Erysipelas is an acute infection of the epidermis and superficial dermis that generally affects the elderly or immunocompromised people.1 The use of biological therapies implies an increased risk of infection, often skin infections,2,3 and therefore it is essential to start antibiotic therapy when suggestive signs appear. We present the case of a woman with psoriatic arthritis who developed facial erysipelas following treatment with secukinumab, which to date has not been described with this monoclonal anti-IL17A antibody.
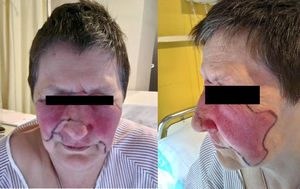
A 61-year-old woman with a history of hiatus hernia and smoker of 30 packs/year until 10 years earlier, diagnosed with peripheral psoriatic arthritis in January 2008, continued treatment with methotrexate from diagnosis to cessation due to dyspepsia (2016), adalimumab (2009–2010) and etanercept (2010–2017), both discontinued due to secondary inefficiency. In February 2017 she started treatment with subcutaneous secukinumab 300mg/month in monotherapy combined with naproxen 500mg/12h and lansoprazol. After 10 months of treatment with secukinumab, 24h after the injection, an erythematous lesion appeared in the left nasogenian sulcus spreading to both cheeks, eyes and dorsum of the nose, with no feeling of dysthermia. She received oral erythromycin for 48h with no improvement. On admission she was in a good general condition, blood pressure 200/98, temperature 37.4°C, and systemic examination was normal. Erythematous lesions on the dorsum of the nose, both malar and periorbital regions, with a well-defined border, were observed, with some blisters on the left side and on the upper lip (Fig. 1). Of note in the blood tests were leukocytes 11.3cell/μl (neutrophils 8.6cell/μl), normal biochemistry, ESR 70mm/h, CRP 3.9mg/dl and procalcitonin<.12ng/ml (normal: 0–.5). Blood cultures were negative. Empirical treatment with intravenous antibiotic therapy with vancomycin and ceftriaxone was initiated, and due to good clinical progress over 48h replaced by amoxicillin-clavulanic acid for 10 days, with resolution of symptoms. To date, the patient, whose articular disease is stable, did not want to restart biological therapy, and methotrexate has been reintroduced.
Erysipelas is an acute superficial cellulitis characterised by the onset of a small erythematous lesion that rapidly spreads and causes inflammation and redness of the dermis with well-defined edges, located in the legs (68%–90%) or face (2.5%–9%).4,5 The infection may progress to bulla formation and necrosis. In up to 40% of cases patients have a systemic disease, and in 78% there is a predisposing factor, among which age and immunosuppression stand out; although there is usually fever and general malaise, 15% are afebrile. Streptococcus is the most frequent aetiological agent, principally group A beta-haemolytic Streptococcus, and Staphylococcus aureus is found in 10%–17%, especially in immunosuppressed patients in whom other types of bacteria can be isolated.4 Diagnosis is clinical, blood cultures are of poor yield, being positive in 5%, and the causative agent can only be isolated by culture of the skin lesions.5 The treatment of choice is penicillin or macrolides in cases of allergy to beta-lactams, although oral or intravenous administration or courses of 5 or 10 days appear to be equally effective in curing and preventing relapses.6 Recurrence is common and up to 29% of subjects have a further episode in the following 3 years, which seems to be more frequent for group C and G Streptococcus.5,6 Treatment with biological therapy involves an increased risk of infection, often in the skin. Recently a case of a woman presenting with erysipelas in the leg following treatment with tocilizumab has been described,7 but in the literature reviewed no cases of erysipelas associated with secukinumab have been described, although in the study by Baeten et al. on ankylosing spondylitis, one of the patients had a subcutaneous abscess of the foot due to S. aureus.8 Erysipelas is an infectious complication that is easily recognisable and treatable, with a good prognosis provided antibiotic therapy is initiated early. The relative frequency of recurrences in a third of subjects must be taken into account due to the greater susceptibility of our patients, especially if they continue with biological therapy.
Please cite this article as: Pantoja Zarza L, Díez Morrondo C. Erisipela facial tras tratamiento con secukinumab. Reumatol Clin. 2020;16:431–432.