Cardiac involvement in systemic sclerosis (SSc) is rare but leads to poor short-term prognosis. Evidence regarding heart transplantation (HT) is scarce and is based on experience with isolated cases. We present this case with the aim of analysing the characteristics of a patient with SS who has undergone a successful transplant.
El compromiso cardíaco en la esclerosis sistémica (ES) es raro, pero conlleva un mal pronóstico a corto plazo. La evidencia relativa al trasplante cardíaco (TC) es escasa y se basa en la experiencia con los casos aislados. Presentamos este caso con el objetivo de analizar las características de un paciente con esclerosis sistémica sometido a un trasplante exitoso.
SSc is a systemic autoimmune disease of heterogeneous pathogenesis in which vascular, cutaneous and internal organ fibrosis are prominent.1 Primary symptomatic cardiac involvement occurs in 15–35% of patients and is estimated to cause up to 30% of deaths.1,2
CaseWe present the case of a 58 year-old male diagnosed with anti-SCL70 positive diffuse cutaneous SSc (dcSSc). At diagnosis he presented with myositis, arthralgias and scleroderma (Rodman index 23/51), as well as interstitial disease of subpleural predominance in both lung bases. No oesophageal or renal involvement was observed. After 11 months of evolution it presented elevation of myocardial damage markers (CK, CK-Mb, Troponin and NT-proBNP). Echocardiogram and cardiac resonance showed pericardial effusion, dilation and biventricular systolic dysfunction. The initial affectation was mild (LVEF 51% and RVEF 40% without pathological gadolinium enhancement or myocardial oedema) but despite the support treatment with neurohumoral inhibitors (ACEI, beta-blockers and aldosterone antagonists) and immunosuppressive treatment (corticosteroids, mycophenolate mofetil, cyclophosphamide pulses and Rituximab) it progressed unfavourably to severe affectation (LVEF 26% and RVEF 24% with patchy subendocardial gadolinium enhancement). Interstitial lung involvement was controlled with immunosuppressors, whereas residual myocardial involvement triggered episodes of cardiogenic shock and malignant ventricular arrhythmias. Five months after the diagnosis of cardiomyopathy, HT was chosen as the therapeutic option. Thirty-six months after HT the patient is in stage I of the NYHA, with good biventricular function of the graft, respiratory stable and has presented regression of the skin affectation (Rodman's index of 17/51 at 16 months post-transplant) with the usual immunosuppressive treatment.
DiscussionMyocardial involvement is associated with ventricular systolic dysfunction in 10% of patients3 with a two-year mortality of 60%.4 Although it can occur in both subtypes it is more severe in patients with cdSSc, often evolving in parallel with skin progression.5 It is also more frequently associated with certain antibodies: anti-SCL70, anti-U3 RNP, anti-Ku and anti-Th/To. Due to the importance in terms of mortality of pulmonary involvement, pulmonary and cardio-pulmonary transplantation are accepted options in the face of therapeutic failure. In the case of cardiac affectation there are fewer reported cases of CT, being an option frequently limited by the concomitant affectation of other organs. After a systematic search, another 15 cases of CT were identified in patients with cardiac involvement by ES (Table 1). Eight presented a diagnosis of EScd (53.3%), 5 EScl (33.3%), 1 (6.6%) overlap syndrome with rheumatoid arthritis and in another case the ES subtype was not included. No cardiac recurrence of ES was reported in any case. Only one other published case presented associated pulmonary involvement,6 although its evolution is not assessed since it died 6 weeks after the CT scan due to infectious complications. It is worth noting the skin improvement after immunosuppression for CT, also observed in other published cases.
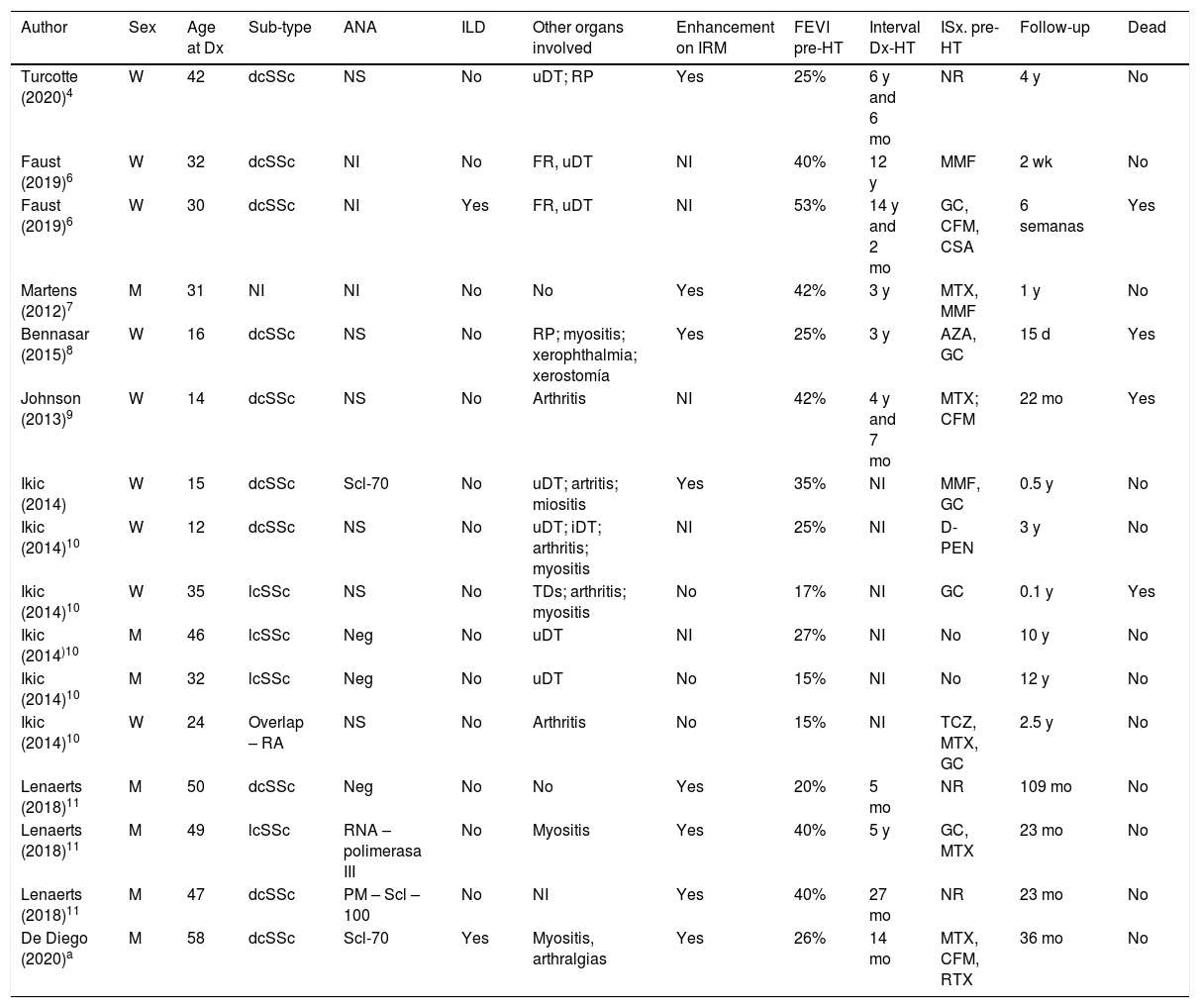
Published cases of heart transplantation in patients with Systemic Sclerosis: demographic, laboratory and clinical characteristics, used immunosuppressive therapies and progression.
| Author | Sex | Age at Dx | Sub-type | ANA | ILD | Other organs involved | Enhancement on IRM | FEVI pre-HT | Interval Dx-HT | ISx. pre-HT | Follow-up | Dead |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Turcotte (2020)4 | W | 42 | dcSSc | NS | No | uDT; RP | Yes | 25% | 6 y and 6 mo | NR | 4 y | No |
| Faust (2019)6 | W | 32 | dcSSc | NI | No | FR, uDT | NI | 40% | 12 y | MMF | 2 wk | No |
| Faust (2019)6 | W | 30 | dcSSc | NI | Yes | FR, uDT | NI | 53% | 14 y and 2 mo | GC, CFM, CSA | 6 semanas | Yes |
| Martens (2012)7 | M | 31 | NI | NI | No | No | Yes | 42% | 3 y | MTX, MMF | 1 y | No |
| Bennasar (2015)8 | W | 16 | dcSSc | NS | No | RP; myositis; xerophthalmia; xerostomía | Yes | 25% | 3 y | AZA, GC | 15 d | Yes |
| Johnson (2013)9 | W | 14 | dcSSc | NS | No | Arthritis | NI | 42% | 4 y and 7 mo | MTX; CFM | 22 mo | Yes |
| Ikic (2014) | W | 15 | dcSSc | Scl-70 | No | uDT; artritis; miositis | Yes | 35% | NI | MMF, GC | 0.5 y | No |
| Ikic (2014)10 | W | 12 | dcSSc | NS | No | uDT; iDT; arthritis; myositis | NI | 25% | NI | D-PEN | 3 y | No |
| Ikic (2014)10 | W | 35 | lcSSc | NS | No | TDs; arthritis; myositis | No | 17% | NI | GC | 0.1 y | Yes |
| Ikic (2014)10 | M | 46 | lcSSc | Neg | No | uDT | NI | 27% | NI | No | 10 y | No |
| Ikic (2014)10 | M | 32 | lcSSc | Neg | No | uDT | No | 15% | NI | No | 12 y | No |
| Ikic (2014)10 | W | 24 | Overlap – RA | NS | No | Arthritis | No | 15% | NI | TCZ, MTX, GC | 2.5 y | No |
| Lenaerts (2018)11 | M | 50 | dcSSc | Neg | No | No | Yes | 20% | 5 mo | NR | 109 mo | No |
| Lenaerts (2018)11 | M | 49 | lcSSc | RNA – polimerasa III | No | Myositis | Yes | 40% | 5 y | GC, MTX | 23 mo | No |
| Lenaerts (2018)11 | M | 47 | dcSSc | PM – Scl – 100 | No | NI | Yes | 40% | 27 mo | NR | 23 mo | No |
| De Diego (2020)a | M | 58 | dcSSc | Scl-70 | Yes | Myositis, arthralgias | Yes | 26% | 14 mo | MTX, CFM, RTX | 36 mo | No |
Dx: diagnosis; ANA: anti-nuclear antibody; ILD: interstitial lung disease; Interval Dx-TC: interval between Dx and HT; ISx: immunosuppressant; y: years; mo: months; wk: week; M: man; W: woman; NI: not included; NS: no specificity; uDT: upper digestive tract; iDT: inferior digestive tract; RP: Raynaud's phenomenon; lcSSc: limited cutaneous SSc; cdSSc: cutaneous diffuse SSc; Neg: negative; RA: rheumatoid arthritis; MTX: methotrexate; MMF: mycophenolate mofetil; D-PEN: D-penicillamine; AZA: azathioprine; GC: glucocorticoids; CFM: cyclophosphamide; CSA: cyclosporine A; TCZ: tocilizumab; RTX: rituximab.
Although the literature is limited, the case presented, along with those previously published, demonstrates that HT is a valid therapeutic option in SSc with severe cardiac involvement especially if non-cardiac systemic involvement is ruled out and/or controlled.
Consents and approval of the ethics committeeThe publication of the case was approved by the ethics committee of the Donostia University Hospital. Informed consent was obtained from the patient for the publication of his case.
Conflict of interestThe authors declare that they have no conflicts of interest. Also, all authors read and approved the final manuscript.