The patient was a 64-year-old man with a 35-year history of recurrent nephrolithiasis and progressive development of chronic kidney disease, presently in stage 3. Since he had begun to experience colic, he had had recurrent episodes of monoarthritis in lower limb joints, more marked in the knees, where signs of advanced arthrosis had already appeared. As the findings were suggestive of gouty arthritis, he was treated with colchicine. A few years later, the kidney stones were found to be composed of uric acid and hyperuricemia of approximately 10mg/dL was detected. The patient was recommended to drink abundant liquids and to take potassium citrate, together with dietary measures and allopurinol.
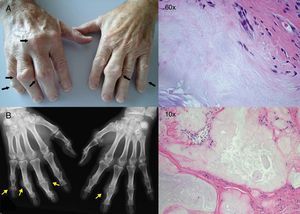
In our examination, we observed hard, painless nodules in proximal interphalangeal joints that, when pressed, showed slight mobility (Fig. 1A; black arrows), independent of the underlying bone, and were radiolucent (Fig. 1B; yellow arrows). The patient could not remember when they had appeared for the first time. The pathological study of a specimen from one of the nodules that caused him discomfort revealed urate deposits among fibrous bridges (10×). At a greater magnification (60×), the remains of uric acid crystals in the form of thin parallel fibers can be discerned.
The patient has a classical syndrome caused by untreated chronic hyperuricemia. It is characterized by the successive development of uric acid stone formation, gouty arthritis, tophi and urate nephropathy (interstitial or secondary to stone formation).1 The tophi in this patient in particular must be distinguished from the Heberden and Bouchard nodes found in other degenerative inflammatory nephropathies.
Hyperuricemia is highly prevalent and is related to other also common disorders, such as hypertension and the metabolic syndrome.2 However, what is not so common is to see such florid clinical manifestations, since detection and treatment take place in increasingly earlier stages of the disease, especially in individuals with comorbidity. This patient, who had no other medical history of interest, was not diagnosed on time and exhibited the natural course of the disease.
Hyperuricemia and its clinical signs generally have an insidious and benign behavior, which responds favorably to treatment. For this reason, early detection and proper treatment are essential in the prevention of progression toward its most serious complication: uric acid nephropathy.
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Author Contributions- 1.
Manuscript conception and design: Fernando Macaya.
- 2.
Data collection: Fernando Macaya, Isaac Díaz.
- 3.
Data analysis and interpretation: Fernando Macaya, Isaac Díaz.
- 4.
Writing, revision and approval of the submitted manuscript: Alejandro Adrover.
The authors declare no conflicts of interest.
Please cite this article as: Macaya F, Adrover A, Díaz I. Nódulos periarticulares, artritis y nefropatía crónica. Reumatol Clin. 2015;11:401–402.