Takayasu arteritis is a vasculitis that affects the aorta, and its large branches, including renal, coronary and pulmonary arteries. This is a case report of a newborn who had early onset sepsis, vascular imaging reported aneurysms in the thoracic and abdominal aorta, with decreased distal pulses, a blood pressure difference >10mmHg and angiographic changes, integrating the diagnose of Takayasu's arteritis.
La arteritis de Takayasu es una vasculitis de grandes vasos, afecta principalmente a la aorta, a sus ramas principales, incluyendo las arterias renales, coronarias y pulmonares. Se reporta un caso de recién nacido hospitalizado desde su nacimiento por proceso séptico, en el cual se encuentran aneurismas a nivel de aorta descendente y abdominal. El paciente cursa con disminución de pulsos distales, predominio en extremidad inferior izquierda, discrepancia mayor a 10mmHg en toma de TA en 4 extremidades, así como cambios angiográficos en aorta integrándose el diagnóstico de arteritis de Takayasu.
Takayasu's arteritis is a large vessel vasculitis that mainly affects the aorta, its major branches and the pulmonary arteries. It may present segmental stenosis, occlusion, dilatation or aneurysm formation during the course of the disease.1 An incidence of 2.6/1000000 cases per year in North America is estimated, however, no information is available on the incidence of TA in the pediatric age.5
All major arteries can be affected, but the vessels most commonly involved are the aorta, subclavian and carotid (60%–90%). It presents various signs and symptoms such as malaise, joint pain, claudication, lightheadedness, heart murmurs, absent or diminished pulses and loss of blood pressure.2
Clinical ObservationThe patient had been hospitalized at birth for suspected trisomy 21, symptomatic hypoglycemia, apnea, intrauterine pneumonia and septic shock. During the hospital stay, a diagnosis of patent ductus arteriosus (PDA) was performed, accompanied by hemodynamic consequences and Enterobacter cloacae bacteremia.
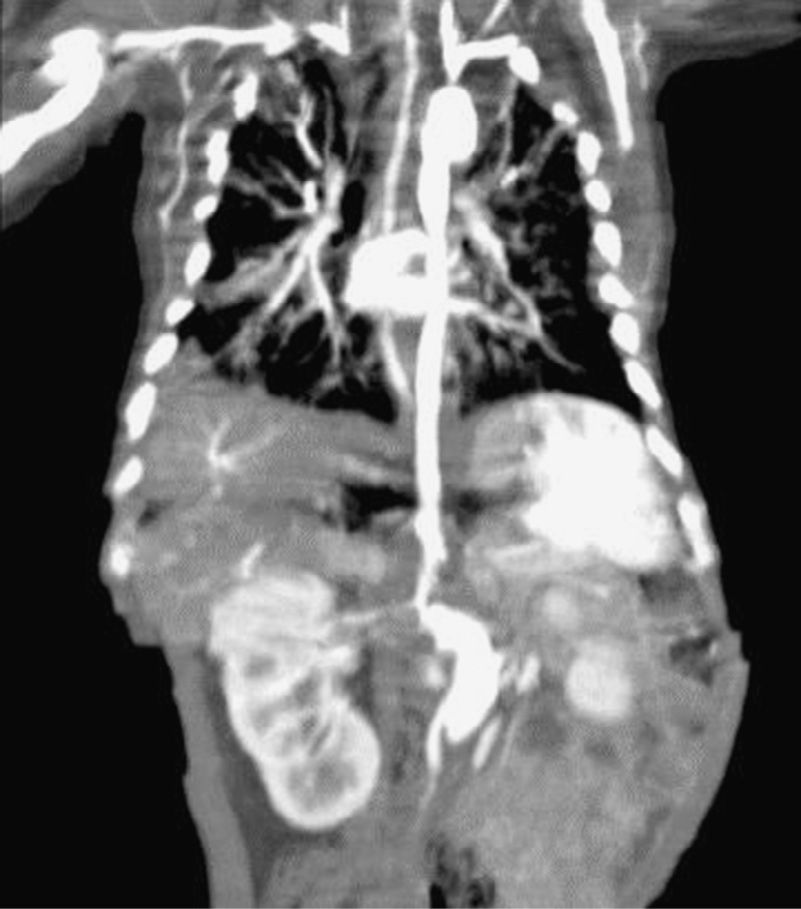
While performing the first echodopplercardiogram, a dilated descending aorta was observed, corroborated by a postsurgical repair of the PDA echocardiography, with an aneurysm of the aortic arch distal to the subclavian artery and the presence of thrombus 4cm×3cm at the mouth of superior vena cava; an angiotomography demonstrated an aortic aneurism, a probable aortic coarctation, plus an abdominal aortic aneurysm (Fig. 1). At diagnosis, the patient had a normal platelet and white blood cell count, anemia, hypocomplementemia at the expense of C3, increased factor VIII and positive PCR.
When approaching the diagnosis, an infectious etiology which may predispose to the inflammatory condition that causes vasculitis is sought; we determined anti-rubella, toxoplasma, CMV, Herpes type 1 and 2 antibodies, Aspergillus fumigatus IgE, IgA Candida albicans, IgG and IgM, Anti Epstein–Barr virus capsid antigen IgG and IgM, Hepatitis B, Hepatitis C and HIV, all of which were negative.
Management began with immunoglobulin 2g/kg/d and prednisone 2mg/kg/day plus anticoagulation with enoxaparin and warfarin for maintenance at 0.3mg/kg/day due to the presence of thrombus in the aforementioned lesion, as well as due to prothrombotic factors and a high cardiovascular risk; no treatment with cyclophosphamide was initiated because of the patient's age and the infection at the time of diagnosis.
We do not know how the patient evolved as the patient was transferred to another hospital for administrative reasons.
DiscussionTA represents 1.5% of vasculitis in childhood; 2% of cases are diagnosed before 10 years of age. The course is variable, depending on the degree of activity, time of diagnosis, presentation and associated symptoms and the effect on other organs. It may have multiple relapses despite treatment. The inflammatory process causes thrombosis in the affected arteries, gradual emergence of stenosis, dilation and aneurysms.7
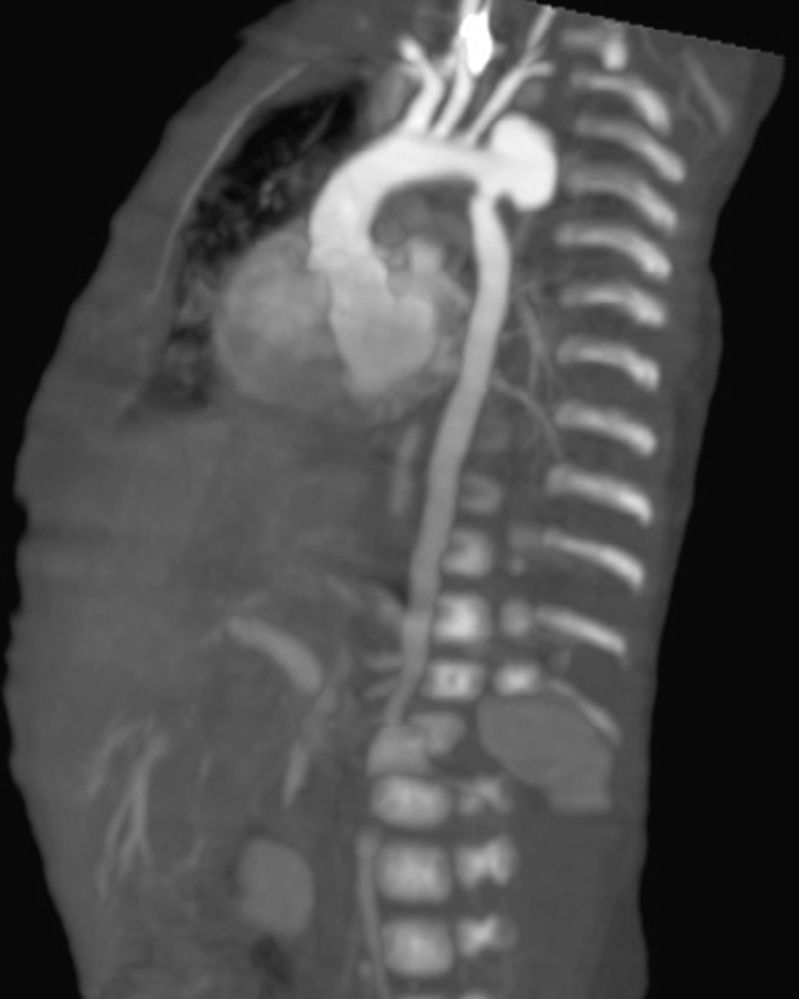
When control echocardiograms were performed for the underlying cardiac disease, aortic dilatation was noted, being more evident in the 3rd week of life; because of this finding, we opted to confirm it through a CT angiography (Fig. 2)
The criteria for classification of AT were established by the American College of Rheumatology (ACR) in 1990, having over 90% sensitivity and specificity. The lack of a control group with atherosclerotic aortic or congenital disease may limit its usefulness, especially in the pediatric age.3
The patient presented decreased distal pulses, predominantly in the left lower limb, with a difference greater than 10mmHg in the BP on the 4 limbs and angiographic changes in the aorta. The diagnosis of Takayasu's arteritis is integrated, according to the ACR, when 4 criteria are present, representing a sensitivity of 90.5% and specificity of 97.8%.4 According to the radiological classification proposed in 1994 by the ACR the patient had thoracic and abdominal artery lesions, type III according to the classification.5 According to the criteria for vasculitis in childhood proposed in 2005 by Ozen et al.,6 which include angiographic changes (CT or conventional MRI) of the aorta or its major branches as a major criterion, and at least one of the following criteria: diminished peripheral arterial pulses and/or limb claudication, difference in BP>10mmHg, dilation of aorta or its major branches and hypertension, with one major criterion and 3 minor ones making the diagnosis according with this classification.
ConclusionsWhile TA is not a common disease in the pediatric age, it should be taken into account in patients with diminished pulses, regardless of their status. Although in TA there is no direct relationship with the ongoing infectious process, the inflammatory pattern may predispose the patient, and the previously described histopathological finding of inflammation composed of plasma cells, lymphocytes and eosinophils in early stages of the disease has been identified.8 Early diagnosis of this vasculitis, and the early onset of immunosuppressive therapy is critical to avoid complications.8 The creation of criteria including pediatric and neonatal populations should be considered.
Ethical ResponsibilitiesProtection of people and animalsThe authors declare this research did not perform experiments on humans or animals.
Data confidentialityThe authors declare that they have followed the protocols of their workplace regarding the publication of patient data.
Right to privacy and informed consentThe authors have obtained the informed consent of patients and/or subjects referred to in the article. This document is in the possession of the corresponding author.
Conflict of InterestThe authors declare no conflict of interest.
Please cite this article as: Vega-Cornejo G, Meza-Beltrán J. Arteritis de Takayasu en el recién nacido, un diagnóstico que sospechar. Reumatol Clin. 2015;11:174–176.