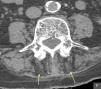
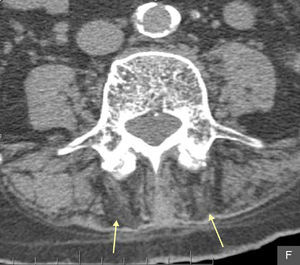
The patient is an 86-year-old male, who performed activities of daily living independently and a history of ischemic heart disease, chronic atrial fibrillation, diabetes mellitus type I and hypothyroidism. He consulted due to back pain and mechanical instability, without previous trauma. It was accompanied by a harmonic progressive kyphosis, reductible when upright and recumbent. The physical examination showed increased anteroposterior curvature of the spine, which conditioned contact of the ribs to the pelvis and was reduced when prone (Fig. 1), with slight flexion of the knees and retroversion of the pelvis. The remaining physical examination was unremarkable. Radiographs were performed and on the lumbar spine (anteroposterior and lateral) showed no significant alterations except for degeneration. With the suspected diagnosis of camptocormia, we requested a CT scan of the lumbar spine which showed selective posterior paravertebral muscle atrophy (Fig. 2), consistent with the initial workup. Analgesic treatment and rehabilitation was started.
Camptocormia or “bent spine syndrome” is an acquired postural impairment, disabling, characterized by flexion of the thoracolumbar spine, pelvis retroversion and flexion of the knees to make the center of gravity stay on the feet. The term derives from the Greek ‘camptos “meaning double and “corms”, which refers to the trunk.1 It was first described by Brodie in 1818, who suggested that the etiology of low back pain and abnormal curvature of the spine had a psychogenic origin. Years later, in 1915, Rosanoff and Souques used the term camptocormia to describe this disease.2
Although the first reported cases suggested a psychogenic etiology, several studies have shown organic causes such as lesions involving the nucleus lenticularis,3 Parkinson's4 disease, dystonia and neuromuscular alterations,5 paraneoplastic syndromes, Graves disease and drugs.6,7 In a retrospective study of 16 patients, it was described in 69% of patients with Parkinson disease, 25% dystonia and one patient with a Gilles de Tourette8 syndrome.
It is a rare disorder with little epidemiological data. Prevalence was 6.9% in an analysis that included 275 patients diagnosed with Parkinson's disease. The development of this condition was related to severe neurological disease.1
The mean age at diagnosis is 65 years. Regarding the clinical features, it is characterized by involuntary flexion of the trunk as a result of progressive weakness of the extensor muscles of the vertebral column. In limited cases, it presents with back pain which is most often asymptomatic. A high percentage of patients had spondyloarthritis, something that suggests that camptocormia may be a risk factor for its development.1,3
The diagnosis is clinical, supported by additional tests such as a CT scan of the lumbar and dorsal column, which typically shows hypodensity and atrophy of the paravertebral muscles and is interpreted as an involution of fat. Given the heterogeneous etiology of this disorder, other examinations such as an electromyogram may be performed; hormonal, bone metabolism and muscle enzymes studies, cranial computed tomography and/or MRI to study basal ganglia may be affected in patients with Parkinson's camptocormia. Patients may also undergo a muscle biopsy.1
Treatment is limited and usually ineffective. It combines rehabilitation and symptomatic pharmacological treatment. In some cases more invasive measures such as surgery has been employed.
A prospective study of 15 patients diagnosed with camptocormia evaluated the effectiveness of orthoses and associated toracopélvica physiotherapy, getting increases in the quality of life in more than 90% of cases.9 IV immunoglobulin has proven effective in cases with inflammatory myopathy. l-Dopa in patients with Parkinson's disease does not usually lead to results. The injection of botulinum toxin in the abdominal and iliopsoas muscle has been effective in some cases reviewed in the literature.1,10
Ethical disclosuresProtection of human and animal subjects. The authors declare that no experiments were performed on humans or animals for this investigation.
Confidentiality of Data. The authors declare that they have followed the protocols of their work centre on the publication of patient data and that all the patients included in the study have received sufficient information and have given their informed consent in writing to participate in that study.
Right to privacy and informed consent. The authors have obtained the informed consent of the patients and /or subjects mentioned in the article. The author for correspondence is in possession of this document.
The authors thank Dr. Ana Carreras, Head of the Emergency Department of the Hospital Germans Trias i Pujol for the images and case.
Please cite this article as: Tejera B, et al. Camptocormia: a propósito de un caso. Reumatol Clin. 2012. http://dx.doi.org/10.1016/j.reuma.2012.05.004.