We present the case of a 91 year old woman without known chronic diseases. As significant history she had been diagnosed with a lipoma in the right knee extensor region over 60 years ago, but did not provide evidence or reports related to the diagnosis. The patient consulted because the lesion had changed color becoming more violet in recent months, had increased in size and prevented her from kneelling comfortably. Throughout the whole process, the lesion was never painful.
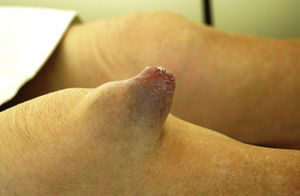
Physical examination revealed a soft consistency tumor of conical shape with a base circumference of 8cm and a height of 6cm located in front of the patellar tendon. The tumor was painless, apparently not dependent of deep tissue and had no local heat. At its distal region thin, purple and scaly skin could be seen (Fig. 1).
The mobility of the knee joint was not compromised and the tumor did not move during the performance of knee flexor movement. The remaining physical examination was not relevant.
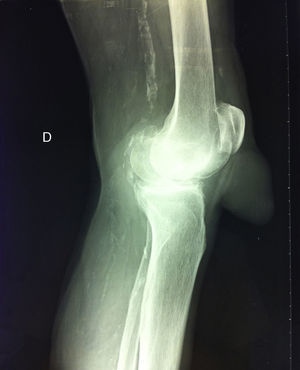
During radiological examination of the knee we observed that the tumor was of soft tissue in origin, showed no radiopaque images inside and respected the integrity of the patellar tendon. Other findings highlighted a degree of osteoarthritis and the presence of radiological signs of atheromatosis (Fig. 2).
Ultrasound examination of the lesion showed heteroechoic content that moved under pressure exerted by the probe or by the examiner. Studying the patellar tendon from the lateral approach demonstrated their integrity and no relation to the tumor.
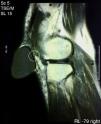
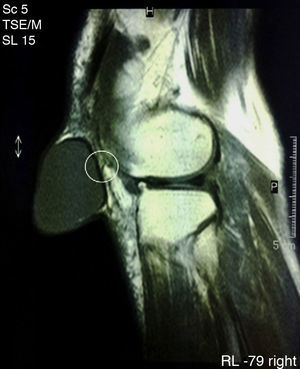
Finally, we performed magnetic resonance imaging (MRI) (Fig. 3) which confirmed the diagnosis of a cystic tumor but was unable to identify any communication with the prepatellar bursa, although it recognized a small non-communicating fold in the rear wall thereof. The anatomy of the rest of the knee was unremarkable except for characteristics associated with the age of the patient.
The patient underwent complete surgical excision of the tumor after needle aspiration of its contents (11 cc of serosanguineous fluid). The volume of fluid obtained and the surgical specimen were sent to pathology. The surgeons reported an extra-articular thin-walled and complete cystic structure of 7cm×7cm×6cm with little adherence to surrounding tissues, located anteriorly to the patellar tendon without making contact with this or with the prepatellar bursa and removed in its entirety. Pathological report indicated that the cystic structure was lined by synovial tissue and the fluid content consisted of synoviocytes, macrophages, red cells and synovial fluid.
After surgery, the patient resumed her usual activities normally.
CommentsThe differential diagnosis of tumors of the knee include lipoma, hemangioma, giant cell tumor of the tendon sheath, synovial cysts, ganglions and nodular localized synovitis.1–3 In general, their progression is benign and may rarely be related to an intra or paraarticular tumor.4
Synovial cysts are usually benign entities located outside the joint capsule but anatomically related to it by means of small channels that can be permeable or obliterated.1,5 In our case, we identified a fold of the posterior wall of the cyst which could be the remnant of a canal structure, now obliterated, that connected the cyst with the joint (Fig. 3). Synovial cysts are caused by mucinous degeneration, trauma or tumors.1 For any of these reasons, a shift of synovial fluid from regions of high to low pressure causing a progressive mobilization of the synovial tissue and its eventual outgrowth outside the capsule.2 Once this phenomenon occurs, the liquid may organize or move freely from the joint to the cyst through a channel with a permeability can be permanent, episodic or short lasting.6 The displacement of fluid in one direction or another conditions an increase or decrease in the size of the cavity.2
Ganglia are cystic formations similar to synovial cysts.6 They differ in that the walls of synovial cysts are coated by synoviocytes, while ganglia are covered by the adjacent tissue itself.1,7 This makes histological testing critical for the final diagnosis. Both structures are considered extra-articular, but may rarely occur inside the knee joint, or paraligamentary1 or intramenisca.l,8,9
Although the technique of choice for the diagnosis of synovial cysts is MRI, histological demonstration is the definitive test and should not be overlooked before definitively ruling out all other possibilities.2
As for treatment, synovial cysts may be treated by aspiration of its content without requiring more than local anesthesia.1,9 The drawback of this technique is that the mechanism that gives rise to the lesion may still be patent and as a result, the cyst can replenish synovial fluid in time.1 Surgical excision is the definitive treatment6 but procedures have been tested including needle aspiration of intracystic content and administration of fibrin-based substances that affect the final sealing of the walls.10
Please cite this article as: Guillén Astete CA, et al. Tumor anterior de rodilla como forma de presentación de un quiste sinovial gigante. Reumatol Clin. 2013;9:69–71.