The role of growth factors (GFs) in arthritis is rarely investigated, reporting controversial results.1–4
To the best of our knowledge, the serum levels of IGF-1, FGF-1, TGFβ in patients (pts) with undifferentiated spondyloarthritis (SpA) or psoriatic arthritis (PsA) have never been described in literature. Partsch et al. described a higher titer of GH in the sera of PsA pts compared to psoriatic pts.1
We describe a study designed to evaluate the serum levels of GFs, IGF-1, FGF-1, GH and TGFβ, in PsA pts and SpA pts, with particular focus on the entheseal involvement. Our goal was to assess any differences in the concentration of these GFs between pts with different clinical and instrumental features.
Preliminary data were obtained on 15 pts (all female): 6 with a new diagnosis of PsA,5 9 with a new diagnosis of SpA.6 The control group was formed by 5 age-matched healthy females (HC). The exclusion criteria were intestinal bowel disease, diabetes mellitus, body mass index >30, systemic hypertension, dyslipidemia, alteration of thyroid function.
Serum levels of IGF-1, FGF-1, GH and TGFβ were measured using enzyme-linked immunosorbent assay (ELISA). Moreover, an imaging evaluation was conducted on all pts: the presence of calcific enthesopathy (CE) was assessed using standard radiology; the ultrasound evaluation was conducted according to the Madrid Sonographic Enthesis Index (MASEI) score.7 Disease activity was assessed by means of Disease Activity Score (DAS28), Disease Activity in PSoriatic Arthritis (DAPSA) and Leeds Enthesitis Index (LEI). Comparisons between groups were made with one-way analysis of variance (ANOVA) (Table 1).
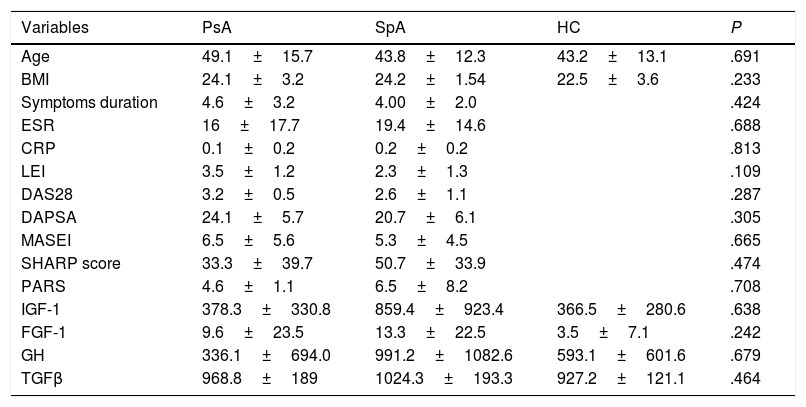
Comparison of demographic, clinical characteristics and serum levels of growth factors between groups in study.
| Variables | PsA | SpA | HC | P |
|---|---|---|---|---|
| Age | 49.1±15.7 | 43.8±12.3 | 43.2±13.1 | .691 |
| BMI | 24.1±3.2 | 24.2±1.54 | 22.5±3.6 | .233 |
| Symptoms duration | 4.6±3.2 | 4.00±2.0 | .424 | |
| ESR | 16±17.7 | 19.4±14.6 | .688 | |
| CRP | 0.1±0.2 | 0.2±0.2 | .813 | |
| LEI | 3.5±1.2 | 2.3±1.3 | .109 | |
| DAS28 | 3.2±0.5 | 2.6±1.1 | .287 | |
| DAPSA | 24.1±5.7 | 20.7±6.1 | .305 | |
| MASEI | 6.5±5.6 | 5.3±4.5 | .665 | |
| SHARP score | 33.3±39.7 | 50.7±33.9 | .474 | |
| PARS | 4.6±1.1 | 6.5±8.2 | .708 | |
| IGF-1 | 378.3±330.8 | 859.4±923.4 | 366.5±280.6 | .638 |
| FGF-1 | 9.6±23.5 | 13.3±22.5 | 3.5±7.1 | .242 |
| GH | 336.1±694.0 | 991.2±1082.6 | 593.1±601.6 | .679 |
| TGFβ | 968.8±189 | 1024.3±193.3 | 927.2±121.1 | .464 |
Data are expressed as mean±standard deviation; significant P value was set to ≤ .05.
BMI: BODY MASS INdex; CRP: C Reactive Protein; DAPSA: Disease Activity in PSoriatic Arthritis; DAS28: Disease Activity Score; ESR: Erythrocytes Sedimentation Rate; HC: Healthy Controls; LEI: Leeds Enthesitis Index; MASEI: MAdrid Sonographic Enthesitis Index; PARS: Psoriatic Arthritis Ratingen Score; PsA: Psoriatic Arthritis; SpA: undifferentiated Spondyloarthritis.
We found that serum levels of IGF-1 and TGFβ were remarkably but not significantly higher in SpA pts compared to PsA pts and HC. In particular, there was a tendency toward higher serum concentrations of TGFβ in pts with CE compared to those pts without and HC (1003.5±208.5 vs. 999.5±156.9 vs. 975.9±61.7; P=.965). Furthermore, a statistically significant negative correlation between TGFβ levels and symptoms duration both in SpA and PsA pts was observed (r2=0.582; P=.029). In addition, subjects with moderate (MA) or high disease activity (HA) according to DAPSA score showed a tendency toward higher GH (low activity (LA): 310.8±449.4, MA: 533.8±967.4, HA: 630±1074.4; P=.903) and IGF-1 (LA: 389.4±532.8, MA: 467.7±825.2, HA: 491.7±585.6; P=.908) levels, while TGFβ levels were higher only in DAPSA HA (LA: 954.6±257.3, MA: 910.1±170.5, HA: 1049.5±44.1; P=.653). Interestingly, this tendency was not observed when assessing the disease activity using the DAS28 score, except for the HA group (LA: 954.6±257.3, MA: 903.8±207.7, HA: 974.5±124.2; P=.91).
The differences we found were not statistically significant most presumably given the small sample size. Since no statistically significant differences in age and BMI were observed between the groups, a difference in the GFs concentration due to physiological hormonal variations can be excluded.8,9
The evidences about DAS28 may be owed to the focus of this score on joint involvement, while enthesitis is not evaluated, as in DAPSA.
The most remarkable result is the significant higher TGFβ serum levels in pts with shorter symptoms duration, suggestive for a potential role of TGFβ as an early biomarker of disease.
This preliminary study, although lacking statistically significant results, support the hypothesis of an important role played by GFs IGF-1, GH and TGFβ rather in the pathogenesis of enthesitis than of joint inflammation. In particular, TGFβ should have a key role in earlier phases of SpA and PsA. Further studies, with a larger sample size, are necessary to clarify the role of GFs in the pathogenesis of enthesopathy, and more broadly of spondylarthritis.
FundingNo funding was received for this study.
Conflict of interestNone.
We would like to thank Prof. Addolorata Corrado and Dr. Giovanni Bellantuono for their contribution in this study.