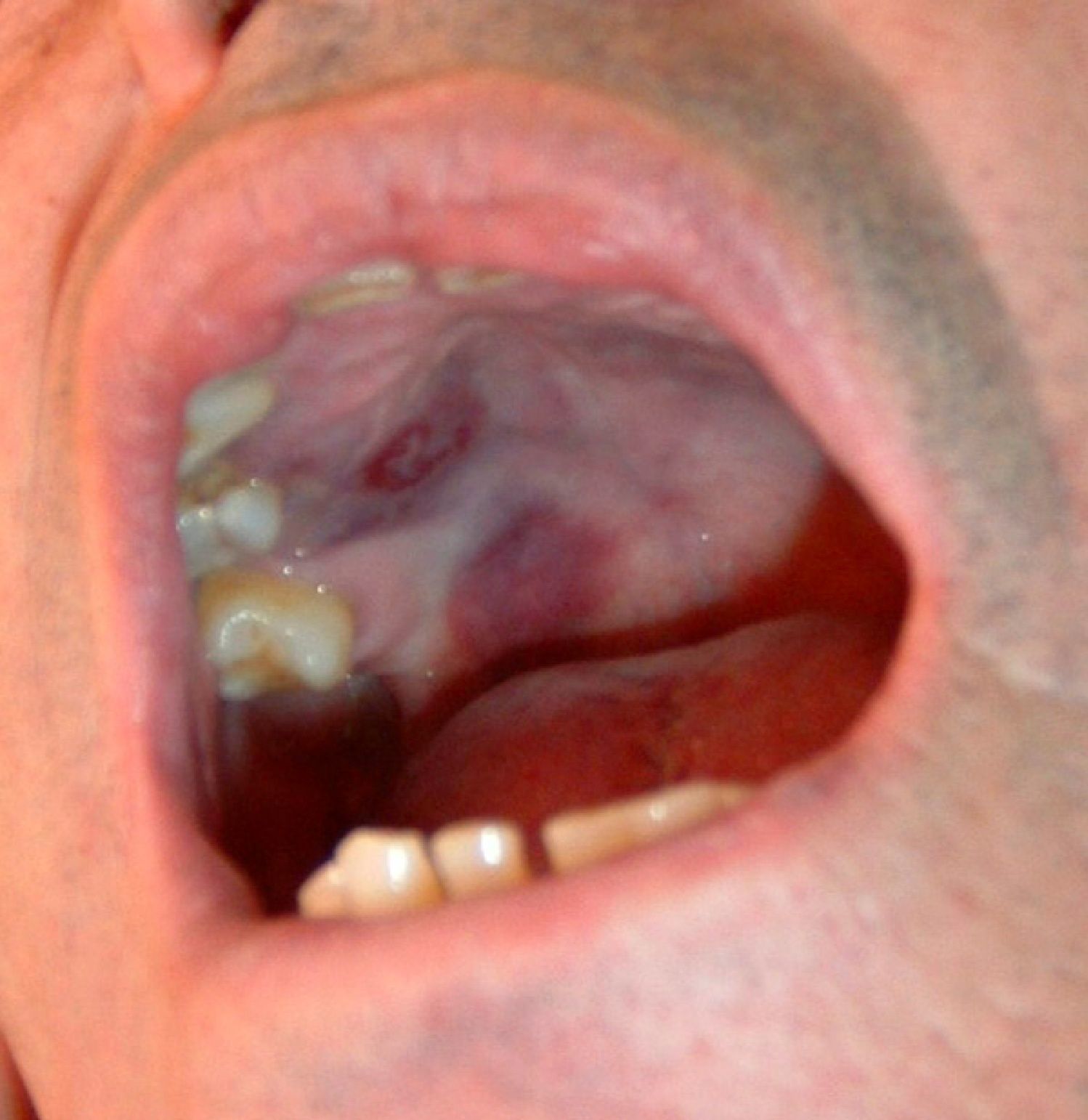
Fifteen months after the diagnosis, there was the appearance of purpuric lesions on the soft palate and on the back of his left foot, which was biopsied. The pathological examination was consistent with KS (Fig. 2) and immunohistochemical study was positive for human herpes virus 8 (HHV-8). Further studies ruled out visceral involvement. A repeat HIV serology was negative. In March 2009, the patient was treated with chemotherapy (doxorubicin), reducing the dose of prednisone and achieving improvement of skin lesions. A CT scan in January 2009 revealed multiple pulmonary nodular lesions that did not appear in previous studies, so an open lung biopsy was performed, finding nonspecific interstitial fibrosis and vascular emphysematous changes in small arterioles. Given the outcome of the lung biopsy and functional impairment of the patient, it was necessary to increase the dose of steroids and we decided to add cyclosporine to the treatment, but these were modified due to the radiographic appearance of pulmonary lesions, although there was clinical and spirometry improvement. Later, in early 2012, the patient had recurrence of KS, with increased skin lesions on the legs, so chemotherapy with betaxolol was administered again. Note that all attempts to reduce steroid treatment below 7.5mg/day have been unsuccessful for worsening respiratory symptoms.
DiscussionKS is a malignant vascular tumor with four clinical varieties: classic, endemic or African, associated with HIV epidemic and iatrogenic. The latter is related to immunosuppressive therapies, mainly affecting not only recipients of solid organs (especially the kidneys), but also patients receiving immunosuppressive treatment due to other conditions, including rheumatic disease, leukemias and lymphomas, inflammatory bowel disease or asthma.1 In the latter group, the risk of KS is 2–4 times lower than in renal transplant at patients and the appearance of the tumor after initiation of immunosuppressive treatment is later in its course (mean of 60 months versus 20 months in transplant patients).2 In any case, it is difficult to discern the importance of the role of immunosuppressive therapy in the development of KS in these patients, as cases have been published of KS associated with autoimmune diseases without prior immunosuppressive therapy1 or related to other treatments (captopril, infliximab, and leflunomide).
Iatrogenic KS has a clinical course similar to classic KS when immunosuppression is not severe, although it is described as more aggressive with visceral involvement in up to 45% of cases compared with 10% in classic KS3,4 There is no clear relationship with ethnicity as in the classic KS2 but, since the incidence of KS is very low relative to the large number of patients on immunosuppressive therapy, we believe that several factors, including this one, play a role in its pathogenesis. In this sense, in the few patients in whom the CD4/CD8 ratio was measured a significant decrease in this ratio could not be verified, although the state of immunosuppression should be a key factor in the pathogenesis.2
HHV-8 has been identified in over 95% of KS lesions associated with all3 clinical subtypes, including iatrogenic KS,4 considered as a necessary but not sufficient factor.5 A recent study has shown that the glucocorticoid receptor is significantly increased in KS tissues, both in the cytoplasm and the nucleus. In addition, corticosteroids have the ability to induce the replication and activation of the lytic cycle of HHV-8. These findings reinforce the theory that HHV-8 is activated in patients treated with corticosteroids.2
There is no clear relationship between the duration or dosage of immunosuppressive therapy and the development of KS, although most patients have received treatment for at least 4 months2 Corticosteroids may act as inducers or as triggers of the disease,6 which would explain why only in the first case KS resolves after discontinuation of treatment.1 In the case of PM and dermatomyositis (DM), it would be necessary to assess whether KS precedes the disease, triggering a paraneoplastic syndrome or is secondary to immunosuppressive therapy.6
In iatrogenic KS prognosis is variable, with an approximately 50% remission rate after the reduction or withdrawal of immunosuppressive therapy.1 In other cases with severe disease or visceral involvement, the use of radiotherapy and/or chemotherapy is required.
Following the literature review we found 36 cases of KS in patients with rheumatic diseases: 10 with rheumatoid arthritis (2 with associated PM), 7 with PM/DM, 6 with temporal arteritis, 4 with lupus erythematosus, 2 with polymyalgia rheumatica, 2 with Wegener, 2 with Behçet, 1 with psoriatic arthritis, 1 with allergic arteritis and 1 with undifferentiated connective disease, ours being the eighth reported case of KS in PM/DM since 1982.2,6–8
ConclusionsIn conclusion, we describe a new case of iatrogenic KS in a patient undergoing chronic steroid therapy for a rheumatic disease. Although the incidence is still low compared with the number of patients who are receiving immunosuppressive therapy, it is important to remember that it is a high risk population for developing KS. Maintaining a high degree of clinical suspicion facilitates the diagnosis of skin lesions, which could be confused initially with cutaneous vasculitis lesions, which can delay treatment and, therefore, worsen the prognosis. We emphasize the need to find a balance between immunosuppressive therapy and chemotherapy in those patients who cannot suspend the former.
Ethical ResponsibilitiesProtection of People and AnimalsThe authors state that no experiments were performed on humans or animals.
Data ConfidentialityThe authors declare that they have followed the protocols of their workplace on the publication of data from patients and all patients included in the study have received sufficient information and gave their written informed consent to participate in this study.
Right to Privacy and Informed ConsentThe authors have obtained informed consent from patients and/or subjects referred to in the article. This document is in the possession of the corresponding author.
Conflict of InterestThe authors declare no conflict of interest.
Please cite this article as: Bragado L, et al. Sarcoma de Kaposi en paciente con síndrome antisintetasa en tratamiento corticoideo. Reumatol Clin. 2013;9:243–5.