Proximal humeral osteosynthesis is not without complications (45%1). Infection has a frequency of 0%–4%.2,3 Our objective was to report a case of osteomyelitis, after osteosynthesis and review current treatments.
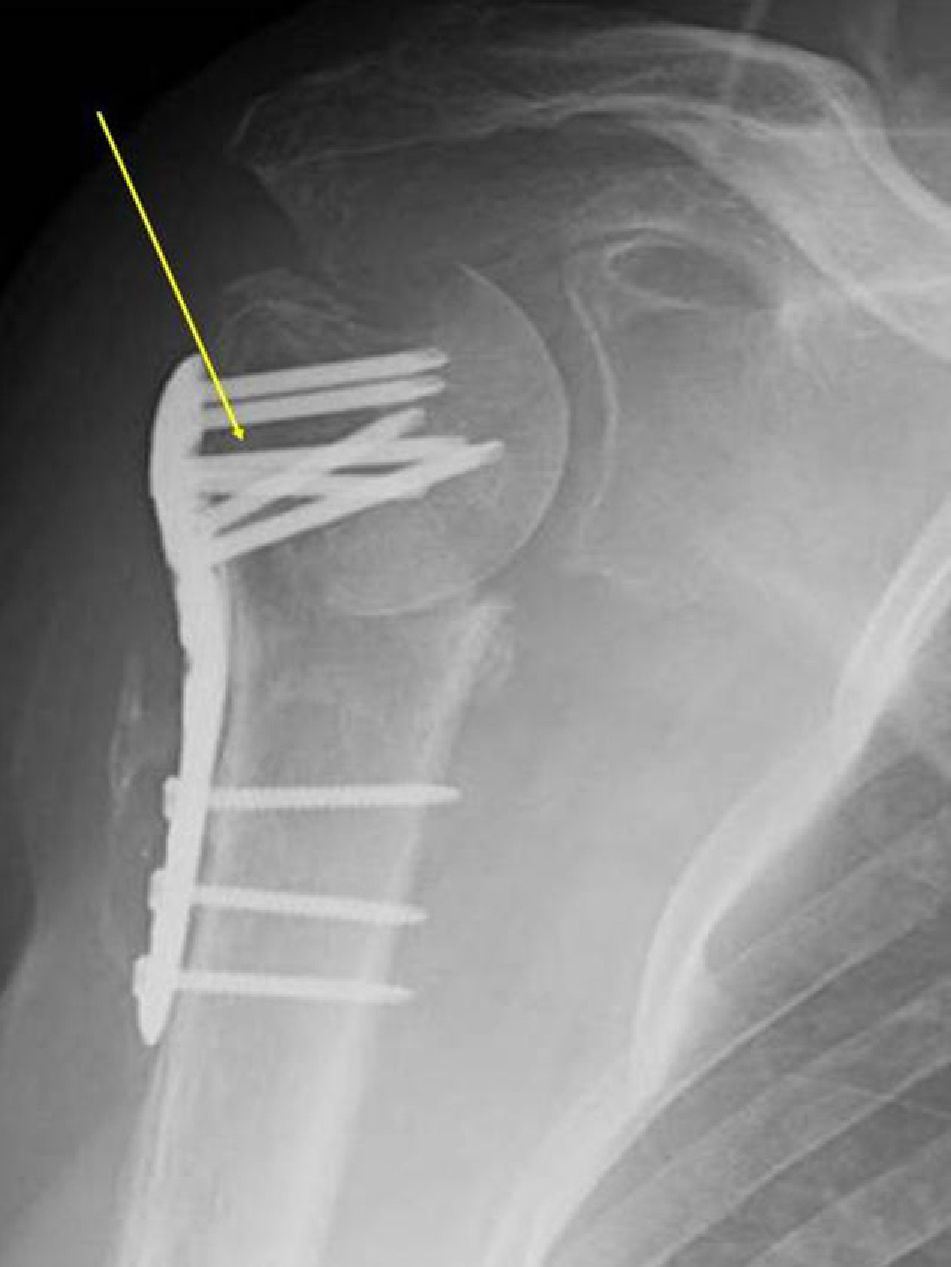
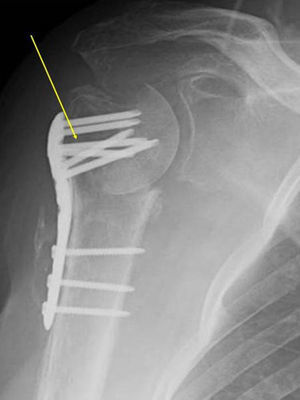
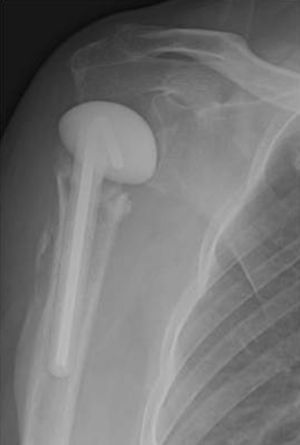
Case PresentationThe patient was a 54-year-old male with liver disease, allergic to penicillin, presenting a proximal humeral fracture with a cervicodiaphysal angle of 80° and a trochiter ascent of 11mm. Pl osteosynthesis was performed with a Philos plate (Synthes®) (Fig. 1). The patient began rehabilitation, with a limited arc (60° of active abduction and 50° of anterior active flexion), fever and wound seroma (ultrasound size: 25mm×12mm), at 2 months and 22 days after the intervention, requiring 2 surgical debridements and the taking of cultures and antibiograms.
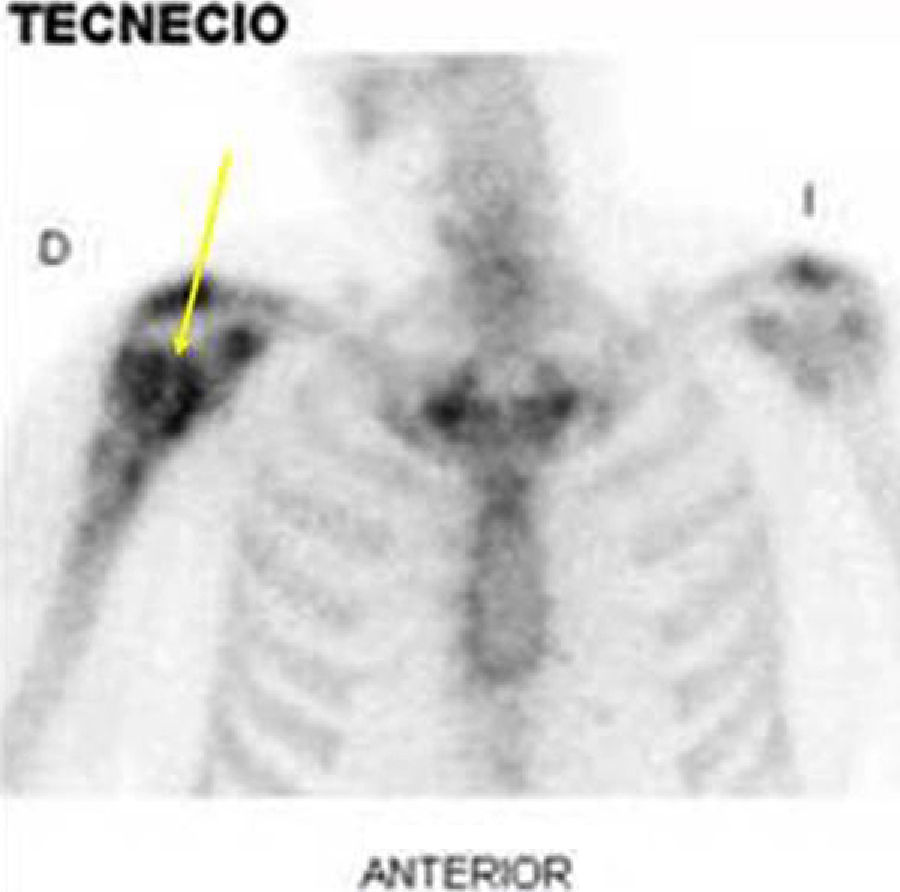
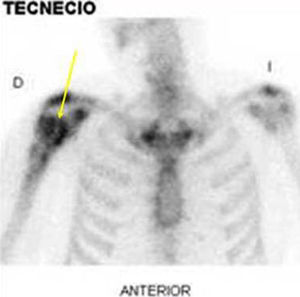
DiagnosisProximal humeral osteomyelitis with stage IV B Cierny–Mader,4 due to coagulase-negative Staphylococcus. Culture antibiogram indicated susceptibility to penicillin, cephotaxime, erythromycin, tetracycline, levofloxacin, and vancomycin cotrimoxazole. Scintigraphic uptake (Fig. 2).
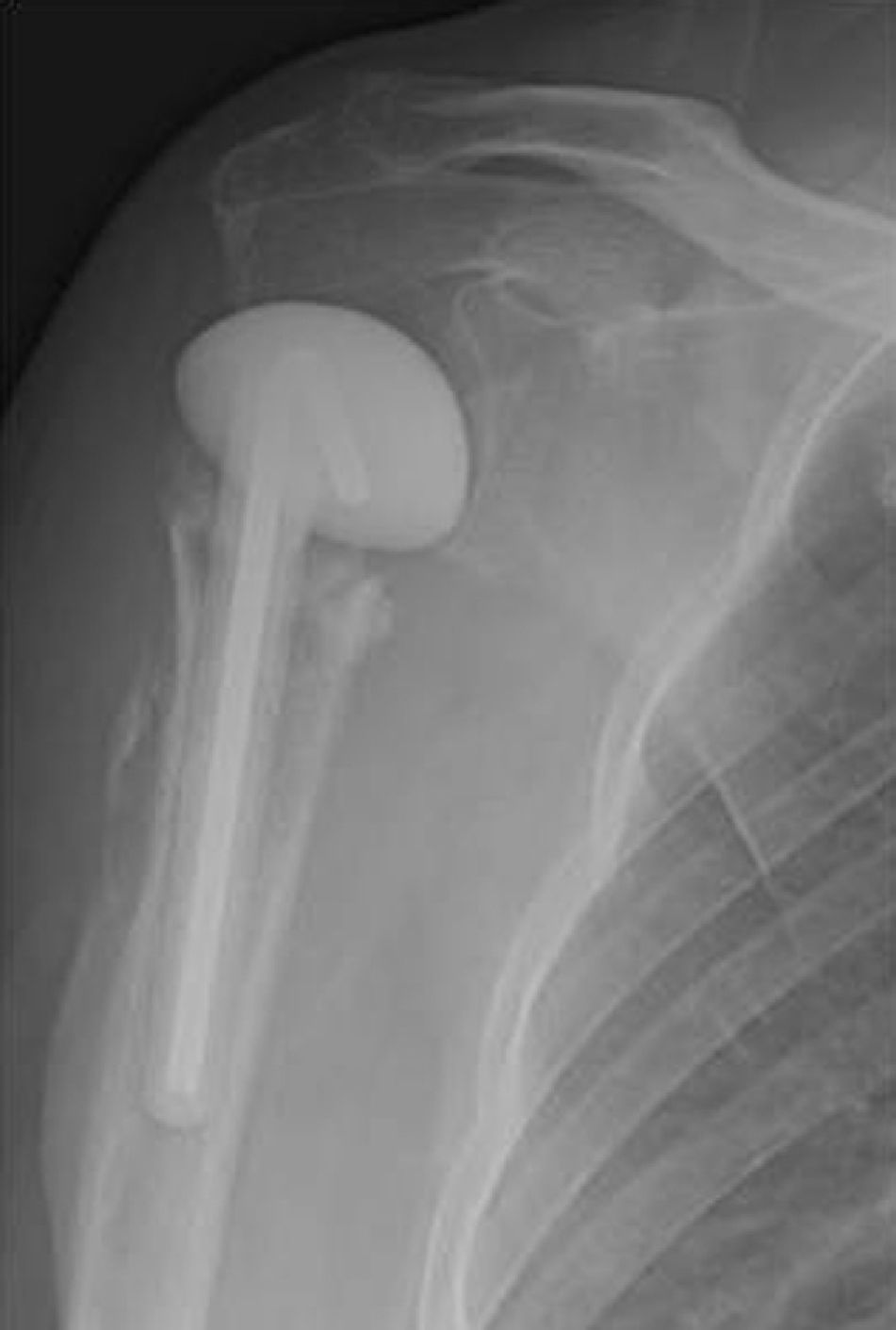
ProgressionGiven the pathogenic agent, the clinical progression and the increased erythrocyte sedimentation rate (ESR: 140mm/h), we removed the material and put a spacer cemented with gentamicin (Fig. 3). We postsurgically started (intravenous (iv)) clindamycin. The patient was under treatment with antibiotics PO: levofloxacin 500mg1/24h vo rifampin 600mg and 1/24h PO for the first 3 months following surgery (considering the sensitivity of the pathogen and the patient's allergy to penicillin). Six months after intervention the infection was controlled (ESR: 17mm/h), with an arc of 100° (flexion/active abduction). The patient refused to undergo withdrawal of the spacer. One year after surgery, the infection remained controlled, with a similar arc.
DiscussionAthwal et al.1 recommend 3.3 surgical lavages to eradicate the infection, achieving 53 points in the American Shoulder and Elbow Surgeons Score (ASES), but recurrences of 50%.5 Seitz et al.6 recommend removing the material, placing a spacer with antibiotics and arthroplasty (although 33.3%3 of patients refuse arthroplasty). Spacers improve the VAS (8.4–0.5 points), for forward flexion (65–110°) and the ASES Score (16–74 points).3 Themistocleous et al.7 recommend keeping the spacer, eradicating osteomyelitis in 81.8% of test with a Disabilities of Arm, Shoulder and Hand (DASH) score of 37.5 points. Stine et al.8 maintain spacers if comorbidity is present, although controlling renal function, due to the risk of kidney failure.3,9
In conclusion, in humeral osteomyelitis cases, placement of a cemented spacer may be an effective treatment for infection control.
Ethical disclosuresProtection of human and animal subjects. The authors declare that the procedures followed were in accordance with the regulations of the responsible Clinical Research Ethics Committee and in accordance with those of the World Medical Association and the Helsinki Declaration.
Confidentiality of Data. The authors declare that no patient data appears in this article.
Right to privacy and informed consent. The authors have obtained the informed consent of the patients and /or subjects mentioned in the article. The author for correspondence is in possession of this document.
Please cite this article as: Jiménez-Martín A, et al. Evolución tórpida tras fractura humeral proximal. Reumatol Clin. 2012. http://dx.doi.org/10.1016/j.reuma.2012.04.005.